The Red Eye Challenge
aka Ophthalmology Befuddler 002
Things are humming along nicely in the ‘Fast track’ area of the emergency department. You check the triage note of the next patient – RED EYE is written capitals.
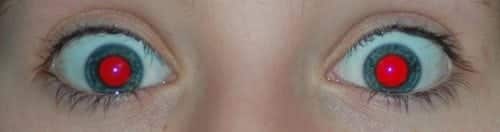
Q1. There are many causes of ‘red eye’ — how can they broken down as an approach to diagnosis and management?
Answer and interpretation
Of course there are myriad ways of doing this. I like Jeff Mann’s approach — he has a simple way of breaking the causes down into 3 groups:
- extra-ocular causes: (e.g. orbital cellulitis, cavernous sinus thrombosis, carotid-cavernous fistula, cluster headache)
- external eye disease: (e.g. eye lid and conjunctival disease)
- internal eye disease: (e.g. iritis, glaucoma)
Once an extra-ocular cause is excluded (this will be discussed in a later post), a helpful approach is to divide up the causes of red eye as follows:
- Painless — is there diffuse or localised redness?
- Painful?
The next step is to consider which structures are abnormal:
- Lid, conjunctiva, cornea, sclera, or anterior chamber?
This approach gets you off to a good start in narrowing down the causes of a red eye.
Q2. What are the causes of a painless red eye?
Answer and interpretation
These can be classified according to whether the redness is diffuse or localised.
- diffuse: usually this is an eyelid abnormality as most cases of conjunctivitis are painful: e.g. blepharitis, ectropion, trichiasis, entropion, eyelid lesion (e.g. tumour, stye)
- localised: e.g. pterygium, corneal foreign body, ocular trauma, subconjunctival hemorrhage
If you’re stuck for a differential diagnosis, fall back on working through the anatomical components of the eye and running through a pathophysiological sieve.
Q3. What are the causes of a painful red eye?
Answer and interpretation
These can be classified according which structure is abnormal:
- abnormal cornea: e.g. herpes simplex keratitis, corneal ulcer, marginal keratitis, corneal abrasion,
- abnormal eyelid: e.g. chalazion/ stye, acute blepharitis, herpes zoster ophthalmicus
- diffuse conjunctival injection: e.g. viral conjunctivitis, allergic conjunctivitis, bacterial conjunctivitis, dry eyes, acute glaucoma
- ciliary injection/ scleral involvement: e.g. scleritis
- anterior chamber involvement: e.g. acute anterior uveitis (iritis), hypopyon, hyphema
Q4. What 4 features usually suggest an internal cause of a red eye?
Answer and interpretation
- severe eye pain (unrelieved by topical anesthetics)
- impaired vision
- poorly reactive pupils
- abnormal slit lamp examination +/- abnormal intra-ocular pressure
Q5. What 6 features on history and exam suggest an external cause for red eye?
Answer and interpretation
- pain sensation is usually itching, gritty, scratching, or burning (not a deep-seated ache)
- pain is significantly improved by topical anesthetics
- eye discharge is common: (watery, mucoid or purulent depending on etiology)
- photophobia and blepharospasm may be present
- visual acuity is usually normal or near-normal (there may be some blurriness)
- preauricular lymphadenopathy may be present. e.g. viral or chlamydial conjunctivitis
Q6. What 7 features on exam should be present if the cause of a red eye is not serious?
Answer and Interpretation
- cornea clear
- anterior chamber clear
- pupils normal in size and reactivity
- visual acuity normal or near-normal
- extraocular eye movements normal
- proptosis absent
- eyeball is not tender on palpation
Q7. What is the likely diagnosis of a red eye in a middle-aged woman with the following findings?
Quick Quiz…
Mid-dilated unreactive pupil, steamy cornea, peri-orbital pain, nausea/vomiting and increased intra-ocular pressure
Answer
angle closure glaucoma
Small irregular pupil, deep-seated eye pain that is worse on eye movement and accommodation, consensual photophobia and positive slit lamp signs of flare and cells
Answer
iritis
Deep-seated eye pain that is worse at rest and at night, pain on palpation of the eye and violaceous appearance of the sclera
Answer
scleritis
Proptosis, congested chemosis, painful external ophthalmoplegia, and visual loss with a relative afferent pupillary defect
Answer
orbital cellulitis or cavernous sinus venous thrombosis
Q9. What potentially serious causes of a red eye are suggested by the following features on history or examination?
Quick Quiz…
Severe eye aching
Answer
Iritis, keratitis, acute angle-closure glaucoma, scleritis, orbital cellulitis, cavernous sinus thrombosis (CST)
Prominent photophobia
Answer
Iritis, keratitis
Impaired vision
Answer
Iritis, keratitis, acute angle-closure glaucoma, orbital cellulitis, CST
Cloudy cornea
Answer
Keratitis, acute angle-closure glaucoma
Corneal opacification
Answer
Keratitis – chemical or infectious
Circumcorneal conjunctival injection
Answer
Iritis, keratitis
Cloudy anterior chamber
Answer
Iritis
Pain on eyeball palpation
Answer
Scleritis (+++), orbital cellulitis, CST
Proptosis
Answer
Orbital cellulitis, CST, posterior scleritis
Impaired, or painful, extraocular eye movements
Answer
Orbital cellulitis
Fever, toxic appearance
Answer
Orbital cellulitis (+), CST (++)
Hyperpurulent discharge from an “angry” eye
Answer
Gonococcal conjunctivitis/endophthalmitis
Prominent nausea and vomiting
Answer
Acute angle-closure glaucoma
Small, irregular, poorly-reactive pupil
Answer
Iritis
Fixed mid-dilated pupil
Answer
Acute angle-closure glaucoma
Increased intra-ocular pressure
Answer
Acute angle-closure glaucoma, iritis (secondary complication)
History of connective tissue disease, or granulomatous disease
Answer
Iritis, scleritis
References
- Mahmood AR, Narang AT. Diagnosis and management of the acute red eye. Emerg Med Clin North Am. 2008 Feb;26(1):35-55, vi. PMID: 18249256.
- NSW Statewide Opthalmology Service. Eye Emergency Manual — An illustrated Guide. [Free PDF]
OPHTHALMOLOGY BEFUDDLER
Chris is an Intensivist and ECMO specialist at The Alfred ICU, where he is Deputy Director (Education). He is a Clinical Adjunct Associate Professor at Monash University, the Lead for the Clinician Educator Incubator programme, and a CICM First Part Examiner.
He is an internationally recognised Clinician Educator with a passion for helping clinicians learn and for improving the clinical performance of individuals and collectives. He was one of the founders of the FOAM movement (Free Open-Access Medical education) has been recognised for his contributions to education with awards from ANZICS, ANZAHPE, and ACEM.
His one great achievement is being the father of three amazing children.
On Bluesky, he is @precordialthump.bsky.social and on the site that Elon has screwed up, he is @precordialthump.
| INTENSIVE | RAGE | Resuscitology | SMACC
