Button Battery Update 3.0
Button battery ingestion is one of the leading causes of death in paediatric poisoning and this has risen sharply from 2016 despite manufacturing warnings. More recently Duracell has devised batteries with a bitterant coated ring which they claim discourages swallowing. However, the bitterant is on their larger batteries and only on one side of the battery. In addition, not everyone can taste bitter, and there is no evidence that it reduces the incidence of ‘one gulp’ poisonings. In fact, it was not helpful when added to antifreeze (another one gulp poison) to discourage poisoning. See Poison.org Button Battery stats
Usefuly, ‘The bitter taste layer on the Duracell cell is non-toxic and completely harmless if consumed’.
Which is more than one can say for the battery!
What makes button battery ingestion more frightening is the fact that the ingestion may go unwitnessed, the child may have vague symptoms like being ‘off food’ and later devastating haematemesis can result from erosion of the battery through the oesophagus and into the thoracic aorta.
Peer reviewer Dr Ruth Barker, Director, Queensland Injury Surveillance Unit and Emergency Paediatrician, Queensland Children’s Hospital, Brisbane.
Mechanism of injury
Bridging of the electrodes (the small rim along the edge of the battery) allows residual battery charge to generate current.
The current causes hydrolysis of H2O generating hydroxide ions at the negative pole. Hydroxide ions are essentially oven cleaner! This accumulation of hydroxide produces a localised alkaline corrosive injury with tissue liquefaction and necrosis (remember aLkaLine caustics lead to Liquefaction necrosis). Hydroxide production starts immediately. Corrosive injury and perforation of the oesophagus can occur within 2 hours of lodgement and can continue even after the battery is removed. The severity of injury is all dependent on the size of the battery, current produced, length of time and location where it is lodged. Complications include oesophageal perforation, tracheal-oesophageal fistula, aorta-oesophageal fistula and stricture formation.
Remember the 3 ‘N’s – Negative – Narrow – Necrotic
The negative battery pole, identified as the narrowest side on the lateral x-ray, causes the most severe, necrotic injury.
Resuscitation
- Rarely required acutely. Choking is transient. An ingested battery is usually swallowed.
- Need to consider airway obstruction but battery inhalation very rare.
- Stridor (‘croup’)/ vocal cord paresis can result from high oesophageal lodgement.
- Delayed presentations may result in cardiovascular collapse from haemorrhage or sepsis and should be managed along conventional lines.
- Oesophageal bleeding due to a battery warrants urgent cardiothoracic surgical discussion.
Risk Assessment
Battery age and chemistry
- A spent battery is less likely to cause as much damage. 1.2V is required to generate hydrolysis. A 3V battery has a 10 year shelf life and when spent still has 1.5V so is capable of causing lethal injury even when no longer working in the product.
- Lithium batteries hold their charge for longer (and make up the majority of the large (20mm) 3V batteries on the market). But a battery of any chemistry with > 1.2V can cause hydrolysis.
- Zinc air batteries (most small hearing aid batteries) rely on oxygen to generate charge and are mostly a problem in ears and noses.
- All batteries should be considered active and removed promptly, because you never know what is inside the child!
Battery Size
- Batteries of <20 mm are less likely to lodge in the oesophagus and cause complications (although ‘relatively bigger’ batteries in small children increases risk despite being <20 mm).
- Batteries >/=20 mm are usually the ones getting stuck in the oesophagus and can cause severe local damage within 2 hours.
- Smaller batteries can also cause localised damage when placed in aural or nasal cavities/ elsewhere (vagina, eyelid, under plaster cast). Actually, any battery, like a AA, can cause this damage they are just not as easy to ingest or insert.
Age and time of presentation
- Age is a risk factor. Most fatalities occur in the under 4 year old age group.
- Peak age for ingestion is 1-2 years.
- Non-mobile infants have been fed batteries by siblings.
- Autistic children can have a prolonged oral phase and even the elderly can mistake batteries for tablets.
- Most injured children are pre- or non-verbal.
- Delayed diagnosis has a worse outcome.
- Where oesophageal injury is established, perforations and fistulas may not be evident for up to 28 days.
