Broken open
aka Bone and Joint Bamboozler 001
A 34 year-old woman is brought to your emergency department following an accident at a local tourist attraction. She was careering downhill in a ‘luge’ (a type of small 4-wheeled go-kart with handle bars for steering, foot brakes and, thankfully, no engine).
To avert a collision with another ‘luger’ she tried to come to a sudden stop. Unfortunately, instead of using the foot brakes she reflexively put her right foot out of the ‘luge’ onto the fast-moving ground — she heard a loud ‘crack’ and experienced immediate pain in her right ankle as she crashed.
An ambulance was called and the paramedics splinted her right lower limb and gave her IV morphine for pain. On arrival, she is GCS 15 and her vital signs are within normal limits.
Following the removal of her footwear you examine the right ankle and see this:
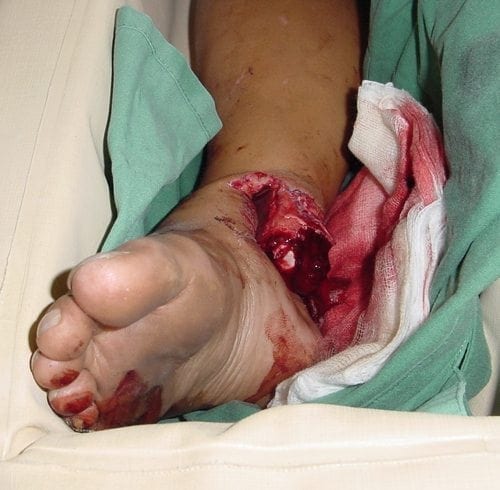
Describe the injury?
Bamboozler Answer
The photograph shows an open fracture of the distal tibia; the ankle is almost certainly dislocated.
The medial malleolus is exposed and is protruding through a large complex laceration.
There appears to be significant tissue loss overlying the bone.
The wound is not overtly contaminated.
Although difficult to be certain from the photograph, the foot may be somewhat pale and dusky, which suggests circulatory compromise.
What is an open fracture?
Bamboozler Answer
An open fracture is a fracture that communicates with an overlying disruption of the skin and soft tissues.
They are called compound by the obscure and pseudo-erudite.
What are the key aspects of history and examination?
Bamboozler Answer
Remember to start with the primary survey — the ABCs.
History:
- take the usual AMPLE history but focus on:
- impact energy, e.g. fall from a great height versus tripped over the curb.
- likelihood of contamination, e.g. tractor roll-over on a farm = very dirty!
Examination:
- examine the wound, the surrounding tissues, and look for contamination.
- assess neurovascular status.
- perform a secondary survey identify any other associated injuries (is the patient’s head still attached?)
How can you tell if a fracture is open?
Bamboozler Answer
Most open fractures are obvious, but this is not always the case.
In general, exploration of wounds that overly fractures should not be performed in the emergency department as it is usually not very informative and disruption may increase the risk of infection.
However, a blunt sterile probe may be safely used to determine if bone can be contacted and is in communication with the wound.
Visible tracking of air from the wound to the fracture on x-ray is also highly suggestive.
If in doubt, leave it for an orthopedic surgeon to explore in the operating theatre.
What is the Gustillo-Anderson classification of open fractures?
Bamboozler Answer
The Gustillo-Anderson classification describes open fractures and their risk of infection according to degree of soft tissue injury and contamination. (The infection risks quoted above are ball-park figures only.):
Class I <1 cm wound — no evidence of contamination (0-2% infection risk)
Class II >1 cm wound — moderate contamination (2-5%)
Class IIIA severe soft tissue injury but adequate bone coverage, highly contaminated (5-10%)
Class IIIB severe soft tissue injury, massive contamination, bone is exposed and there is periosteal stripping (10-50%)
Class IIIC same as IIIB but with an arterial injury requiring repair (25-50%). Class IIIC injuries, understandably, have a high rate of amputation.
The injury in this case is either Class IIIB or IIIC, depending on whether there is an arterial injury.
The Gustillo-Anderson classification certainly is not the be-all and end-all for determining outcomes – for instance, the Mangled Extremity Severity Score (MESS) takes into account other factors:
- extent of skeletal and soft-tissue damage
- extent and severity of limb ischemia
- associated shock
- age
How would you manage an open fracture in the ED?
Bamboozler Answer
Give the orthopods a shout early, in case they are free to come down and look at the wound right away (it might happen you know!), and let the radiographers know that their skills are needed.
Management overview:
- Attend to ABCs including C-spine precautions if necessary
- Control hemorrhage and correct coagulopathy e.g. direct pressure, tourniquets if in extremis. Fluid resuscitation, transfusion of packed cells and other blood products as required
- Analgesia and antibiotics earlye.g. morphine or fentanyl +/- ketamine for analgesia. See Q10 for antibiotics
- Assess the limb and seek/treat complicationse.g. neurovascular compromise, compartment syndrome, crush injury and rhabomyolysis
Following the provision of adequate analgesia:
- Remove gross contaminants from the wound
- If there will be more than a 1 to 2 hour delay in going to the operating theatre for washout and debridement then clean by profusely irrigating with saline and cover the wound with a sterile dressing (e.g. saline soaked pads).
