Patellar dislocation
Clinical case presentation
A 32 male presents to the ED following a hefty collision with another player during a football game. During the altercation he sustained a direct blow to the medial aspect of his left knee.
On examination the patient is lying on a trolley in considerable pain, you look at the left kneecap and noticed it’s displaced laterally. The nurse starts administering Nitrous Oxide to the patient which helps the pain considerably.
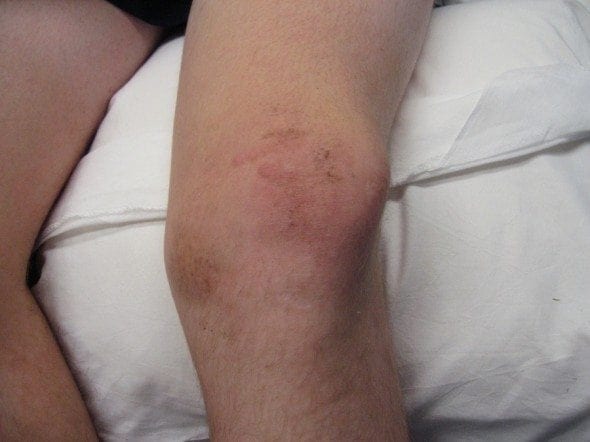
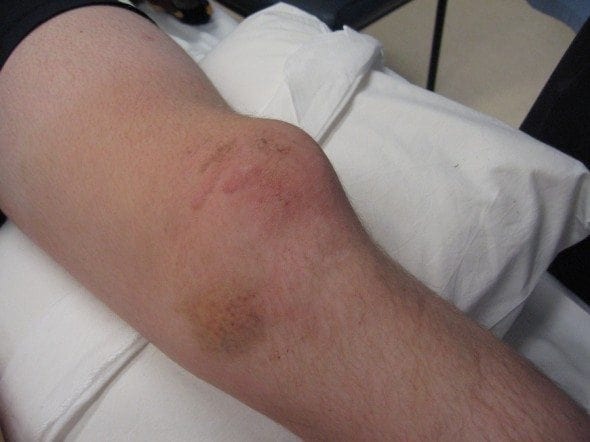
Patella Dislocations
- Majority of patella dislocations occur in females, especially targeting teenage girls.
- Literature shows, depending on the study that 30-72% of patellar dislocations are sports related and 28-39% will involve osteochrondral fractures
- The most common location of patella dislocations is lateral dislocation.
- Patients complain of the knee suddenly giving way, and inability to weight-bear or extend the knee and are often in considerable pain.

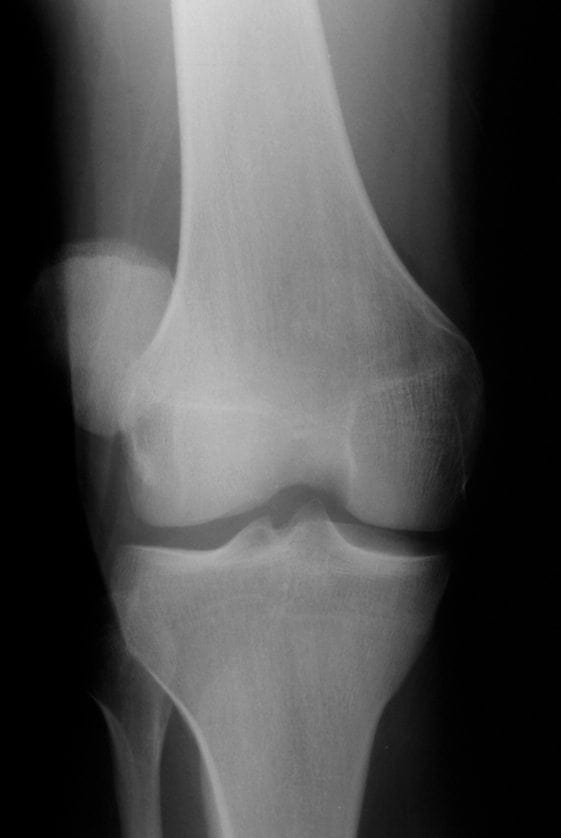
Anatomy
- The Patellar is the largest sesamoid bone in the body, and it resides within the complex of the quadriceps and patellar tendons.
