Lester T. Jones

Lester Tallmon Jones (1894-1983) was an American ophthalmologist
Jones specialised in dacryology. He postulated that tear drainage is not passive plumbing but a blink-driven functional system. He described the lacrimal pump, lacrimal diaphragm, and formalised the Jones fluorescein dye tests (I & II) for epiphora. He created a bypass solution for canalicular failure, the conjunctivodacryocystorhinostomy (CDCR), and the Jones (Pyrex) tube to manage patients without a functional canalicular system.
He is remembered by the establishment of a national surgical anatomy award in his name, a major surgical text on lids and lacrimal surgery, and institutional honours including the Watzek Award.
Biographical Timeline
- Born June 13, 1894, Danville, Boyle County, Kentucky
- 1906 – Family moved to Forest Grove, Oregon
- 1921 – Graduated University of Oregon Medical School
- 1921 – Internship at the Polyclinic, Philadelphia.
- Early 1920s – Worked as a ship’s doctor on a freighter to South America. Returned to Portland and began general practice.
- 1922–1941 – Taught anatomy at the North Pacific Dental College
- 1927–1928 – Undertook specialist training Staatliches Universität, Vienna in EENT (eye, ear, nose & throat)
- World War II – Served in the U.S. Navy, reaching captain;. Executive officer of the Bremerton Naval Hospital by war’s end.
- Post-WWII – Returned to Portland; practiced ophthalmology/ENT (later limited practice to ophthalmology).
- Academic career (post-WWII onward) – Volunteer faculty at what is now Oregon Health & Science University (OHSU); became Professor of Anatomy, later Emeritus Professor
- 1972 – ASOPRS instituted the ‘Lester T Jones’ Award (now the Lester T. Jones Surgical Anatomy Award) recognising outstanding contributions to ophthalmic plastic/reconstructive surgery.
- 1976 – Published the 241-page treatise Surgery of the Eyelids and Lacrimal System
- 1977 – Retired from active clinical practice at age 82.
- 1980 – Received the Aubrey R. Watzek Award
- Died October 30, 1983 (aged 89), Portland, Multnomah County, Oregon, USA
Key Medical Contributions
Lacrimal pump (concept and anatomical mechanism)
Jones defined lacrimal drainage as a dynamic, blink-driven system, not simply passive “plumbing.”
1958 – Jones separated the lacrimal apparatus into three functional components: a secretory (tear production), a distributional (the eyelids spreading tears), and excretory (drainage). He coined the term “lacrimal pump” to describe how blinking actively drives tears through the canaliculi into the lacrimal sac and onward to the nose.
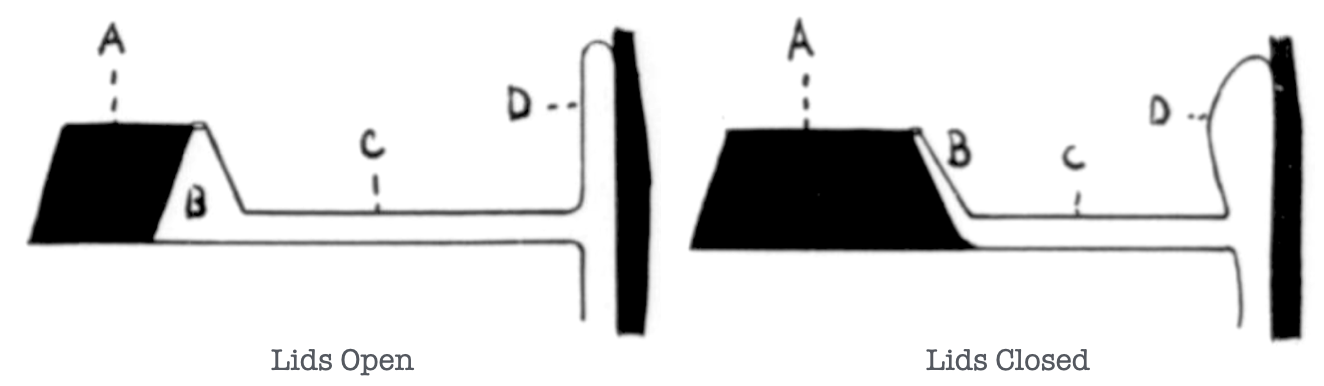
A. tarsus; B. ampulla; C. canaliculus; D. fundus of tear sac.
Jones, 1958
1961 – Jones described a “lacrimal diaphragm” at the medial canthus whose movement during blinking creates alternating pressures within the lacrimal sac. Negative pressure to draw tears in, followed by positive pressure to propel tears onward. An important concept for lacrimal surgery to respect the canaliculi and preserve the pumping structures, as drainage success depends on function as much as patency.