- Reduce gross deformities using gentle traction and splint the injured limb — this is a top priority if there is neurovascular compromise
- Immobilise the limb with a POP backslab and elevate the limb
- Tetanus toxoid/ tetanus immunoglobulin if indicated
Remember to look at the x-ray and consult orthopedics. Consider taking a photograph of the wound so that different doctors don’t keep coming along and pulling down the dressings, which will add to the risk of infection.
Don’t forget the secondary survey or you might miss other injuries!
The short version of the immediate management of any fracture is this (the order may vary, and not every step is required in every instance):
CCCAAARE
- Control hemorrhage and correct coagulopathy
- Seek and treat Complications
- Clean and cover any open wounds
- AAA therapy (analgesia, antibiotics, ADT/ tetanus)
- Reduce and immobilise
- Elevate
What is the ‘Six Hour Golden Rule’ of Orthopedics?
Bamboozler Answer
The ‘Six hour Golden Rule‘ holds that open fractures require operative repair within 6 hours of injury to decrease the risk of osteomyelitis.
The evidence base for this is limited, and times are a changin’.
In general, cases are more likely to be done ‘urgently’ the next day rather than rushed to theatre.
However, open fractures associated with gross contamination or a mangled limb are best taken to theatre ASAP.
The 6 hour golden rule grew out of lab studies of bacterial doubling time and early clinical outcome studies. Since then a lot has changed, including improved emergency care, and later studies suggest operative care can be safely delayed up to 24 hours in many cases.
Should you swab the wound for culture in the ED?
Bamboozler Answer
This is often requested of emergency department staff, and is often performed — primarily to keep inter-departmental relations well lubricated.
In truth, there is little evidence that pre-debridement cultures alter the management of open fractures.
They do not necessarily indicate that infection has occurred, nor whether the cultured organisms are the actual culprit.
Which is better, covering open fractures with pads soaked in saline or iodine?
Bamboozler Answer
Saline
Povidone-iodine causes tissue destruction. Its old school. Don’t use it.
What antibiotics should you use for open fractures?
Bamboozler Answer
Staphylococcus aureus is the most common cause of secondary infection, and the Australian Therapeutic Guidelines recommendation for first-line prophylaxis for open fractures is:
flucloxacillin 2 g (child: 50 mg/kg up to 2 g) IV, 6-hourly.
However, most sources suggest broad spectrum antibiotics that cover both gram-positives and gram-negatives, depending on the severity of the injury and degree of contamination. Choice will depend on local sensitivities and personal proclivities — and every book you look up will tell you something different!
Grade I/ II
- 1st generation cephalosporin
- e.g. cephazolin 1 g (child: 25 mg/kg up to 1 g) IV, 8-hourly
- e.g. cephalothin 2 g (child: 50 mg/kg up to 2 g) IV, 6-hourly
Grade II/ III
- add an aminoglycoside (e.g. gentamicin)
If heavily contaminated
Add penicillin or metronidazole due to the risk of infection with Clostridum and other anaerobes.
Consider adding doxycycline, or changing to ciprofloxacin, if the wound is heavily contaminated with sea water to cover for Vibrio species.
When should antibiotic prophylaxis be started?
Bamboozler Answer
As soon as possible (I suggest waiting until after the injury has occurred…)
The rate of infection is thought to increase with delays of greater than 3 hours post-injury.
References
- Newton EJ, Love J. Acute complications of extremity trauma. Emerg Med Clin North Am. 2007 Aug;25(3):751-61, iv. [PMID: 17826216]
- Lee CK, Hansen SL. Management of acute wounds. Surg Clin North Am. 2009 Jun;89(3):659-76. [PMID: 19465203]
- Auerbach PS. Auerbach Wilderness Medicine
- Sherman, S. Simon’s Emergency Orthopedics 7e
- Purcell, D. Minor Injuries A Clinical Guide 3e

CLINICAL CASES
Bone and Joint Bamboozler
Chris is an Intensivist and ECMO specialist at The Alfred ICU, where he is Deputy Director (Education). He is a Clinical Adjunct Associate Professor at Monash University, the Lead for the Clinician Educator Incubator programme, and a CICM First Part Examiner.
He is an internationally recognised Clinician Educator with a passion for helping clinicians learn and for improving the clinical performance of individuals and collectives. He was one of the founders of the FOAM movement (Free Open-Access Medical education) has been recognised for his contributions to education with awards from ANZICS, ANZAHPE, and ACEM.
His one great achievement is being the father of three amazing children.
On Bluesky, he is @precordialthump.bsky.social and on the site that Elon has screwed up, he is @precordialthump.
| INTENSIVE | RAGE | Resuscitology | SMACC