- Liquefactive necrosis can persist post battery removal. Strictures take weeks or months to form.
- A battery can cause damage when lodged in the oesophagus then pass. Best to treat oesophageal bleeding as battery damage until proven otherwise!
Clinical features
When to suspect an ingestion
- Observed (sometimes by a sibling) or overheard choking episode.
- Finding products that do not work because the battery is missing.
- Finding evidence of packet or product tampering.
Symptoms
- Ingestions that do not result in impaction are often asymptomatic once the battery has been swallowed.
- In unwitnessed or unsuspected, button battery ingestion, presentations can be delayed.
- Where oesophageal impaction occurs, signs and symptoms are non-specific and may include:
Early (caused by obstruction): note obstruction can be partial.
- Unexplained vomiting or food refusal (sometimes tolerating soft foods and able to vomit back past the partial obstruction)
- Drooling or regurgitation of food. Regurgitation is a reasonably specific indicator of oesophageal obstruction.
In the next few hours to days (caused by burning and inflammation)
- Croup-like symptoms (if the battery is near the larynx)
- Chest/ abdominal pain (sometimes this presents as grunting). Grunting is another reasonably specific marker of chest or abdominal pathology. Should trigger a CXR.
- Unexplained fever
Late signs due to erosion through to other organs
Lungs
- Coughing or choking with feeds
Major vessels or heart: oesophageal bleeding
- Vomiting blood (sometimes this can be vomited through the nose). Blood can be altered (coffee ground) or if bleeding is arterial and brisk, fresh red blood.
- Melaena or heamatochezia.
Spine
- Pain and limitation of movement
Gut
- Abdominal pain/ vomiting/ fever: gut perforation rare but reported in Meckels
Insertions
Damaging but less time-critical.
- Unexplained nasal, ear, rectal, vaginal or eye discharge/bleeding – these batteries can be stuck in many places; even under plaster casts. While we say less time-critical there are case reports of children going deaf from a battery stuck in the ear – be vigilant.
Immediate Care
Routine care for the paediatric patient
- Analgesia.
- Keep nil by mouth until a full assessment is made.
For oesophageal impaction:
- First aid advice includes administration of honey or jam (check your local recommendations)
- Honey: If < 12 h post ingestion and > 12 months of age (botulism precaution), 10ml every 10 min.
- Jam could be used in under 12 months
- Not all children can tolerate.
Investigations
Specific: URGENT: Plain anteroposterior X-ray of the neck, chest and abdomen (need a lateral chest X-ray if an object is identified above the diaphragm).
- Think ‘neck to bottom’ X-rays for all GI bleeding and suspected FB ingestion, or a history of epistaxis but no bleed point identified.
- Skull X-ray if you suspect a nasal placement.
- Abdominal if rectal or vaginal insertion is considered.
Do not mistake a button battery for a coin – (54% of fatalities are due to mis-identification) the battery should have a:
- “Double ring” appearance on PA (most of the time – absence of a double ring does not exclude the diagnosis -see below)
- “Step off” appearance on lateral view (most of the time – see X-rays below for when this may still be absent).
See an example clinical case below and the differences between a button batteries versus a coin on X-ray. From ‘A second Look at a Coin in the Stomach – Radiology Cases in Paediatric Emergency Medicine Vol 2 Case 9’ (click on images for full link of go to DFTB):
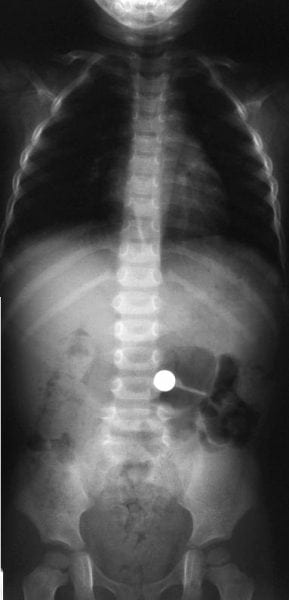


This lineup above shows a radiograph of a series of 6 disc batteries and a dime.
- The first disc battery on the left has the positive terminal facing toward us.
