COVID-19 airway management: better care through simulation
Editor’s note: Health services around the world are faced with the challenge of preparing for the impact of COVID-19 on their communities as we all prepare for a potential global pandemic. I, like many others, see a great role for simulation in process development and testing and see COVID-19 as a prime example of how simulation can make a difference by improving systems and processes of patient care. My team in Melbourne is working on this and are very keen to learn from the experiences of others. Fortunately, Dr Albert Chan (@gaseousXchange) and his colleagues in Hong Kong have extensive experience (>40 COVID-19 simulations at the time of writing) and are willing to share it with the world. Read on for their insights into how to deliver COVID-19 airway management simulations, including principles for instructional design and practical tips on how to make it happen effectively.
– A/ Prof Chris Nickson (@precordialthump)
Background
- COVID-19 epidemic is threatening global health, and declared by WHO as a Global Health Emergency
- Healthcare workers are in the forefront battling the virus, particularly during aerosol generating procedures such as intubation (Caputo, Byrick, Chapman, Orser, & Orser, 2006)
- Statistics from Wuhan showed that 1,716, approximately 3.8% of confirmed cases in a series were infected (Wu & McGoogan, 2020)
- Some communities are in the heat of battling the disease, while others have some lead time for preparedness for Covid-19 amongst healthcare staff
- Simulation-based medical education (SBME) certainly has its role, and has been utilized in previous epidemics (Phrampus et al., 2016)
- In-situ simulation was carried out in intensive care unit and operating theaters at the Department of Anaesthesia and Intensive Care, Prince of Wales Hospital (affiliated with Chinese University of Hong Kong) in preparedness for the outbreak
Simulation goals
- Build staff preparedness for managing suspected or confirmed cases of Covid-19 with “just-in-time training” (Van Merriënboer & Kirschner, 2017) in a timely manner (short lead time for preparation)
- Engage in process testing based on systems integration principles and refine infection control protocols and workflows (Dubé et al., 2019; Reid, Stone, Huang, & S. Deutsch, 2016)
Simulation location
- Best if carried out in situ – in the actual clinical work place e.g. in Airborne Infection isolation Room (AIIR)
- Interprofessional, authentic teams training in their respective settings
- Need institutional support, and engage staff of all levels to optimize preparedness
- In-situ simulation also serves as a platform for systems and process testing, and detection of latent safety threats, specifically with infection control issues (Patterson, Geis, Falcone, LeMaster, & Wears, 2013; Reid et al., 2016)
Simulation Modality and Instructional Design
For building capacity
- To build staff prepares in a timely manner for epidemic preparedness, consider applying principles of “Rapid Cycle Deliberate Practice” (Hunt et al., 2014) to focus on rapid acquisition of skills (e.g. airway management for Covid-19 cases) through mastery learning
- Direct feedback, according to a standardized rubric, and allowing for opportunities to repeat the process may be the focus, as supposed to focused facilitation (Eppich & Cheng, 2015; Hunt et al., 2014)
- Using visualization of contamination is a powerful learning aid for infection control (Pope, Baggett, Dubois, Martin, & Gore, 2014). Consider using stickers, GlitterBugTM, or video review for debriefing.
- Some centers may have lots of staff to train – in that case do think of observer roles with specific tasks, which has also been shown to improve learning outcomes (O’Regan, Molloy, Watterson, & Nestel, 2016)
For process testing
- Participants should be oriented in the beginning of simulation regarding purpose of simulation, including process testing, and be given the opportunity of expressing their concerns about the processes of infection control within the in-situ setting (Dubé et al., 2019)
- The feedback from the simulations should be used as a basis to refine system processes
Facilitators
- Preferably, the facilitators are trained simulation facilitators and debriefers with knowledge in systems testing and integration
- If not, providing scripts, or utilizing available resources, to guide faciliators may be useful
- It is a great opportunity for faculty development as well, if your institution has the capacity for it, given the great number of simulations that may need to be run
Practical issues and tips
- Psychological safety is very important, especially in this setting, as participants may be very anxious and overwhelmed by infection risks, as well as the protocols and guidelines. Make efforts to orient learners and establish a safe container (Rudolph, Raemer, & Simon, 2014).
