Night shift and paying it forward
On a cold Monday night in late winter I pulled on my scrubs, packed my lunch and quietly crept into the small, cosy room my children share. My daughter was lying rumpled and skewiff in her big bed, covers thrown back, her little nappy clad bottom in the air. I moved to the cot where my son was safe and snuggly in his baby sleeping bag, little hands balled into tight fists by his face, fair head turned to one side, breath soft and rhythmic. Then I kissed my husband, patted our dogs and went to work, staying up all night to treat other people’s families while mine slept. I was back on the grindstone of the ED registrar roster, where nightshift is as inevitable as breathing.
Six months earlier, late in the afternoon of his due date, my son Tom entered the world and took his first breath. But when the warm slippery bundle was placed upon my chest he simply lay, still and blue, his initial mew of surprise followed by silence. The paediatrician went to work, suctioning his trachea before gently inflating his lungs with tiny, quick bursts of the toy-like neopuff. Oxygenated blood now circulating again, Tom gave a few tentative cries then settled into steady, if slightly fast respirations. The crisis had passed and we all relaxed a little. Except my husband, the only non health professional in the room, who still had the sick feeling of something being very bad. His human intuition turned out to be more accurate than the accumulated knowledge and experience of the rest of us.
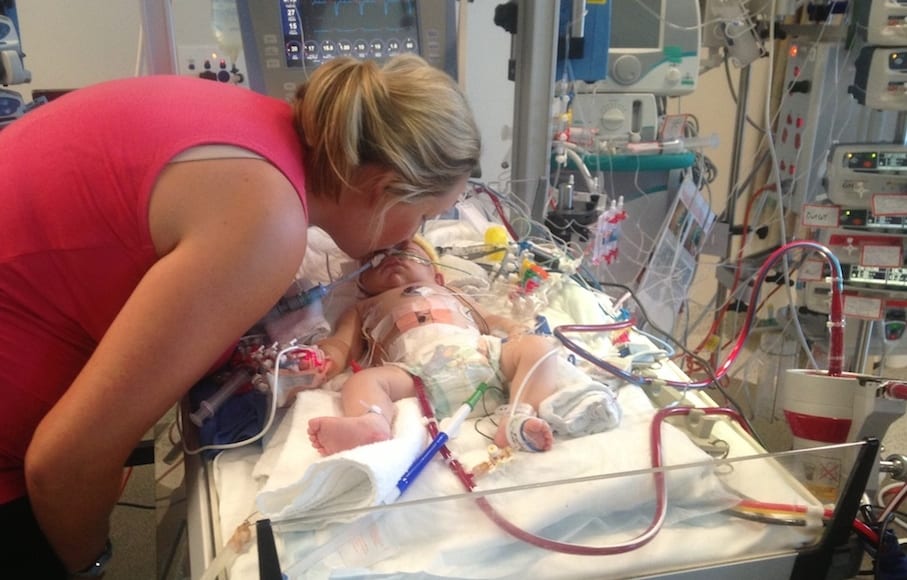
The next time I saw him, my now two hour old son was lying prone, grunting, tachypnoeic, the muscles retracting deep between his ribs as he desperately tried to move air into his little lungs. Thick, toxic meconium sludge was clogging his air passages, delicate alveoli tissue becoming progressively more inflamed and waterlogged. A weakened patch of his right lung had overexpanded and perforated, the growing pneumothorax further compromising his efforts to breathe. The special care nurses were quiet and serious. Perhaps still unsure of the situation and my role within it, I asked to see his gas. It was not reassuring. My boy was sick.
Events progressed. A solemn talk with the paediatrician. The wait while he was intubated and “plumbed” for transfer. A midnight departure for Elsewhere. I was not well enough to accompany him but by mutual agreement my husband left my side to be with our new son. To advocate for him, to hold his little hand so he never felt alone, and, we both felt but didn’t articulate, to ferociously fight off death if it circled. That the separation felt so unnatural as to be outside the laws of physics didn’t concern me; If Tom were to survive he needed more than cuddles and his mother’s breast.
Born elsewhere in place or history, Tom would have died in his first twenty-four hours. And if our son had died that night he would be simply one of the almost two million babies who die on the day they are born each year. Our personal story, however, would have changed profoundly, sadness and loss seeping through to wash a little colour out of our days. Despite our beautiful daughter to hold close, and the possibility of more children to come, we would have joined the ranks of the brave parents who live with empty arms.
But Tom survived. After five days on ECMO, another seven ventilated and a total of three weeks in hospital, we strapped our tiny bundle into his capsule and, driving slowly and carefully, took him home.
There are many reasons why Tom didn’t die during that first night. The paediatrician on call recognised his early deterioration and organised a timely transfer. The retrieval system worked, and Tom was taken to the right hospital at the right time. The retrieval staff maintained his standard of care en route, and his receiving hospital was a paediatric centre of excellence with a strong ECMO culture.
But Tom also survived because caring and experienced clinicians left their homes and families at bedtime and went to work. There, they made difficult judgement calls and performed challenging procedures at hours during which they had every right to be sleeping undisturbed.
And that is why I don’t mind working night shift anymore. Because it would be an honour to be the alert and skilled doctor whose actions overnight changed the course of someone else’s personal story. Because I have a hell of a lot of paying it forward to do. And because at the end of my shift, I go home and I see my Tom.

SMILE
squared
Emergency physician and keen follower of #FOAMed | @KristinJBoyle | LinkedIn