Basic Life Support
The most recent BLS 2015 guidelines (ILCOR 2015) retain many of the 2010 recommendations, again reinforcing the chain of survival. However, there is an increased emphasis on simplification of compression method, good quality bystander CPR and encouragement thereof, dispatcher guided CPR and early defibrillation.
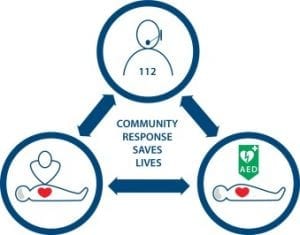
Fig. 2.1 The interactions between the emergency medical dispatcher, the bystander who provides CPR and the timely use of an automated external defibrillator are the key ingredients for improving survival from out of hospital cardiac arrest (ERC guidelines).
Fig. 2.2 The chain of survival. (ERC guidelines)
Specific Elements of BLS:
Main resource used: ANZCOR (Australia and New Zealand Committee on Resuscitation) as this is the most relevant local guideline for the ACEM. Some of this seems a little obvious but it is often the assumed basic knowledge that we forget or don’t know as well as we think. These are guidelines for all comers.
DRS ABCD as an aid memoir
Dangers: Check for scene safety – overhead powerlines, road side etc. etc.
Responsiveness: Call out, stimulate patient, assess for signs of life for 10 seconds (no signs of life include – no movement, unconscious, no signs of breathing or abnormal breathing – experienced providers may include a carotid pulse check but this is not required)
Send for help: Delegate this role to a person to call emergency services and get back to you. Request them to find you an AED if available. Remember the relevant number for your country – 000 Australia
Airway:
- Airway management takes precedence over any other injury including spinal.
- Ideally leave the victim in the position they are found unless they are demonstrating signs of an obstructed airway – gentle handling at all times if they must be moved.
- To clear the airway – open mouth and turn head to allow drainage
- If airway becomes compromised in resuscitation roll onto side to allow clearance and then reassess for responsiveness.
- Remember your airway opening manoeuvres – head tilt chin lift in adults, neutral position in infants.
Breathing:
Causes of ineffective breathing include – central causes (e.g. opiates, brainstem injury)/ acute upper airway obstruction / chest wall paralysis or diaphragmatic paralysis / intrapulmonary cause / drowning / suffocation.
Principles in BLS – Look, listen and feel for effective breathing for 10 seconds – if absent declare cardiac arrest. Caution with agonal breaths or see saw breathing where there is a partial obstruction.
Rescue breath technique:
- Open the airway using head tilt chin lift manoeuvre or jaw thrust
- Place mouth over open mouth with nostrils pinched (with care not to lose tilt).
- Give one breath of 1 second duration to give adequate volume to give chest rise
- Causes of failure – obstruction, insufficient air or poor seal
- Alternative methods include: mouth to nose (operator choice, infants, trismus), mouth to mask, mouth to neck stoma.
Circulation / Compressions:
- Compressions should be started in BLS protocol if victim is unresponsive and has abnormal breathing including agonal respirations. Pulse check is no longer required though it can be done if trained and comfortable to do so.
- Bystander CPR is actively encouraged and should be coached
- Recommended ration remains 30:2 – ARC recommends for all ages though other resources suggest 15:2 in paediatrics. This is a BLS recommendation for simplification. If an expert is present do a ratio of 15:2 in children.
- Compression only CPR is also an option – see links below demonstrating
- All rescuers should perform compressions and if trained and willing, they should be encouraged to provide rescue breaths.
- Paediatric arrests are often hypoxic therefore if there are two people 15:2 should be encouraged and rescue breaths should in particular be encouraged. Consider further rescue breaths prior to going for help
- Location: lower half of the sternum – consensus for simplicity (lower ineffective with risk of visceral injury, higher will be ineffective)
- Rate: 100-120 BPM “Staying alive”
- Depth: Adult: 5cm (2inches) to max of 6cm. Paediatric: 1/3rd of depth or 4cm infants, 5cm children
- Allow for chest recoil and avoid leaning on the chest
- Minimise interruptions
- Multiple rescuers – rotate roles – evidence would suggest fatigue of compressor at around 1 minute though only realised by compressor at 5 minutes. Guidelines suggest rotation every 2 minutes. Ensure early help and early access to AED as priority.
