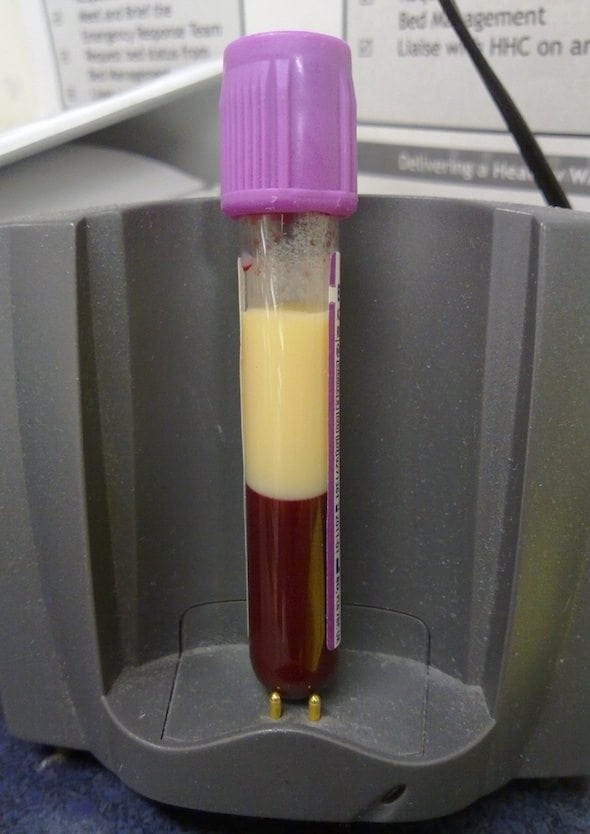
Does fat float on blood?
Your first patient of the drizzly Thursday night shift is Matthew, a man in his 30s, lying on his side on a trolley. He winces as he rolls onto his back to face you, waving aside your apology for his 3hr 47min wait; he’s in obvious discomfort and very happy to see you.
He complains of having constant generalised abdominal pain, slightly worse on the right, gradually increasing over three days.
Things got much worse a few hours earlier, and he vomited several times. You ask if it was dinner that aggravated him, and he shakes his head ruefully, saying he hasn’t so much as glanced at food since Tuesday. He denies urinary symptoms, and diarrhoea, but concedes he hasn’t actually opened his bowels since Monday.
As you glance over Matt’s nursing chart, he mentions that although he’s a smoker, he’s pretty fit and well; he captain-coaches a suburban soccer team and he hasn’t had a drink in several years, since his daughters were born. You note in passing a kind colleague has already prescribed your patient some paracetamol and codeine, and normal saline is charted, but no IV line has been sited.
You note the respiratory rate has been recorded as 14bpm, and decide to carefully watch him while pretending to take his pulse. Over a full minute you note with some surprise his rate is a little higher at 25bpm; you become a bit perplexed when on exam, his abdomen is actually all fairly soft, with only a little localised tenderness above the umbilicus. Despite this he is clearly in marked discomfort.
Not having fully awoken, your coffee half-finished at the computer behind you, and being a bit flummoxed, you decide to order a few tests to play for time. You insert a cannula, and just for a moment wonder about his unusual pale, bright red blood, and then shrug this off. You start the fluid your colleague ordered, add some morphine to his chart, and send him off for plain films of his chest and abdomen while you wander towards the blood gas machine, hoping for an instant answer.
Your tired frustration is further piqued when the blood gas machine complains of an intentionally vague technical error. At this point a trauma call goes out, and you lean the phlebotomy tubes up against a phone charger, and you go to see what the light rain has done to the roads.
You return from the code team some 45 mins later, and drink your icy cold coffee. On the bright side, you think, some answers might have emerged about Mr tummy pain in 23. Unfortunately his x-rays aren’t as helpful as you hoped (not that you were really sure what you were looking for anyway..).
