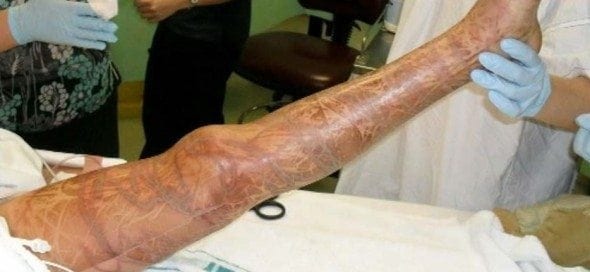
Box Jellyfish
The Box Jellyfish is found in the Northern waters of Australia. It has a ferocious reputation having been responsible for a number of deaths in Australia with the majority of recent deaths in children. Fortunately most of the stings respond well to simple first aid and patients should be reassured. If an arrest is going to occur it typically occurs within 5 minutes likely secondary to a cardiac toxin affecting the calcium channels.
The classic history if of someone on the tropical waters of Australia between November and April who has immediate pain after a jellyfish sting associated with a crosshatched pattern of welts on their skin.
Resus
Potential life threats include:
- Cardiac arrest – undiluted antivenom should be given as a rapid push unto 6 ampoules and continue with advanced life support along usual guidelines. If the antivenom fails, 10 mol of IV magnesium should also be given. It is important to continue prolonged CPR as good outcomes have been achieved
- Hypotension or hypertension
- Cardiac dysrhythmias
Risk Assessment
Typical symptoms include:
- Immediate severe pain, typically lasts 8 hours with linear welts in a crosshatched pattern. In 25-30% of cases the tentacles are still attached
- Systemic features mentioned above in the resuscitation section
- Delayed hypersensitivity reactions occur in at least 50% of patients and manifest as pruritic erythema at the original sting site and can last up to two weeks.
Supportive Care
- Analgesia Initially simple paracetamol and ibuprofen may suffice but if the pain is refractory IV opiates such as morphine 0.1 mg/kg every 10 minutes should be effective.
- Vinegar Has been effective for controlling pain and stopping any further discharge from any remaining nematocysts – these should then be removed either with your own hands, credit card or sticky tape.
- Ice packs or hot water maybe applied – there is a current debate about which one if more effective.
- Do not apply a dressing as this can cause firing the nematocysts and promote systemic envenomation.
- If the patient has a delayed sensitivity reaction steroid or antihistamine cream maybe effective.
Investigations
- 1. 12 lead ECG for evidence of any dysrhythmias or bundle branch blocks
- Laboratory investigations should selected in the context of trying to rule out other differentials e.g. other reasons for a collapse on the beach if the history is unclear. However, if the patient is haemodynamically unstable check FBC, EUC, magnesium, calcium, phosphate, CK and troponin.
- Chest X-ray for signs of pulmonary oedema.
Differential Diagnosis:
- Bluebottle stings also have immediate pain and skin markings but the pain usually resolves within 1-2 hours and systemic features are rare
- Irukandji syndrome usually has delayed onset of pain and systemic features without skin markings.
- In a diver decompression illness can lead to severe pain and collapse – again skin markings will be absent.
Antivenom
- CSL box Jellyfish Used in the treatment of severe envenomation
- Give 6 ampoules as an IV push in cardiac arrest
- Give 3 ampoules IV diluted in 100 ml of 0.9% saline over 20 minutes to all patients with systemic envenoming (collapse, hypotension or cardiac dysrhythmias). The patient then requires close observation, if no resolution of symptoms, further ampoules can be given up to a maximum of another 3 (6 in total).
- Give 1 ampoule (diluted in 100ml 0.9% saline over 20 minutes) for refractory pain to IV opiates
- See Box Jellyfish antivenom for dosing, administration and complication details
Disposition
- Patients without evidence of envenomation at two hours can be discharged.
- Patients who have received antivenom or IV opiates will need 6 hours observation to observe for clinical resolution of symptoms
Controversies
- Efficacy and role of the CSL Box jellyfish Antivenom
- Recent laboratory work shows that already discharged nematocysts may release more venom with the application of vinegar. Therefore future first aid recommendations may change.
- Ice has been recommended for first aid but it might be heat that is more effective.
LITFL Resources:
- Box Jellyfish Antivenom
- Box Jellyfish (Chironex fleckeri)
- Toxicology Conundrum 010 – Box Jellyfish
- Chris Nickson – Spiders and Stingers – SMACC podcast
- Mark Little – Dangers of the deep – SMACC podcast.
Zeff – James Hayes Fellowship teaching Marine toxinology
References
- Currie BJ, Jacups S. Prospective study of Chironex fleckeri and other box jellyfish stings in the ‘Top End’ of Australia’s Northern Territory. Medical Journal of Australia 2005; 183:161-166
- Currie BJ. Marine Antivenoms. Journal of Toxicology – Clinical Toxicology 2003: 41:301-308 [PMC 12807313]
- Tibballs J. Australian venomous jellyfish, envenomation syndromes, toxins and therapy. Toxicon 2006; 48:830-859 [PMID 16928389]
- Welfare P. Little M, Pereira P, Seymour J. An in-vitro examination of the effect of vinegar on discharged nematocysts of Chironex Fleckeri. Diving and Hyperbaric Medicine 2014; 44(1):30-34
- White J. A clinician’s guide to Australian venomous bites and stings: Incorporating the updated CSL antivenom handbook. Melbourne: CSL Ltd, [PDF Free eBook]

Toxicology Library
TOXINS
Dr Neil Long BMBS FACEM FRCEM FRCPC. Emergency Physician at Kelowna hospital, British Columbia. Loves the misery of alpine climbing and working in austere environments (namely tertiary trauma centres). Supporter of FOAMed, lifelong education and trying to find that elusive peak performance.