Open wide
Ever wondered what the ultrasound peeps do in the ‘sonocave’?
…tonsillar ultrasound of course!
Rationale
Clinically differentiating peritonsillar abscess (quinsy) from uncomplicated tonsillitis can be difficult. Traditional teaching dictates the uvula should be displaced away from the side of a quinsy, and that a quinsy tends to obliterate the palatoglossal fold.
In reality we find clinical assessment is relatively unreliable…
Tonsillar Ultrasound Technique
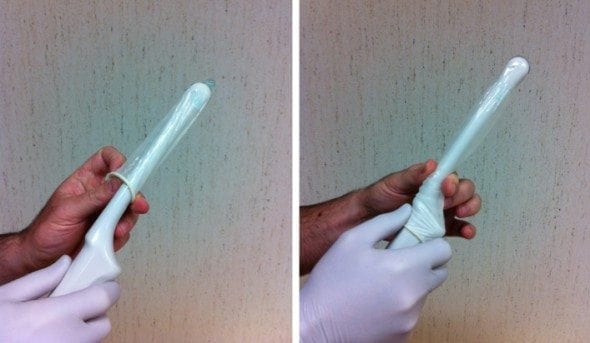
- Chose either a sterilised endocavity transducer or a hockey stick transducer for this procedure.
- Cover it with an unused condom.
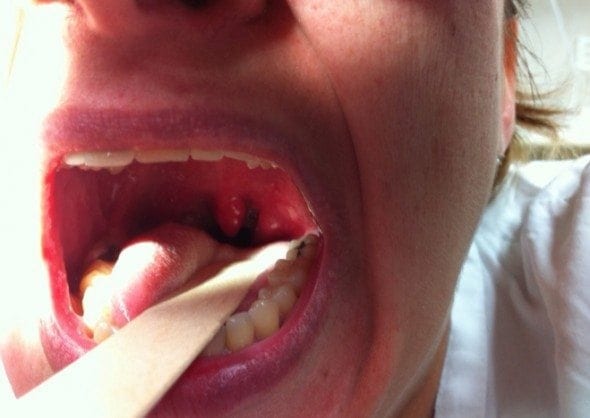
- Explain the procedure to the patient, reassuring them it is not as bad as it looks!
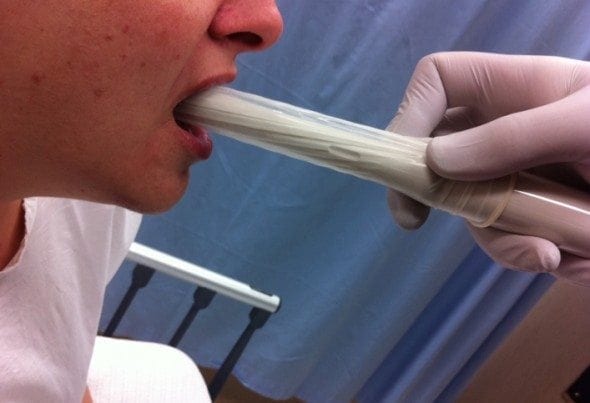
- Spray the oropharynx with a local anaesthetic ENT spray. Now introduce the transducer carefully with the imaging plane transversely oriented.
- Gently push the transducer against the enlarged tonsil watching for any flow within the area of interest. Add colour Doppler. Record images measuring the size of any collection in both the transverse and longitudinal planes.
- Noting the depth from mucosal surface to collection, and from mucosal surface to carotid gives the proceduralist a sense of relative depths.
Clinical Cases
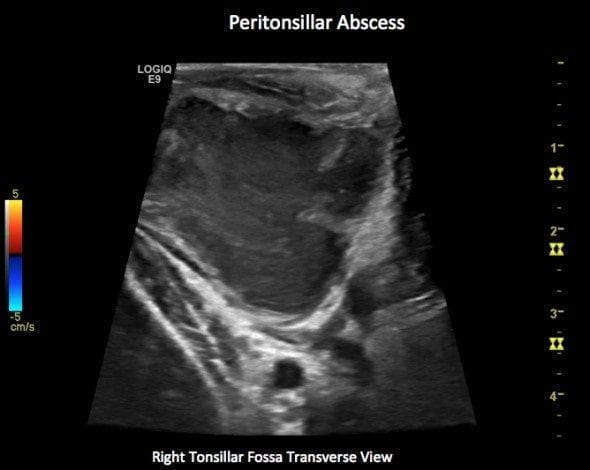
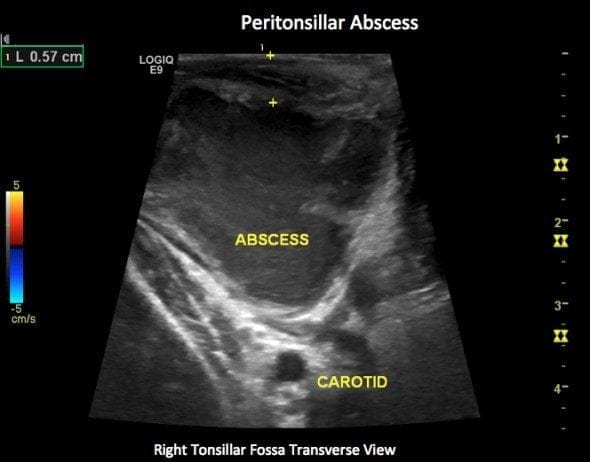
Peritonsillar Abscess – Right Tonsillar fossa
Differentiation between solid enlarged tonsil and peritonsillar abscess is made by close observation of the heterogenous predominantly hypoechoic material within the tonsillar area.
- If an abscess has formed subtle movement of the probe will cause the pus to flow within the collection.
- If the tonsillar enlargement remains solid, no such flow occurs.
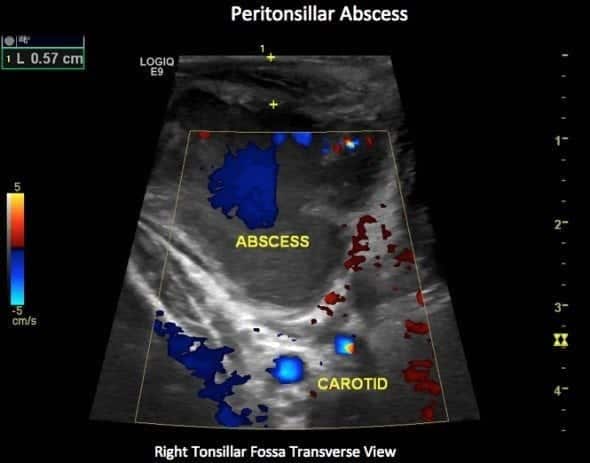
The addition of colour Doppler also assists. There is no flow within an abscess, whereas an inflamed enlarged but solid tonsil tends to be hyperaemic. In the first case note the vascular flow within the solid tonsil.
In the second case the flash of blue within the image is artefact, not hyperaemia

ULTRASOUND LIBRARY
POCUS
An Emergency physician based in Perth, Western Australia. Professionally my passion lies in integrating advanced diagnostic and procedural ultrasound into clinical assessment and management of the undifferentiated patient. Sharing hard fought knowledge with innovative educational techniques to ensure knowledge translation and dissemination is my goal. Family, wild coastlines, native forests, and tinkering in the shed fills the rest of my contented time. | SonoCPD | Ultrasound library | Top 100 | @thesonocave |