- It functions as both a lever and a pulley.
- As a lever, the patella magnifies the force exerted by the quadriceps or knee extension.
- As a pulley, the patella redirects the quadriceps force as it undergoes normal lateral tracking during flexion.

Mechanism of Injury:
- Generally there is two types of mechanisms that result in patella dislocations.
- Type 1: results when there is a powerful contraction of the quadriceps in combination with sudden flexion and external rotation of the tibia on the femur. This is the most common reason for the patellar to dislocate.
- Type 2: results from direct trauma to the patella with the knee in flexion, can cause dislocation, however this is seen uncommonly.
Patellar Dislocations are common in patients with the following:
- Genu valgum
- Genu recurvatum
- Excessive femoral neck anteversion or internal femoral torsion
- External tibial torsion
- Lateral insertion of patella ligament on the tibia
- Contracture of the lateral patellar retinaculum
- Relaxation of attenuation of medial patellar retinaculum
- Hypoplasia or dysplasia of the patellar
- Hypoplasia or flattening of the trochlear grove
- Patellar alta or high riding patellar
- Atrophy of the vastus medialis muscle
- Pes planus
- Generalised joint laxity
Assessment of Patellar Dislocation:
- Assess neurovascular status distal to the patellar
- The apprehension test can be used to assess for patellar dislocation and subluxation. Apprehension sign occurs when the knee is placed at 30° flexion, and lateral pressure is applied. Medial instability results in apprehension by the patient.
- Examine for anterior defect, the laterally deviated patellar, and swelling and medial joint line tenderness of the partially flexed knee.
- Order X-rays of the knee AP and lateral generally provide adequate views.
- If the patellar is already relocated, still order X-rays to rule out fracture
Management of Patellar Dislocation
- Provide analgesia, Nitrous Oxide with oxygen is generally effective and can also be used during reduction of the dislocation
- Reduction is achieved by pushing the patellar medially with firm pressure, whilst extending the knee.
- First time dislocations should be splinted in above knee plaster cast and referred to the next available fracture/orthopaedic clinic
- Patients presenting with recurrent dislocations post reduction, can be splinted in a pressure bandage or Richards splint, until follow up can be arranged.
- Patients should be discharge home on crutches with simple analgesia for pain control.
- Generally conservative management is all that is required for patellar dislocations, surgical intervention is considered when recurrent dislocations occur, and those with anatomical abnormality.
Reference
- Fiebel, R. Dehghan, N. Cwinn, A. (2007). Irreducable lateral pattelar dislocation: The importance of impaction fracture recognition. The Journal of Emergency Medicine. 33(1), 11-15. [Reference]
- Patellar Dislocations. (2007). In Buttaravoli, P (Ed), Minor Injuries Splinter to Fractures (p.509-512). Philadelphia: Mosby Elsevier.
- Lu, D. Wang, E. Self, W. & Kharasch, M. (2010). Patellar Dislocation Reduction. Academic Emergency Medicine. 226.
- Malanga, G. White, B. Lee, W. & Angeson, T. (2009). Patellar Injury and Dislocation. Accessed 30/04/2010 @ http://emedicine.medscape.com/article/90068-overview
- Simon, R. Sherman, S. Koenigsknecht, S. (2007). Patellar Dislocations: Emergency Orthopaedics The Extremities. pp.430-432. New York: McGraw Hill
[cite]
Emergency nurse with ultra-keen interest in the realms of toxicology, sepsis, eLearning and the management of critical care in the Emergency Department | LinkedIn |