Jones fluorescein dye tests (Jones I & II)
Building on his “lacrimal pump” physiology, Jones used fluorescein to create a simple diagnostic pathway for epiphora. The core idea is to differentiate functional delay from anatomic obstruction, and to localise the site of blockage by following fluorescein’s transit from the ocular surface to the nose.
In his teaching, a “primary” fluorescein test became a practical clinic procedure: instil fluorescein, avoid wiping the tears away, then look for dye reaching the inferior meatus, potentially revealing obstruction at the anterior end of the inferior turbinate.
1972 – Jones, Marquis & Vincent quantified the “primary dye (fluorescein) conduction test“. By instilling 2% fluorescein and repeatedly sampling the inferior meatus to measure dye transit time, he showed that superior and inferior canaliculi contribute similarly to drainage.
1977 – Jones publishes his “lacrimal fluorescein test” a painless method for diagnosing lacrimal obstruction in routine practice. Place a fluorescein drop in each eye, no wiping, topical nasal anaesthesia, then gentle sampling of the inferior meatus with a cotton-tipped applicator to detect dye.
Conjunctivodacryocystorhinostomy (CDCR) and the Jones tube (Pyrex glass tube)
Jones designed the conjunctivodacryocystorhinostomy (CDCR) as a bypass procedure for patients with significant epiphora due to permanent canalicular failure (e.g., congenital absence, traumatic destruction, cicatricial closure). His solution was to create a new passage from the conjunctival tear lake toward the nasal cavity and maintain it long enough to become stable, then keep it patent with a tube designed for long-term tolerance.
In every case of disturbing epiphora due to a permanent failure of the canaliculi, a new passage should be created…A glass tube possessing capillary attraction combined with the negative pressure phase of tidal respiration in the nose, is a satisfactory substitute for the lacrimal pump.
Jones, 1965
1965 – Jones formalised CDCR with a Pyrex glass tube (“Jones tube”), arguing that a properly sized glass conduit could act as a practical substitute. He outlined the tube’s mechanism as capillary attraction combined with the negative-pressure phase of nasal respiration.
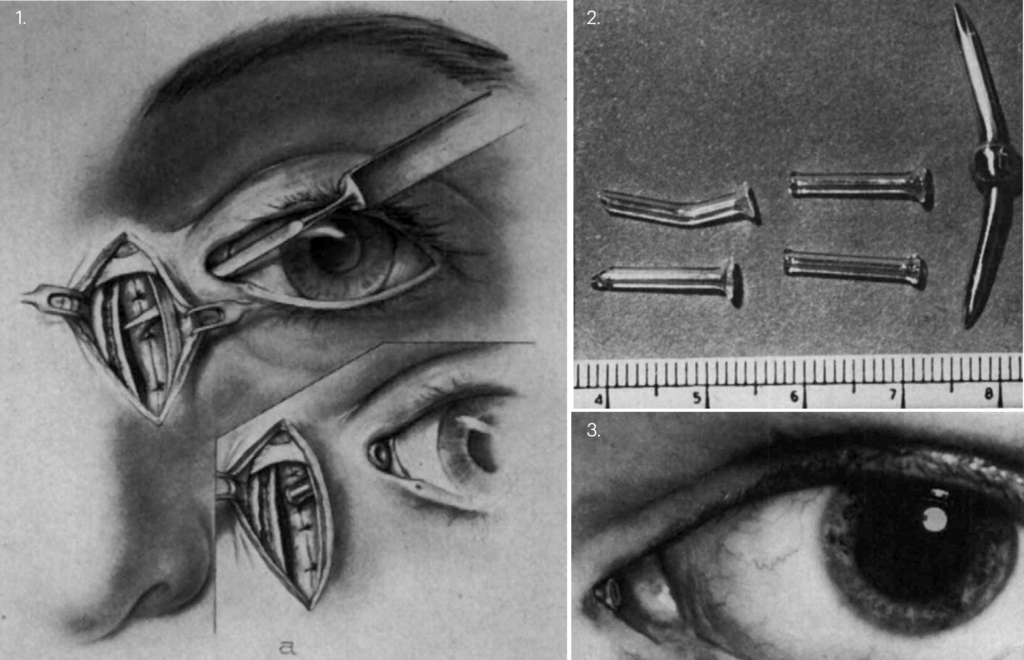
2. Pyrex glass tubes with bevelled ends and 2.5-mm enlarged ends and double-ended dilator
3. Appearance of tube in normal position. Jones, 1965
Major Publications
- Jones LT, Boyden GL. A new mucous membrane flap for dacryocystorhinostomy. Trans Pac Coast Otoophthalmol Soc Annu Meet. 1952;33:137-41; discussion, 141-5.
