George Mallory

George Kenneth Mallory (1900-1986) was an American pathologist
GK Mallory was an American pathologist whose name endures through the Mallory-Weiss Syndrome/lesion/tear. Born into a dynasty of distinguished pathologists, he followed in the footsteps of his father Frank Burr Mallory (1862-1941) for whom Mallory’s bodies are named; and older brother Tracy Burr Mallory (1896–1951) a distinguished pathologist who succeeded James Homer Wright as Chief of Pathology at Massachusetts General Hospital in Boston.
Beyond gastroenterology, Mallory made landmark to cardiac pathology. In 1939, in collaboration with Paul Dudley White and Jorge Salcedo-Salgar, he co-authored a definitive study on the temporal histological changes of myocardial infarction based on 72 autopsy cases. This work was the first to systematically correlate infarct age with histological features, establishing diagnostic criteria that remain foundational in forensic and clinical cardiology.
Mallory served as Professor and Chair of Pathology at Boston University School of Medicine and Director of the Mallory Institute of Pathology from 1951 until his retirement in 1965. His publications include important contributions to renal and hepatic pathology, including a histochemical study of Mallory’s hyaline in liver disease.
Biographical Timeline
- Born February 14, 1900 in Boston, Massachusetts, son of Frank Burr Mallory (1862-1941). Younger brother of Tracy Burr Mallory (1896–1951).
- 1922 – Graduated from Harvard College.
- 1926 – Graduated MD cum laude from Harvard Medical School.
- 1926–1928 – Completed internship in internal medicine at Boston City Hospital.
- 1929 – Co-authored seminal paper with Soma Weiss (1898-1942) describing haemorrhagic lacerations at the gastric cardia due to vomiting, Mallory–Weiss lesions.
- 1930–1933 – Undertook further pathology training in Europe: Hamburg with Theodor Fahr at Eppendorfer Krankenhaus. Vienna with Hermann Chiari (1851–1916) at Allgemeine Krankenhaus.
- 1933 – Appointed Assistant Pathologist at Boston City Hospital under Frederic Parker Jr.; joined the newly established Mallory Institute of Pathology.
- 1949 – Professor of Pathology at Boston University School of Medicine
- 1951 – Succeeded Frederic Parker Jr. as Chief of Pathology and Director of the Mallory Institute of Pathology at Boston City Hospital.
- 1953 – Co-authored follow-up study on Mallory-Weiss syndrome, expanding its clinical understanding.
- 1965 – Retired as Director of the Mallory Institute of Pathology.
- 1966 – Appointed Emeritus Professor of Pathology at Boston University.
- Died April 8, 1986 in Needham, Massachusetts.
Medical Eponyms
Mallory–Weiss Lesion (1929)
The characteristic of this lesion are longitudinal mucosal lacerations in the distal oesophagus and proximal stomach, which are usually associated with forceful or prolonged vomiting, retching or coughing. Originally identified in alcoholic patients presenting with severe upper gastrointestinal haemorrhage.
First described in 1929 by George Kenneth Mallory and Soma Weiss (1898–1942), who published 15 cases demonstrating that bleeding was due to mucosal fissures at the cardia, not varices or peptic ulcers.
