James Bain
James Bain (1934 – ) Canadian anesthesiologist
Inventor of the Bain breathing circuit; a prototype initially regarded by his university as a ‘bunch of plastic;’ was a significant advance in anaesthesia and a modification of the Mapleson D circuit. It was used to deliver anaesthesia to more than 30,000 cases each year at their institution alone and over its decades of use, over a million anaesthetics worldwide.
Although its use has been now all but phased out, the Bain circuit was once a contender for the title of ‘universal breathing system.’
Biography
- Born in Listowel, Ontario in 1934
- 1960-1964 graduated medical school at University of Western Ontario and commenced anaesthesia training in Toronto and London
- 1965 – joins Wolfgang Spoerel (Professor and Chairman at University of Western Ontario) at Victoria Hospital, London
- 1971 – begins designing and developing a ventilator system based on the Mapleson D configuration; a prototype circuit is completed in a single afternoon with help from Anaesthetic technician Henry Letanche. Clinical studies are conducted on the home-made circuits together with Spoerel. Preliminary results are presented to the Canadian Society of Plastic Surgeons in Toronto and at the Canadian Anaesthetists’ Society annual meeting in Halifax
- 1972 – Results are officially published by Bain and Spoerel in the Canadian Anaesthetists’ Society Journal titled “A streamlined anaesthetic system”; privately applies for a patent; system now known as “Bain breathing circuit”
- 1973 – Bain system gains popularity especially among head and neck surgeries; new university hospital in London opens and each operating theatre is fitted with Bain circuits
- 1975 – Simon Pethick, an anaesthesia resident in Calgary describes the use of an oxygen flush to check for circuit connection; early Bain systems consisted of opaque tubing and thus proximal disconnections in the circuit could not be detected by visual inspection
- 1980-1990’s pulse oximetry, capnography and anaesthetic agent monitors become the standard and there is a shift to low flow anaesthesia. Bain circuit falls out of fashion where high FGFs and high theatre pollution makes it uneconomical and environmentally unfriendly; trends change from need for large minute volumes to more physiological modes of ventilation
Medical Eponyms
Bain Circuit
The Bain breathing Circuitn (modified Mapleson D coaxial system) was Bain and Spoerel’s answer to Head and Neck anaesthesia. Standard anaesthetic machines at the time were large and bulky and clumsy for plastic surgery procedures where the APL valve was obtrusively close to the surgical field and the weight like an anchor pulling on the tracheal tube.
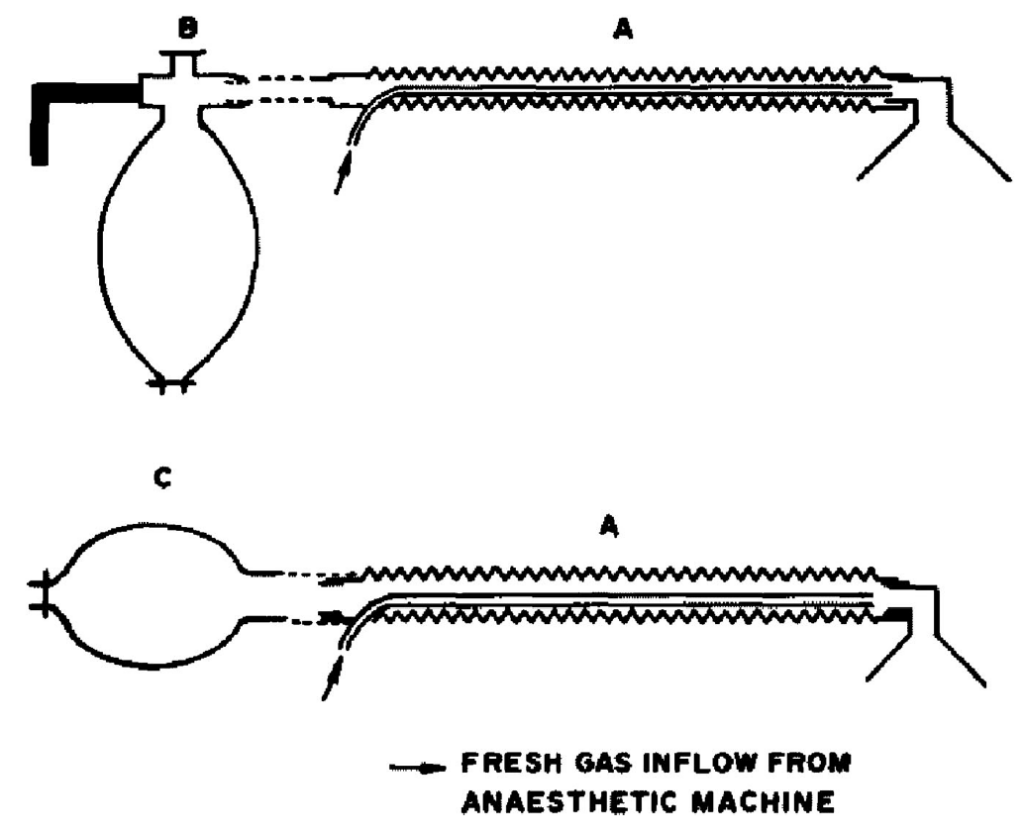
Surgical procedures about the head and neck require an anaesthetic system which is light in weight, does not create facial distortion and does not cause excessive drag on the endotracheal tube
Bain JA, Spoerel WE. 1972
The Bain circuit is a lightweight co-axial system of a tube within a tube. It comprises a 1.8m length of light weight conductive corrugated plastic tubing, 22mm in diameter through whose length, an inner tube (diameter 7mm) delivers fresh gas flow from the anaesthetic machine. The outer tube receives the expired gas and provides a low resistance pathway with counter-current warming, humidification and admixture of gases. A reservoir bag and valve added to the non-patient end makes this system ‘Mapleson D’ and a ‘Mapleson E’ if an open-ended bag without a valve is used.