You go to check his bloods, open your mouth to curse yourself for leaving them behind, when you’re interrupted by a nurse. She very kindly noted you were busy, and not seeing any bloods in the computer, sent some more off. Abruptly you change your expletive to ‘f…antastic’ she cuts you off to mention the lab called to say ‘they’d be a while’ because they’re ‘haemolysed or something’. You call the lab, who don’t answer, and then get distracted by the trauma case trying to leap out of his bed and tear off his collar.
Twenty minutes later, you call the lab, still talking with the deliberate and measured tone you’d used with the unfortuanate fellow involved in the MVA, and then to the radiology registrar to explain the mans agitation was new and worrying. To your surprise you’re put through to the senior scientist on call who says ‘Oh, that guy’s serum’s just like milk. It’ll be another half hour or so while I wash the fat out of it. Has he just had a fatty meal or something?’ You say no, and re-iterate he hasn’t eaten for days. Could it, you ask hopelessly, be anything else? ‘Nope. Sorry. It’ll be a while. Do you wanna add on a lipid profile?’ You mumble vague agreement, wondering what you’ll do with that result, exactly.
A moment of inspiration takes you, and you reassess Matthew. He says he feels a bit better, but this time is clearly concerned. You apologise to him, blaming the lab as nicely as possible, and top him up with more morpine. Oddly, he still looks a bit tachypnoeic, and for some reason he’s been put on nasal prongs. You repeat your respiratory exam, and his chest still sounds pristine. Nonetheless the chart shows his oxygen saturations dropped to 88 about half an hour ago.
With resignation you click on another patient, a 46 year old lady with a three month history of vague unwellness. When you go back to the gas machine (on the off chance her potassium is 9.0) you notice the blood you left from the man with belly pain. Your jaw slowly drops as you pick up the EDTA tube, very carefully. At the same time, the lab calls you to say ‘the lipids are back. His triglyceride is 134mmol/L (11,890mg/dL). The LDL will be longer, but it’s high. Oh, and his lipase is 5600U/L.’
You catch the eye of your consultant, on his way home, who glances at his watch, then shakes his head with some amusement. You wave desperately to the senior registrar next to him, who sighs. She patiently listens to the first 19 seconds of your presentation, then becomes slightly interested. ‘Ultimately, he goes to the surgeons, doesn’t he?’ she points out. There is no question in her voice, and you phone the surgical registrar, who sounds bored until you mention the lipase. Your conversation is overhead by the medical registrar, who laughs sarcastically. “The surgeons think that’s caused by the pancreatitis? Morons. It’s the other way around. There’s at most, what, a few hundred mL of fat in a pancreas – if you poured all his blood out, he’d have two litres of fat floating on top. He needs someone to stop him dying of a heart attack at 40.” He adds that incidentally, he doesn’t admit patients with abdominal pain, but he can tee up a formal review to assess him for familial hyperlipidaemias.
Guest post – Dr Mark J Shea
References
- Hypertriglyceridemia – Overview
- Why does hypertriglyceridemia lead to pancreatitis?
- Yadav D. and Pitchumoni C.S. “Issues in hyperlipidemic pancreatitis.” Journal of Clinical Gastroenterology. 2003; 36(1): 54-62.
- Gan S.I., et al. “Hypertriglyceridemia-induced pancreatitis: A case-based review.” World Journal of Gastroenterology. 2006; 12(44): 7197-7202.
- Linares et al. Acute Pancreatitis in a Cohort of 129 Patients Referred for Severe Hypertriglyceridemia. Pancreas. July 2008 – Volume 37 – Issue 1 – pp 13-2
BA MA (Oxon) MBChB (Edin) FACEM FFSEM. Emergency physician, Sir Charles Gairdner Hospital. Passion for rugby; medical history; medical education; and asynchronous learning #FOAMed evangelist. Co-founder and CTO of Life in the Fast lane | On Call: Principles and Protocol 4e| Eponyms | Books |