Guenter Sprotte

Günter Sprotte (1945- ) is a German anaesthetist
Sprotte is best known for designing the Sprotte atraumatic spinal needle, one of the most important refinements in lumbar puncture and spinal anaesthesia since Whitacre. Working in the late 1970s, Sprotte aimed to preserve the principle of the pencil-point needle, separating rather than cutting dural fibres, while overcoming the practical limitations of slow CSF return and injection resistance.
Sprotte’s innovation was an ogival (bullet-shaped) tip with a large lateral “eye” positioned immediately behind the tip, intended to improve CSF flow and mixing while maintaining atraumatic dural entry. The design was formalised in his German patent (filed 1979; granted 1981) and later supported by large clinical series describing the needle as “atraumatic.”
Concerns arose regarding the size and position of the lateral eye, particularly the risk of mechanical fragility and the possibility of partial extradural injection if the orifice straddled the dura. These issues prompted further refinement in the early 1990s, with a redesign documented as of January 1993.
Biographical Timeline
- Born in 1945, Germany
- 1960s–1970s – Medical training in anaesthesiology in Germany
- 1972–2010 – Worked at Universitätsklinik Würzburg; later became head of the pain clinic
- Late 1970s – Develops concept of a modified atraumatic spinal needle to reduce post–dural puncture headache (PDPH), refining the earlier Whitacre pencil-point design
- 1979 – Filed German patent “Stahlkanüle für die Spinal- und Leitungsanästhesie sowie für die Lumbalpunktion” (Steel cannula for spinal and conduction anaesthesia and lumbar puncture)
- November 3, 1981 – Patent granted [DE 3020926 C2]
- 1987 – Published Eine „atraumatische“ Universalkanüle für einzeitige Regionalanaesthesien with Schedel and Pajunk. First formal classification of a spinal needle as “atraumatic”
- 1990 – Experimental confirmation of reduced peripheral nerve trauma with the Sprotte needle design (Reg Anaesth 1990;13:11–15)
- 1990 – Obstetric PDPH study (Cesarini et al., Anaesthesia 1990) demonstrated 0% PDPH in 55 Caesarean patients using 24G Sprotte vs 14.5% with cutting needle
- 1993 – Design refinement: lateral eye moved closer to the tip and shortened to improve CSF flow and structural integrity (as discussed in Regional Anesthesia 1996)
- 1990s–2000s – Widespread international adoption of the Sprotte atraumatic needle in obstetric, neurological, and ambulatory spinal anaesthesia
- 2005 – American Academy of Neurology classifies atraumatic (pencil-point) needles as evidence class I, recommendation level A for reduction of PDPH
- 2009 – Awarded the German Schmerzpreis
- 2010s – Retired
Medical Eponyms
Sprotte spinal needle (1979; modified 1993)
Atraumatic (pencil-point) spinal needle with a rounded ogival tip and elongated lateral opening (“eye”) just proximal to the tip.
- Tip design: Closed, ogival (bullet-shaped) non-cutting tip
- Orifice: Enlarged lateral eye designed to improve CSF return and reduce injection resistance
- Mechanism: Displaces and separates dural fibres (atraumatic) rather than cutting them
- Clinical effect: Reduced incidence of PDPH compared with cutting needles; widely adopted in obstetric and neurological practice
- Design evolution: 1993 redesign moved the eye closer to the tip and shortened it to improve integrity and mitigate safety concerns
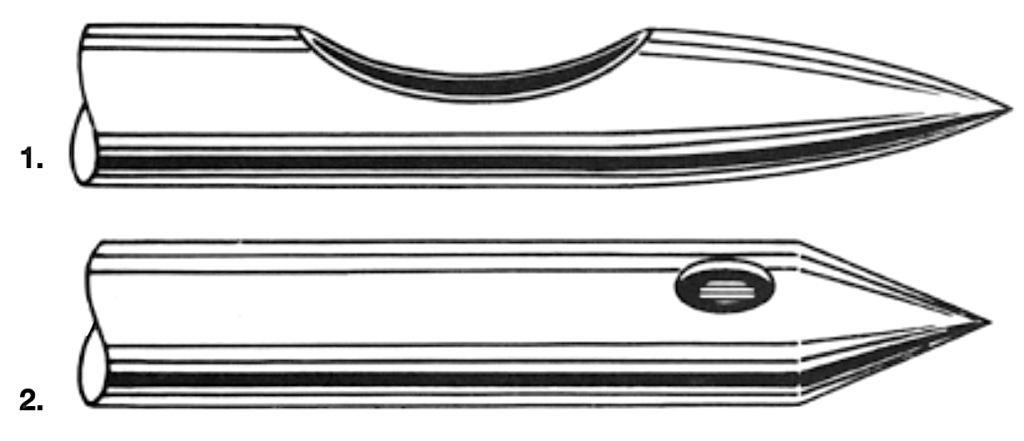
Fig. 2. Tip of the Whitacre cannula: Blunt, closed circular cone with a straight generatrix.
| Feature | Quincke (1891) | Whitacre (1951) | Sprotte (1979) |
|---|---|---|---|
| Tip design | Sharp cutting bevel | Solid conical “pencil-point” with small lateral side-hole | Rounded ogival (bullet-shaped) tip with larger lateral eye |
| Effect on dura | Slices longitudinal fibres → larger persistent defect | Separates fibres → elastic recoil and closure | Preserves atraumatic separation while improving CSF flow |
| CSF flow | Rapid, direct flow | Slower return; more directional flow | Improved flow compared with Whitacre |
| PDPH risk | Higher incidence | Lower incidence | Low incidence (atraumatic class) |
| Design evolution | Original cutting needle | First widely adopted atraumatic design | Modified eye position/length in 1993 to improve strength and safety |
Clinical Evidence – Atraumatic Performance
Early clinical series supported the classification of the Sprotte needle as “atraumatic,” with markedly reduced rates of post–dural puncture headache (PDPH) compared with cutting needles.