- Early defibrillation remains a priority: Defibrillation within 3-5 minutes can produce survival rates as high as 50-70%.
- Continue compressions post defibrillation – the AED will generally prompt you.
- Pulse checks in BLS are not recommended. Rescuers can look for signs of life every 2 minutes / rhythm check if AED prompts you (AED generally has a 2 minute timer between rhythm checks)
Defibrillation:
AED training is generally required. The machine verbally talks the rescuer through the process of its use when the power button is activated. Pads placement is demonstrated in pictures on the back of them. The end cable from the pads is inserted into the AED.
The AED will announce that it is analysing the rhythm and will request hands off the patient i.e. to cease compressions and to stand clear. It will advise if a shock is required or not.
Should a shock be required the AED will charge and deliver this shock. The rescuer’s priority is to maintain scene safety and to ensure all other parties stand clear of the activated shocking defibrillator. Chest compressions must be resumed after a shock is delivered or if no shock is advised.
Advanced discussions / concerns:
BLS duration: continue until the patient responds / you are unable to continue / a health care professional arrives and takes over care or directs cessation
Risks:
- Is there a risk to the victim if they are not in cardiac arrest and they receive chest compressions? The consensus guideline was based on low quality evidence but a high level recommendation. ILCOR argue on a risk benefit basis that the risk of omitting CPR to those in cardiac arrest is greater than causing injury to the non-arrested patient. Observational studies on those who received CPR in the absence of cardiac arrest report a low degree of complications.
- Is there a risk to the rescuer? There is a documented low-risk of disease transmission based on a systematic review done in training and clinical scenarios. However there is some suggestion that using barriers such as face mask reduce bacterial transmission to the rescuer therefore if available this is recommended.
Exam relevance examples:
OSCE: Teaching a bystander / medical student or intern BLS or coaching a bystander over phone.
OSCE: Educate a staff member how to operate an AED
OSCE: Instruction in SIM scenario and identification of inadequate or incorrect techniques.
MCQ : Written question
Videos:
Reveal BLS Videos
ERC BLS demonstration video including AED – Putting it all together:
Opening an airway:
Assessing breathing and rescue breaths: ProCPR ** Pulse check is included in this video if trained**
Reveal Compression only CPR
Australian Style: ARC
American Hangover Style: AHA
CPR 30:2 ProCPR
External Resources
Last ILCOR CoSTR guidelines 2015 resulting in
- ANZCOR (Australia and New Zealand Committee on Resuscitation)- https://resus.org.au/guidelines/
- ANZCOR Guideline 4 – Airway- January 2016
- ANZCOR Guideline 5 – Breathing- January 2016
- ANZCOR Guideline 6 – Compressions
- ANZCOR Guideline 8 – Cardiopulmonary Resuscitation- January 2016
- Guideline 10.1 – Basic Life Support (BLS) TrainingMarch 2013
- AHA (American Heart Association)
- http://circ.ahajournals.org/content/132/16_suppl_1/S51 CoSTR 2015
- https://eccguidelines.heart.org/index.php/circulation/cpr-ecc-guidelines-2/
- ERC (European Resuscitation Council
- http://ercguidelines.elsevierresource.com/european-resuscitation-council-guidelines-resuscitation-2015-section-2-adult-basic-life-support-and CoSTR 2015
- http://www.cprguidelines.eu/
(Evidence for each recommendation is discussed within above guidelines including references. In particular, the AHA / ERC CoSTR publications discusses detailed evidence for each recommendation, knowledge gaps using a PICO format and provide reference back to older items discussed in prior guidelines)
Special Circumstances:
- Foreign body / Choking
- Paediatrics
- Pregnancy
- Drowning
Tá gaeilge agam. Irish doc, ED FACEM in Oz. Into trauma, resus, cardio & tox! Chase gaelic footballs, dive, hike, run & rock in spare time! | @unanici |