- Do develop a script for prebriefing (sample is provided in links) to orientate learners, establish safe container and decrease cognitive load of facilitators
- Using AIIR enhances fidelity and authenticity, and allows systems testing. However, AIIR may need to be used for clinical purposes, balance between training needs and clinical service must be kept, and plan for contingencies.
- Consumption of PPE is a genuine concern in current epidemic, yet practicing gown up and gown down are essential for staff safety (Lau et al., 2004). Do make efforts to conserve PPE for simulation training.
- Institutional support and stakeholder engagement are vital to success of program, because of the resource and time put into building staff capacity in a short time. Feedback your findings from systems testing to further enhance workflow and processes
- Develop learning objectives based on your institutional Needs
Resources (free to download for non-profit educational use)
Resources for delivering a COVID-19 airway management simulation in the operating theatre:
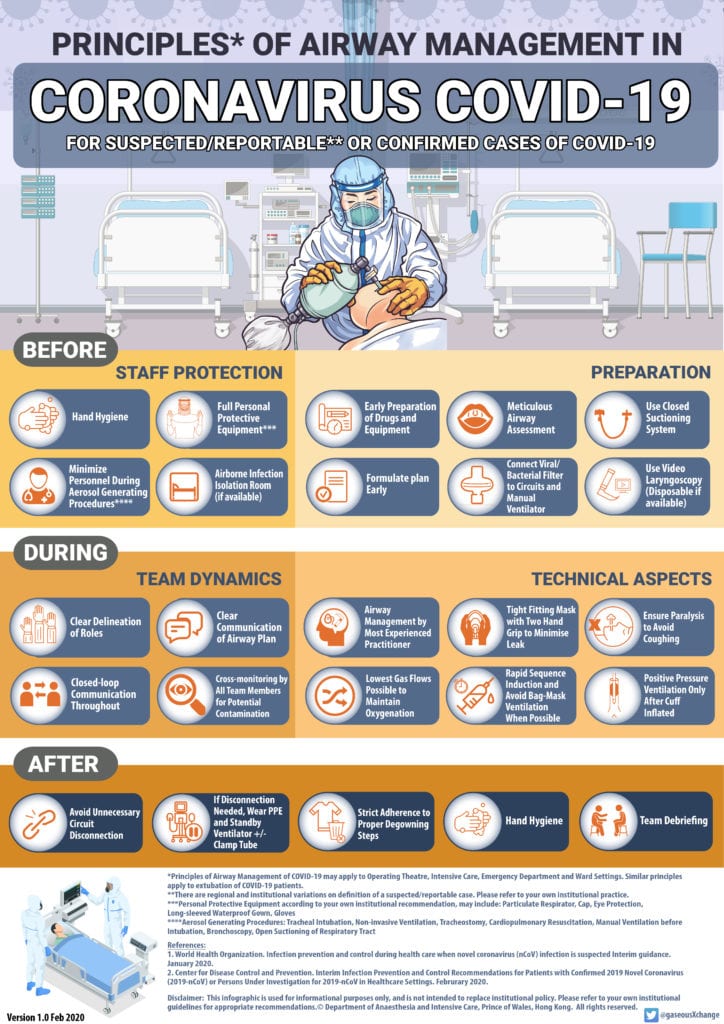
References
- Caputo, K. M., Byrick, R., Chapman, M. G., Orser, B. J., & Orser, B. A. (2006). Intubation of SARS patients: infection and perspectives of healthcare workers. Canadian Journal of Anesthesia, 53(2), 122.