- The second battery from the left has its negative terminal facing toward us. On this second battery, the black plastic insulator is visible in the photograph. However, the radiograph of both the first and the second disc batteries show the internal ring sign of the plastic insulator.
- The fourth battery from the left also shows a plastic insulator, but the radiograph of this battery does not show the internal ring (‘windowing’ on your pacs system may help). It could be absent because the battery casing is thicker than the first and second batteries. Thus, the absence of the internal ring radiographically does not rule out a disc battery since the appearance of the internal ring is highly dependent on the degree of X-ray penetration, the angle of the battery, and the thickness of the battery casing.
- The third and fifth batteries from the left are viewed from the side. On its side view, the battery has a rectangular appearance with a bulge on one end. This bulge represents the negative terminal of the battery as shown in the corresponding photo below it. The radiographic shadow also identifies this bulge which can be described as frosting on the cake (bilaminar appearance).
- However, this radiographic sign may be absent if the battery is oriented obliquely, or if the battery is very thin (see battery on the extreme right). The dime has only be radiographed PA and is the object 6th from the left.
- See radiopedia for more examples.
Decontamination
- Batteries in the oesophagus should be removed within 2 hours of ingestion endoscopically (ENT of gastroenterology/ both).
- Impacted batteries can be difficult to dig out and sometimes rigid scopes (ENT usually) are more effective.
- Bleeding or delayed presentations warrant involvement of cardiothoracic team
- Ingested batteries not in the oesophagus but causing symptoms require discussion with surgical team. DO NOT give aperients (can cause a septic shower).
- Batteries under the eyelid, in the nose, ear vagina or rectum require urgent removal. Expert advice may be required from ENT/ other specialty team.
Disposition
Battery in the oesophagus requires urgent endoscopy for removal.
If the battery is in the stomach, the risk of complication is low, TOXBASE in the UK states that a repeat x-ray should be done in 2 days if the child is asymptomatic (4 days in USA). If it has not moved at this stage, discuss with your upper GI surgeon or endoscopy team, most will remove the battery from the stomach if it has been there for a maximum of 4 days.
If the battery is beyond the pylorus and the child is asymptomatic, they can be discharged and observed at home for a repeat X-ray in 10 – 14 days if the battery has not been observed in the stool (I think most parents would go for a repeat x-ray as opposed to sifting through 2 weeks worth of poo). Once the battery is beyond the pylorus it is very unlikely they will develop any complications. However, parents should be advised to return if any symptoms. There have been rare reports of batteries becoming lodged in Meckel’s diverticulae/ causing gut perforation.
If discharging the patient give parents the advice to return if: they are concerned; the child develops abdominal pain; bloody vomit or faeces; problems swallowing; respiratory distress; or a persistent cough.
Systems Issues
Protocol for triage and investigation – some departments have set protocols which you may wish to adopt: patients are triage 2 and the radiology form only states ‘?button battery’. This then sets in motion an appropriate X-ray series.
Educate staff on common pitfalls in image interpretation, presentation and cognitive bias e.g. fixating on a diagnosis of epistaxis when no bleed point is seen or assuming because the child is vomiting or eating that there can not be an oesophageal foreign body.
Find out now who your go to is, can you get an X-ray if you are rural and who can remove the battery (is it ENT or Gastroenterology). These decisions need to be made in advance, ‘no bun’ fights at 0200). Your local ENT/Surgical/Gastroenterology team are a good first start. Finally, discuss honey/ jam as first aid, especially for longer retrievals.
- Devise own local algorithm – see Dr Litovitz’s example below and adapt as approved by local teams.
- See departmental and patient resources below for some excellent videos from Kidsafe QLD.
- When these cases go wrong, they go spectacularly wrong. See lessons in this paper.
Recent changes to treatment
See algorithm below from NBIH their current advice includes honey:
- Pre-hospital: administer 10ml (2 teaspoons) of honey every 10 minutes (max 6 times) if the child is over 12 months of age, less than 12 hours since ingestion and the child can swallow (while getting to the hospital, don’t stop off at the shops). A recent paper from NSW shows jam also effective and does not carry the botulism risk for <12 month olds.