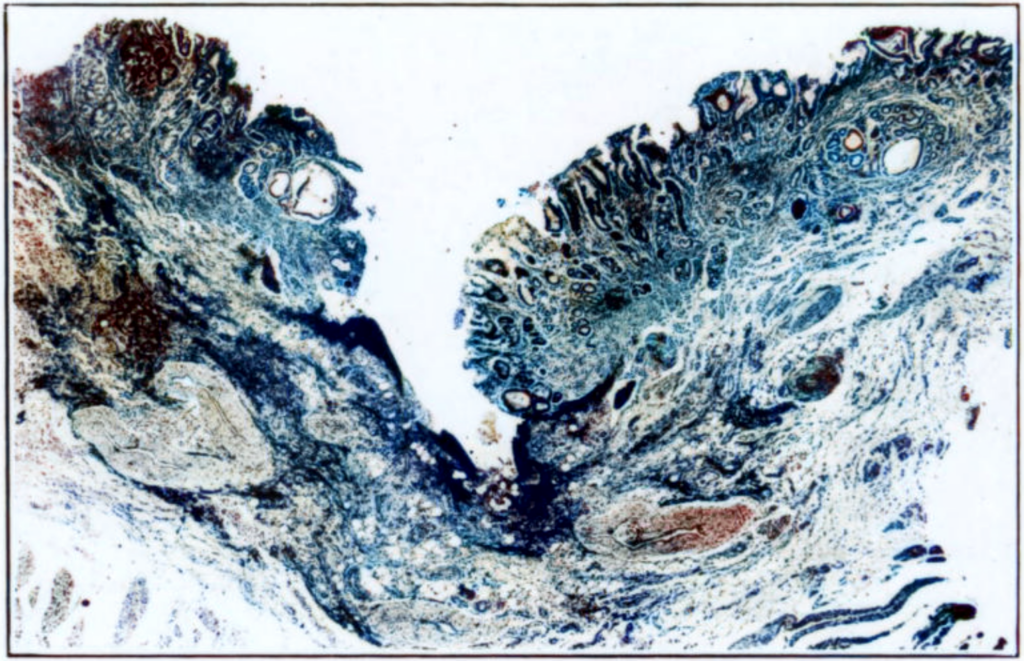
1932 Weiss and Mallory and Weiss rexpanded their observations with two fatal cases.
- Case 1: A “classical” presentation: a man with massive haematemesis after heavy alcohol intake; autopsy revealed a deep acute mucosal laceration rupturing an artery.
- Case 2: More atypical: a man with prior small-volume haematemesis, presenting with an “acute abdomen.” At autopsy, a longitudinal ulcerative lesion at the gastroesophageal junction was found, which had perforated into the mediastinum, causing empyema.
From these cases, Mallory and Weiss proposed a progression: acute laceration → chronic ulcer → perforation, suggesting that repeated vomiting could transform a mucosal tear into a chronic longitudinal ulcer. This concept might now be viewed as overlapping with conditions such as Barrett’s oesophagus.
They also situated their work in historical context:
- Johann Friedrich Hermann Albers (1802–1865) first to describe an ulcer in the lower oesophagus.
- Heinrich Irenaeus Quincke (1842–1922) noted oesophageal “peptic” ulcers.
- Georges Dieulafoy (1839–1911) reported gastric lesions, but Mallory and Weiss differentiated their syndrome on histological grounds.
Key Medical Contributions
Myocardial Infarction Pathology: Co-authored The speed of healing of myocardial infarction with Paul Dudley White and Jorge Salcedo-Salgar. This landmark study of 72 autopsies established the sequential histological changes following myocardial infarction, providing the first reliable histological criteria to date infarcts—a critical advance for both diagnosis and medicolegal pathology.
Renal Pathology: Published key experimental work on acute and chronic pyelonephritis, contributing to the understanding of renal inflammation and its progression.
Hepatic Pathology: Advanced the study of alcoholic liver disease through histochemical characterization of Mallory bodies (hyaline inclusions), continuing the work initiated by his father, Frank Burr Mallory.
Major Publications
- Mallory GK, Weiss S. Hemorrhages from lacerations of the cardiac orifice of the stomach due to vomiting. American Journal of the Medical Sciences, 1929; 178: 506–15 [Mallory-Weiss syndrome; Mallory-Weiss lesion]
- Weiss S, Mallory GK. Lesions of the cardiac orifice of the stomach produced by vomiting. Journal of the American Medical Association, Chicago, 1932; 98(16): 1353-1355 [Mallory-Weiss syndrome; Mallory-Weiss lesion]
- Mallory GK, White PD, Salcedo-Salgar J. The speed of healing of myocardial infarction: A study of the pathologic anatomy in seventy-two cases. American Heart Journal 1939; 18(6): 647-671
- Decker JP, Zamcheck N, Mallory GK. Mallory-Weiss syndrome: hemorrhage from gastroesophageal lacerations at the cardiac orifice of the stomach. N Engl J Med. 1953 Dec 10;249(24):957-63.
References
Biography
- Haubrich WS. Mallory and Weiss of the Mallory-Weiss Syndrome. Gastroenterology, 2001; 121(3): 541
- van den Tweel JG. Mallory, George Kenneth (1900–1986). In: Pioneers in Pathology. 2017: 357-360
Eponymous terms
- Herbella FA, Matone J, Del Grande JC. Eponyms in esophageal surgery, part 2. Dis Esophagus. 2005;18(1):4-16.
- Louis DN, O’Brien MJ, Young RH. The flowering of pathology as a medical discipline in Boston, 1892-c.1950: W.T. Councilman, FB Mallory, JH Wright, SB Wolbach and their descendants. Mod Pathol. 2016 Sep;29(9):944-61.
Eponym
the person behind the name
Graduated Medicine in 2020 from Queens University Belfast. Interested in Internal Medicine.
BA MA (Oxon) MBChB (Edin) FACEM FFSEM. Emergency physician, Sir Charles Gairdner Hospital. Passion for rugby; medical history; medical education; and asynchronous learning #FOAMed evangelist. Co-founder and CTO of Life in the Fast lane | On Call: Principles and Protocol 4e| Eponyms | Books |