There is controversy surrounding the appropriate FGF and minute volume. Bain recommended an FGF of 70ml/kg with controlled ventilation and a FGF of 100ml/kg for spontaneous ventilation to achieve normocapnia. This translated to a FGF of one to two times the minute volume. This was later disputed by Rose and Byrick and later again by Conway, who argued that FGF three times greater than the minute ventilation was needed to prevent rebreathing. The original publication does indeed fall short by todays scientific standards where anaesthetic technique is not standardised, selection to patient cohorts for higher and lower FGF is not described and measurements of arterial blood gases occurred in only few patients.
The thick opaque tubing made inner tube disconnections difficult to visually detect. Foëx described in his publication ‘A test for co-axial circuits’:
We have recently had cause to doubt that the structural integrity of a co-axial ‘Bain’ circuit can be regarded as inevitable
Foëx P, Crampton Smith A. 1972
Breaches in the integrity of the circuit resulted in reduced FGF, increased dead space and ultimately severe hypercarbia and hypoxia. The tubing could also kink, twist or become obstructed with secretions. The Pethick test was later developed in response to this and used the oxygen flush and Venturi effect to check for circuit integrity. Despite the issues and controversies with the circuit, the Bain system was widely used and offered many advantages at the time, including its light weight, ease for sterilization and scavenging and the improved accessibility with the relocated APL valve away from the patient end. Although largely obsolete now, it was a stepping stone towards the development of more modern and efficient anaesthetic systems used today.
Bain system stills remains popular in India and other countries where monitoring is not available, however in current practice, its use is largely limited and superseded by more modern systems
Major Publications
- Bain JA, Spoerel WE. Observation on the use of cuffed tracheostomy tubes (with particular reference to the James tube). Can Anaesth Soc J. 1964 Nov;11:598-608.
- Bain JA, Spoerel WE. A streamlined anaesthetic system. Can Anaesth Soc J. 1972 Jul;19(4):426-35
- Bain JA, Spoerel WE. Flow requirements for a modified Mapleson D system during controlled ventilation. Can Anaesth Soc J. 1973 Sep;20(5):629-36
- Bain JA, Spoerel WE. Prediction of arterial carbon dioxide tension during controlled ventilation with a modified Mapleson D system. Can Anaesth Soc J. 1975 Jan;22(1):34-8
- Bain JA, Reid D. A simple way to ventilate babies utilizing a Mark VII Bird Ventilator and a Modified Mapleson “D” Breathing Circuit. Can Anaesth Soc J. 1975 Mar;22(2):202-7.
- Bain JA, Spoerel WE. Carbon dioxide output and elimination in children under anaesthesia. Can Anaesth Soc J. 1977 Sep;24(5):533-9.
- Spoerel WE, Bain JA. Fresh gas flows. Br J Anaesth. 1983 Oct;55(10):1039-40.
- Spoerel WE, Bain JA. Anaesthetic breathing systems. Br J Anaesth. 1986 Jul;58(7):819-21.
References
Biography
- Maltby JR. James Bain. In: Notable Names in Anaesthesia. The Choir Press 2013: 10-12
Eponymous terms
- Henville JD, Adams AP. The Bain anaesthetic system An assessment during controlled ventilation. Anaesthesia. 1976;31:247-256
- Foëx P, Crampton Smith A. A test for co-axial circuits. Anaesthesia 1977; 32: 294.
- Humphrey D. The Lack, Magill and Bain anaesthetic breathing systems: a direct comparison in spontaneously-breathing anaesthetized adults. J R Soc Med. 1982 Jul;75(7):513-24.
- Cooper R. From the Journal archives: A streamlined anesthetic system: the Bain (and Spoerel) circuit 40 years later. Can J Anaesth. 2014 Jun;61(6):587-90.
[cite]
FACEM. Emergency physician and researcher at Sir Charles Gairdner Hospital, Perth
BA MA (Oxon) MBChB (Edin) FACEM FFSEM. Emergency physician, Sir Charles Gairdner Hospital. Passion for rugby; medical history; medical education; and asynchronous learning #FOAMed evangelist. Co-founder and CTO of Life in the Fast lane | On Call: Principles and Protocol 4e| Eponyms | Books |