- In the OR: If no endoscopic evidence of perforation, irrigate injured area with 50-150ml 0.25% sterile acetic acid to neutralise residual alkali.
Jatana et al have done a series of experiment on piglet oesophagus and then in live piglets to demonstrate the neutralising effect on the alkaline damage.
Prevention
A near miss presentation is an opportunity to discuss poisoning prevention with families:
- Divest of button battery operated devices; recycle electronics and don’t donate them.
- Boycott purchasing new devices with button batteries.
- Don’t accept button battery operated ‘freebies.’
- Safely recycle spent button batteries by taping them with clear sticky tape as soon as they are removed from the device. Store out of reach in a non-airtight glass container (fire resistant) and take to a recycling centre.
- Taping also reduces hydroxide production if the battery is swallowed.
- For essential button battery operated products, ensure that they are durable and have a child resistant battery compartment.
- New button batteries need to be in child resistant packaging.
Advocacy
This devastating injury is on the rise as more and more small electronic devices are produced. Ultimately, we need to design out the hazard through safer button batteries or a move to alternative power.
In the meantime, advocacy has resulted in regulatory changes in Australia and subsequently the US aimed at reducing unintended access to button batteries by young children.
Regulations require button batteries to be sold in child resistant packaging and for products that run on them to be durable and have child resistant battery compartments.
There are teams devising new button battery designs that prevent current flow so the battery remains inert within the body when ingested or inserted.
But commercialisation takes many years and the button battery companies are not on board.
Duracell’s bitterant coated battery is unlikely to deter ingestion. The bitterant is only on one side of the battery and genetically determined ability to taste bitter varies in different populations. It may stop some ingesting more than one, but remember, kids eat dog poo!
Make some noise!
Further reading
FOAM resources
- McGrath C. Ingesting Foreign Bodies at DFTB17. DFTB
- Tagg A. Ingested Foreign Bodies. DFTB
- Foreign body ingestion – RCH
- Long N. Toxicology library. LITFL
- Fox SM. Button Battery Ingestion. Pediatric EM Morsels
- Disc batteries – who and what do I X-Ray?. Queensland Injury Surveillance Unit
- Button batteries. ACCC product safety
- What happens when a button battery is ingested? A chicken fillet and button battery
References
- Jatana KR, Litovitz T, Reilly JS, Koltai PJ, Rider G, Jacobs IN. Pediatric button battery injuries: 2013 task force update. Int J Pediatr Otorhinolaryngol. 2013 Sep;77(9):1392-9
- National Capital Poison Centre Button Battery Ingestion Triage and Treatment Guideline.
- Litovitz T, Whitaker N, Clark L, White NC, Marsolek M. Emerging battery-ingestion hazard: clinical implications. Pediatrics. 2010 Jun;125(6):1168-77.
- Lerner DG, Brumbaugh D, Lightdale JR, Jatana KR, Jacobs IN, Mamula P. Mitigating Risks of Swallowed Button Batteries: New Strategies Before and After Removal. J Pediatr Gastroenterol Nutr. 2020 May;70(5):542-546
- Chiew AL, Lin CS, Nguyen DT, Sinclair FAW, Chan BS, Solinas A. Home Therapies to Neutralize Button Battery Injury in a Porcine Esophageal Model. Ann Emerg Med. 2023 Sep
- Chao S, Gibbs H, Rhoades K, Mehrer C, Jacobs IN, Jatana KR. Button battery taping and disposal: Risk reduction strategies for the household setting. Int J Pediatr Otorhinolaryngol. 2022 Feb
- Leinwand K, Brumbaugh DE, Kramer RE. Button Battery Ingestion in Children: A Paradigm for Management of Severe Pediatric Foreign Body Ingestions. Gastrointest Endosc Clin N Am. 2016 Jan;26(1):99-118.

Toxicology Library
DRUGS and TOXICANTS
Dr Neil Long BMBS FACEM FRCEM FRCPC. Emergency Physician at Kelowna hospital, British Columbia. Loves the misery of alpine climbing and working in austere environments (namely tertiary trauma centres). Supporter of FOAMed, lifelong education and trying to find that elusive peak performance.

Great review! Thanks Neil!