- Jones LT, Boyden GL. New mucous membrane flap for dacryocystorhinostomy. AMA Arch Otolaryngol. 1952 Oct;56(4):405-8.
- Jones LT. Epiphora: its causes and new surgical procedures for its cure; a preliminary report. Am J Ophthalmol. 1954 Dec;38(6):824-31.
- Jones LT. The lacrimal apparatus: practical fundamentals of anatomy and physiology. Trans Am Acad Ophthalmol Otolaryngol. 1958 Sep-Oct;62(5):669-78. [Lacrimal pump]
- Jones LT. An anatomical approach to problems of the eyelids and lacrimal apparatus. Arch Ophthalmol. 1961 Jul;66:111-24. [Lacrimal pump]
- Jones LT. Tear-sac foreign bodies. Am J Ophthalmol. 1965;60(1):111–113.
- Jones LT. New punctum and canaliculus dilator. Trans Am Acad Ophthalmol Otolaryngol. 1967 Mar-Apr;71(2):360.
- Jones LT. Conjunctivodacryocystorhinostomy. Am J Ophthalmol. 1965;59(5):773–783.
- Jones LT. Conjunctivodacryocystorhinostomy. J All India Ophthalmol Soc. 1967 Jun;15(3):86-93.
- Jones LT, Marquis MM, Vincent NJ. Lacrimal function. Am J Ophthalmol. 1972 May;73(5):658-9.
- Jones LT. Anatomy of the tear system. Int Ophthalmol Clin. 1973;13(1):3–22
- Jones LT. Trials and tribulations of an ophthalmic anatomist. Trans Pac Coast Otoophthalmol Soc Annu Meet. 1975;56:11-6.
- Jones LT. Lacrimal fluorescein test. Am J Ophthalmol. 1977 May;83(5):762.
- Jones LT, Wobig JL. The Wendell L. Hughes Lecture. Newer concepts of tear duct and eyelid anatomy and treatment. Trans Sect Ophthalmol Am Acad Ophthalmol Otolaryngol. 1977 Jul-Aug;83(4 Pt 1):603-16.
References
Biography
- Obituary. Dr Lester T. Jones. The Oregonian, 1 Nov 1983: 91
- Wobig JL. Lester T. Jones, MD: An Early Expert on Orbits Both Human and Animal. AAO, Feb 21, 2018
- Dailey RA, Wobig JL, Ali MJ. Lacrimal History – Part 37: Doyens of Dacryology Series – Lester Tallmon Jones (1895-1983). Semin Ophthalmol. 2025 Aug;40(6):451-454
Eponym
the person behind the name
BVisSci, MD, University of Notre Dame, Fremantle. Doctor, baker, avid traveller, aspiring ophthalmologist
BA MA (Oxon) MBChB (Edin) FACEM FFSEM. Emergency physician, Sir Charles Gairdner Hospital. Passion for rugby; medical history; medical education; and asynchronous learning #FOAMed evangelist. Co-founder and CTO of Life in the Fast lane | On Call: Principles and Protocol 4e| Eponyms | Books |