In an obstetric spinal anaesthesia study (Caesarean section), PDPH occurred in 8 of 55 patients (14.5%) using a cutting (diamond-tip) needle, compared with 0 of 55 patients (0%) using a 24G Sprotte needle. [Cesarini 1990]
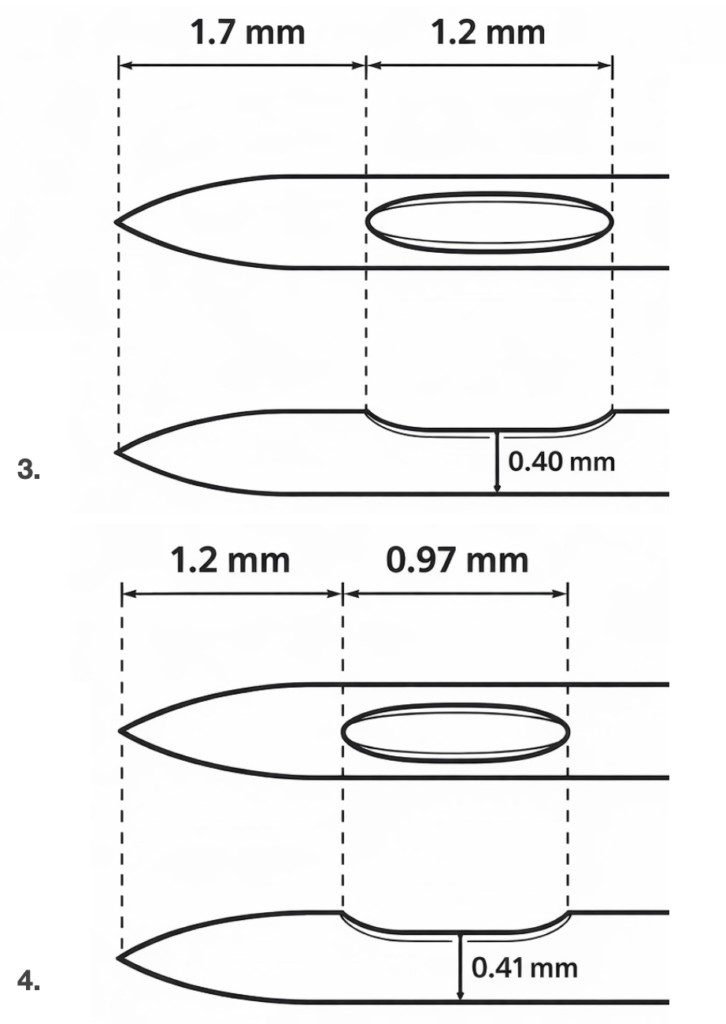
Subsequent engineering analyses examined whether the large lateral eye was necessary for CSF flow and raised concerns regarding tip strength and the potential for partial extradural injection if the orifice straddled the dura. These findings prompted refinement of the design in 1993, with repositioning and shortening of the eye to improve structural integrity and injection behaviour.
Major Publications
- Pajunk H, Sprotte G. Stahlkanüle für die Spinal- und Leitungsanästhesie sowie für die Lumbalpunktion 1979 Patent
- Sprotte G, Schedel R, Pajunk H, Pajunk H. Eine “atraumatische” Universalkanüle für einzeitige Regionalanaesthesien. Klinische Ergebnisse nach sechsjähriger Erprobung bei über 30,000 Regionalanaesthesien [An “atraumatic” universal needle for single-shot regional anesthesia: clinical results and a 6 year trial in over 30,000 regional anesthesias]. Reg Anaesth. 1987 Jul;10(3):104-8.
References
Eponymous terms
- Cesarini M, Torrielli R, Lahaye F, Mene JM, Cabiro C. Sprotte needle for intrathecal anaesthesia for caesarean section: incidence of postdural puncture headache. Anaesthesia. 1990 Aug;45(8):656-8.
- Aglan MY, Stansby PK. Modification to the Sprotte spinal needle. Anaesthesia. 1992 Jun;47(6):506-7.
- Currir DS, Bevacqua BK. Sprotte spinal needle: a new design. Reg Anesth. 1996 Mar-Apr;21(2):172-3.
- Calthorpe N. The history of spinal needles: getting to the point. Anaesthesia. 2004 Dec;59(12):1231-41.
- Boulton T. Spinal anaesthesia during the 19th and 20th Centuries – cocaine and controversy. Anaesthesia News Digital, April 2021
Eponym
the person behind the name
BA Medical Sciences, BMBCh University of Oxford. Pursuing a career in critical care in WA. Passionate about medical education. When not in the hospital often hiking/camping/cycling through the great outdoors.
BA MA (Oxon) MBChB (Edin) FACEM FFSEM. Emergency physician, Sir Charles Gairdner Hospital. Passion for rugby; medical history; medical education; and asynchronous learning #FOAMed evangelist. Co-founder and CTO of Life in the Fast lane | On Call: Principles and Protocol 4e| Eponyms | Books |