- Dubé, M. M., Reid, J., Kaba, A., Cheng, A., Eppich, W., Grant, V., & Stone, K. (2019). PEARLS for Systems Integration: A Modified PEARLS Framework for Debriefing Systems-Focused Simulations. Simulation in Healthcare, 14(5), 333–342. https://doi.org/10.1097/SIH.0000000000000381
- Eppich, W., & Cheng, A. (2015). Promoting Excellence and Reflective Learning in Simulation (PEARLS). Simulation in Healthcare: The Journal of the Society for Simulation in Healthcare, 10(2), 106–115. https://doi.org/10.1097/SIH.0000000000000072
- Hunt, E. A., Duval-Arnould, J. M., Nelson-McMillan, K. L., Bradshaw, J. H., Diener-West, M., Perretta, J. S., & Shilkofski, N. A. (2014). Pediatric resident resuscitation skills improve after “Rapid Cycle Deliberate Practice” training. Resuscitation, 85(7), 945–951. https://doi.org/10.1016/j.resuscitation.2014.02.025
- Lau, J. T. F., Fung, K. S., Wong, T. W., Kim, J. H., Wong, E., Chung, S., … Cheng, A. (2004). SARS Transmission among Hospital Workers in Hong Kong. Emerging Infectious Diseases, 10(2), 280–286. https://doi.org/10.3201/eid1002.030534
- O’Regan, S., Molloy, E., Watterson, L., & Nestel, D. (2016). Observer roles that optimise learning in healthcare simulation education: a systematic review. Advances in Simulation, 1(1), 4. https://doi.org/10.1186/s41077-015-0004-8
- Patterson, M. D., Geis, G. L., Falcone, R. A., LeMaster, T., & Wears, R. L. (2013). In situ simulation: Detection of safety threats and teamwork training in a high risk emergency department. BMJ Quality and Safety, 22(6), 468–477. https://doi.org/10.1136/bmjqs-2012-000942
- Phrampus, P. E., O’Donnell, J. M., Farkas, D., Abernethy, D., Brownlee, K., Dongilli, T., & Martin, S. (2016). Rapid development and deployment of ebola readiness training across an academic health system the critical role of simulation education, consulting, and systems integration. Simulation in Healthcare, 11(2), 82–88. https://doi.org/10.1097/SIH.0000000000000137
- Pope, S., Baggett, S., Dubois, E. J., Martin, C., & Gore, T. (2014). Using visualization in simulation For infection control. Clinical Simulation in Nursing, 10(12), 598–604. https://doi.org/10.1016/j.ecns.2014.08.005
- Reid, J., Stone, K., Huang, L., & S. Deutsch, E. (2016). Simulation for Systems Integration in Pediatric Emergency Medicine. Clinical Pediatric Emergency Medicine, 2016; 17(3): 193–199. https://doi.org/10.1016/j.cpem.2016.05.006
- Rudolph JW, Raemer DB, Simon R. Establishing a safe container for learning in simulation the role of the presimulation briefing. Simulation in Healthcare, 2014; 9(6): 339–349. https://doi.org/10.1097/SIH.0000000000000047
- Van Merriënboer, J. J. G., & Kirschner, P. A. (2017). Ten steps to complex learning: A systematic approach to four-component instructional design. Routledge.
- Wu, Z., & McGoogan, J. M. (2020). Characteristics of and Important Lessons From the Coronavirus Disease 2019 (COVID-19) Outbreak in China: Summary of a Report of 72 314 Cases From the Chinese Center for Disease Control and Prevention. JAMA, 2019, 24–27. https://doi.org/10.1001/jama.2020.2648
Acknowledgements
Jenny Rudolph, Executive Director, Center for Medical Simulation, Boston, Massachusetts
In-situ simulation team (Vivian Lau, Henry Wong, Thomas Lo, Rosinni Wong, Maggie Sin), Prince of Wales Hospital, Chinese University of Hong Kong, Hong Kong
SARS-CoV-2
novel coronavirus of COVID-19
Dr Albert Chan MBBS, FHKCA, FHKAM (Anaesthesiologist), FANZCA is Associate Consultant, Department of Anaesthesia and Intensive Care, Prince of Wales Hospital and Clinical Assistant Professor (Honorary), Chinese University of Hong Kong, Hong Kong | @gaseousXchange |


This is an amazing resource. Thank you so much.
Anyone who could produce a realistic video drill of an unplanned intubation in the setting of COVID would undoubtedly save a lot of lives.
We need more high-impact resources and we do not have them.
Thanks again.
thank you, Chris, from Merced , calif. you and your team are incredible, and invaluable.
excellent presentation here.
(we met at reanimate3… seems like forever ago.
tom