Sheep Pox
Sure….. the diagnosis and management of wide-complex tachyarrhythmia is an exciting part of emergency medicine.
Sometimes however, our attention is drawn to other clinical entities which may not attract the same bright lights and sensational headlines, but still stimulate learning and can lead to interesting questions being raised.
Questions like…..
Q1. What is Orf?
Answer and interpretation
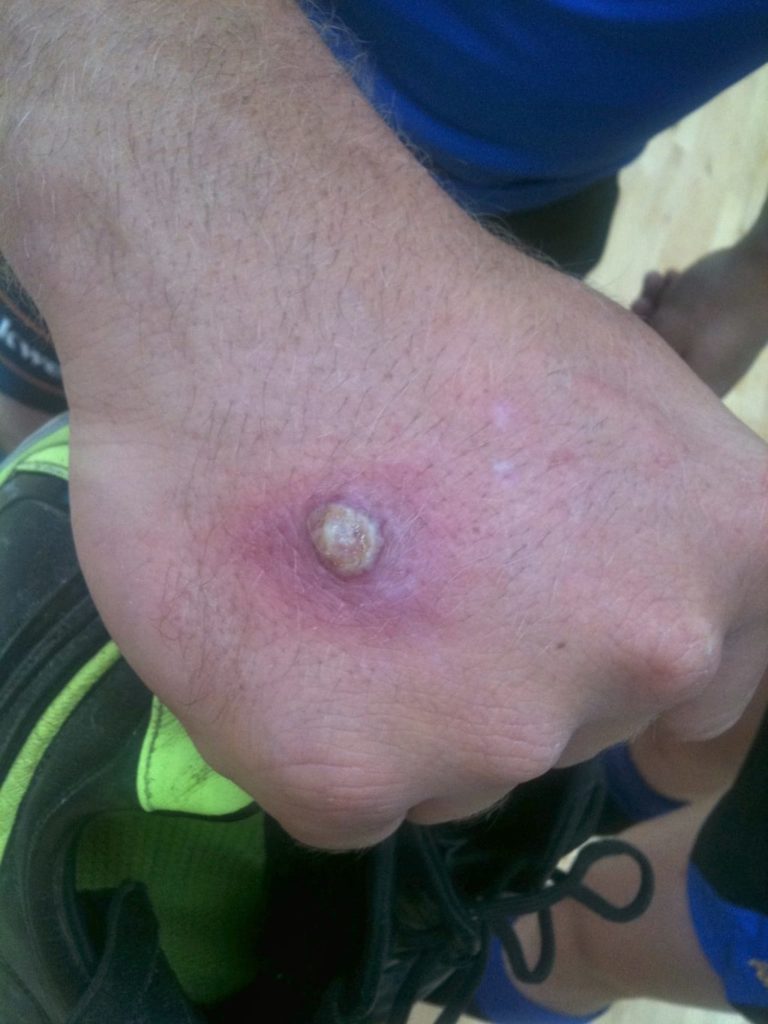
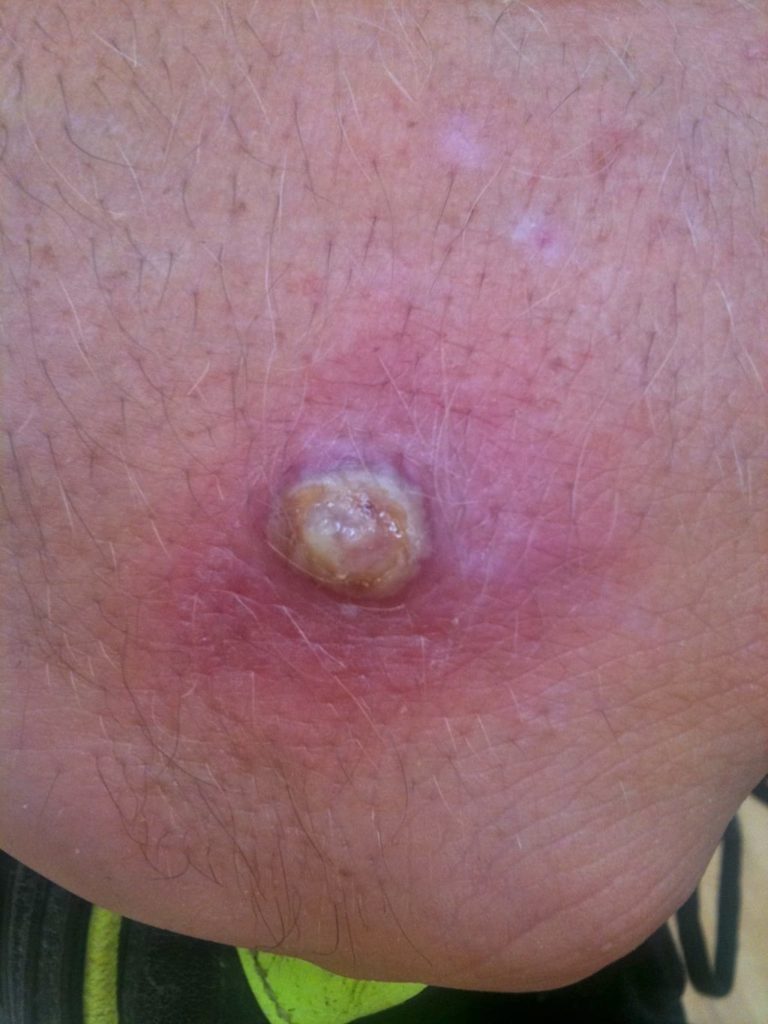
Orf is a zoonotic infection occurring in humans which is characterised by erythematous weeping nodules found most commonly on the hands and feet.
