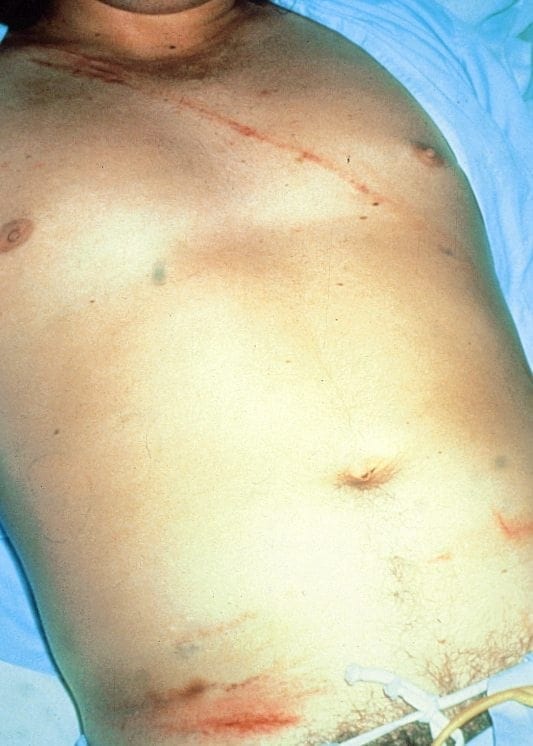
Approach to the High Risk Blunt Trauma Patient
- Gibbs, M. & Winchell, R. (2011). High Risk Scenarios In Blunt Trauma: An Evidence-Based Approach. EM Critical Care. (Vol. 1, Num.3.)
The focus of this article tackles the 3 big presentation’s in the blunt trauma patient from the blunt aortic injury,to the pelvic ring fracture and finishes of with a look at blunt abdominal injury.
Questions
Q1. What is the initial approach towards the blunt trauma patient?
Answer and interpretation
- Step 1: Effectively manage the airway and optimise oxygenation.
- Step 2: Identify and control immediate threats to central perfusion.
- Step 3: Identify and address severe intracranial injuries.
- Step 4: Identify and control other potentially life-threatening thoracic and abdominal injuries.
- Step 5: Identify and control potentially limb-threatening injuries.
- Step 6: Identify and treat noncritical injuries.
Q2. How do you define shock in the blunt trauma patient?
Answer and interpretation
From a physiological standpoint, shock results when oxygen delivery is inadequate to meet tissue demands.
Key points in treating shock are:
The correct approach to treating shock is to restore tissue perfusion rather than to simply achieve a higher systolic blood pressure.
- The presence of shock should never be simplistically equated with a systolic blood pressure reading<90mmHg.
- The recognition of clinical shock requires complex integration of numerous data points including the mechanism of injury and patient’s overall appearance, vital signs , level of mentation, peripheral perfusion and urine output.
- These clinical parameters alone do not adequately quantify the degree of shock or the response to shock therapy. This principle is especially pertinent in elderly patients and in those with limited cardiovascular reserve.
- In severely injured blunt trauma patient, clinical parameters should be coupled with objective makers of tissue perfusion eg, serum lactate or base deficit).
Q3. What are the causes of haemorrhagic and non-haemorrhagic shock in the trauma patient?
Answer and interpretation
Haemorrhagic:
- External bleeding
- Haemothorax
- Haemoperitoneum
- Retroperitoneum (pelvic fracture/renal injury)
- Long bone fracture
Non-Haemorrhagic:
- Tension pneumothorax
- Pericardial tamponade
- Myocardial contusion
- spinal cord transection/injury
- Coincident medical event (cardiac event, GI bleed, vasoactive medications)
Q4. Name 4 options for bedside testing and indicate their utility in the hypotensive trauma patient?
Answer and interpretation
1. Chest radiography:
- Look for tension pneumothorax or massive haemothorax.
- Is there evidence suggestive of aortic injury?
2. Pelvis radiography:
- Is there pelvic ring disruption?
3. Focused assessment with sonography for trauma (FAST) Is there sonographic evidence of:
- Pneumothorax?
- Haemothorax?
- Haemopericardium?
- Haemoperitoneum?
4. Diagnostic peritoneal aspiration (DPA):
- Is there haemoperitoneum?
Q5. What are the goals of optimising resuscitation in the blunt trauma patient?
Answer and interpretation
- The determination that a trauma patient is “in shock” is a complex one, and it is not always synonymous with a systolic blood pressure <90mmHg.
- The accurate diagnosis of the cause(s) of shock begins with a targeted physical examination and the thoughtful use of diagnostic testing (including chest radiography, pelvis radiography, and ultrasound). The use of objective serum makers of tissue perfusion (eg. serum lactate or base deficit) can be helpful in identifying “subclinical” shock and in following the patient’s response to resuscitation.
- In patients requiring massive transfusion (defined as the administration of > 10 U of PRBCs in 24 hours), institutional protocols defining blood product ratios have improved outcomes. When massive transfusion is employed , use of PRBC to platelet to FFP ratio of approximately 1:1:1 may result in decreased need for blood products. (Remember to give calcium as well in patients requiring massive transfusion to prevent citrate toxicity).
Q6. What are the key point to managing a blunt aortic injury?
Answer and interpretation
- A blunt aortic injury is a potentially lethal injury that should be considered in all blunt trauma patients who experience major deceleration, including motor vehicle crashes, automobile-versus-pedestrian injuries, and falls from a significant height.
- A CT scan is the current criterion standard in the diagnosis of BAI. Although TEE can be useful,although it is operator dependent.
- Chest radiography is a useful screening tool in then diagnosis of BAI. In large trials, the most important radiographic findings suggestive of BAI were: (1) widening of the mediastinum (>8cm), (2) blurring of the aortic knob, and (3) loss of aortopulmonary window.
- A BAI seldom occurs in isolation. A diligent search for other potential causes of shock and time-sensitive conditions is essential.
- In the setting of BAI, other causes of ongoing haemorrhage and/or neurosurgical lesions should be rapidly identified. Management of these conditions often’s requires thoughtful staging of interventions and is best done in experienced trauma centers.
Q7. What the key points to managing a pelvic ring fracture?
Answer and interpretation
- Pelvic ring fractures are a sign of major energy transfer and should be viewed as markers of potentially severe multisystem trauma.
- Pelvic ring fractures can be classified as: (1) lateral compression injuries, (2) AP compression injuries, or (3) vertical shear injuries. Classification is helpful to predict risk of ongoing haemorrhage. Fractures that increase pelvic volume 9ie, AP compression injuries and vertical shear injuries) pose the highest risk of ongoing bleeding.
- Institutional protocols that incorporate stabilisation, aggressive resuscitation, and early definitive therapy improve outcomes.
- For community physicians, the essential steps are to : (1) recognise pelvic injury pattern on plain film, (2) institute aggressive resuscitation early, (3) employ external pelvic stabilisation when pelvic fracture patterns lead to increased pelvic volume, and (4) orchestrate timely transfer to a trauma centre.
Q8. What are the key points to managing blunt abdominal trauma?
Answer and interpretation
- In the haemodynamically unstable blunt trauma patient, ultrasound is the study of choice for the initial evaluation for haemoperitoneum.
- Persistent or recurrent hypotension in the patient with haemoperitoneum is an indication for immediate laparotomy.
- Computed tomography managing provides valuable information in patients who stabilise with resuscitation and assists with injury staging and planning for definitive management. The most common injuries are to the liver and spleen, and many of these injuries can be managed non-operatively in patients without hypotension or ongoing transfusion requirements.
Emergency nurse with ultra-keen interest in the realms of toxicology, sepsis, eLearning and the management of critical care in the Emergency Department | LinkedIn |