Q2. What causes Orf?
Answer and interpretation
Orf is caused by the orf virus which is of the Parapoxvirus genus of the family Poxviridae.
This virus causes a highly contagious disease among small ruminant animals (e.g. sheep and goats) and is endemic to most countries of the world. In veterinary medicine it also goes by the names contagious pustular dermatitis, contagious ecthyma, sheep pox and my personal favourite – scabby mouth.
Q3. How is it acquired?
Answer and interpretation

It is transmitted by direct contact from infected animals and is usually described as an occupational disease occurring in farmers, shepherds and shearers and also in abattoir workers, butchers and veterinarians. It is not strictly an occupational disease however with some interesting case reports of the disease occurring after animal contact during the “feast of sacrifice“
Q4. How does it present?
Answer and interpretation
Orf usually appears as a small papule occurring on the hand or finger about one week after animal contact.
There may be multiple lesions and it may occur elsewhere such as on the face or penis (depending on where the unhygienic individual has wiped their hands after touching the dirty beast). The lesion grows to form a pustule usually 2-3cm in diameter.
Six clinical stages have been described; maculopapular, target, acute, regenerative, papillomatous and regressive. It may be associated with a low-grade fever, malaise and lymphadenopathy and is usually tender and susceptible to haemorrhage in the early stages.
Q5 What is the differential diagnosis?
Answer and interpretation
The clinical manifestations and exposure risks have overlap with other zoonoses such as:
- milker’s nodules
- cowpox
- mycobacteruim marinum (fish tank granuloma), and
- cutaneous anthrax (one not to miss)
The differential also includes:
- herpetic paronychial abscess
- pyogenic granuloma
- deep fungal infection
- keratoacanthoma, and
- malignant tumours such as basal cell carcinoma (BCC).
Q6. How is the diagnosis confirmed?
Answer and interpretation
The diagnosis should be suspected primarily on clinical assessment through a history of occupation/animal exposure and from the duration and nature of the lesion.
Serological testing may detect an antibody response but cannot discriminate Orf from other parapoxviruses. Electron microscopy of the crust or the fluid within the lesion may similarly confirm parapoxvirus but not identify orf virus specifically. Polymerase chain reaction (PCR) using tissue, crust or fluid will confirm orf virus as the causative agent.
Q7. What is the prognosis?
Answer and interpretation
Orf is usually a self-limiting disease that resolves typically within 6 weeks usually without a residual scar.
In the immunocompromised patient it may be an entirely different kettle of fish and develop into a progressive lesion resistant to surgical debridement and topical treatment.
Q8. What is the treatment?
Answer and interpretation
As the lesion will resolve spontaneously, treatment is supportive and symptomatic with a simple dressings, a topical antiseptic agent to prevent secondary infection and splinting of the infected finger may also be helpful.
Topical treatment with the antiviral agent cidofovir or the immune response modifier imiquimod have been described in certain case reports. Surgical treatments such as curettage and electrodesiccation or shave excision have been used, as has cryotherapy with liquid nitrogen. It is important to be aware of orf when confronted with an unusual lesion on the hand or finger and seek a history of animal exposure which may lead you to the diagnosis of orf.
This combined with appropriate laboratory testing can confirm the diagnosis and save the patient from unwarranted and over aggressive treatments such as amputation (!).
References
- Büttner M, Rziha HJ. Parapoxviruses: from the lesion to the viral genome. J Vet Med B Infect Dis Vet Public Health. 2002 Feb;49(1):7-16. Review. PMID: 11911596.
- Centers for Disease Control and Prevention (CDC). Orf virus infection in humans–New York, Illinois, California, and Tennessee, 2004-2005. MMWR Morb Mortal Wkly Rep. 2006 Jan 27;55(3):65-8.PMID: 16437055.
- Hosamani M, Scagliarini A, Bhanuprakash V, McInnes CJ, Singh RK. Orf: an update on current research and future perspectives. Expert Rev Anti Infect Ther. 2009 Sep;7(7):879-93. Review. PMID: 19735227.
- Scagliarini A, Gallina L, Dal Pozzo F, Battilani M, Ciulli S, Prosperi S, Pampiglione S. Diagnosis of orf virus infection in humans by the polymerase chain reaction. New Microbiol. 2004 Oct;27(4):403-5. PMID: 15646056.
- Uzel M, Sasmaz S, Bakaris S, Cetinus E, Bilgic E, Karaoguz A, Ozkul A, Arican O. A viral infection of the hand commonly seen after the feast of sacrifice: human orf (orf of the hand). Epidemiol Infect. 2005 Aug;133(4):653-7. PMID: 16050510; PMCID: PMC2870292.