CT Case 022
A 40-year-old female, is brought into ED with an abrupt onset of reduced level of consciousness. She had been experiencing several days of headache prior to presentation.
She has no known PHx.
On examination she is GCS 11 (E4V1M6), with weakness of both upper and lower limbs with a pulse rate of 45bpm and BP 153/76.
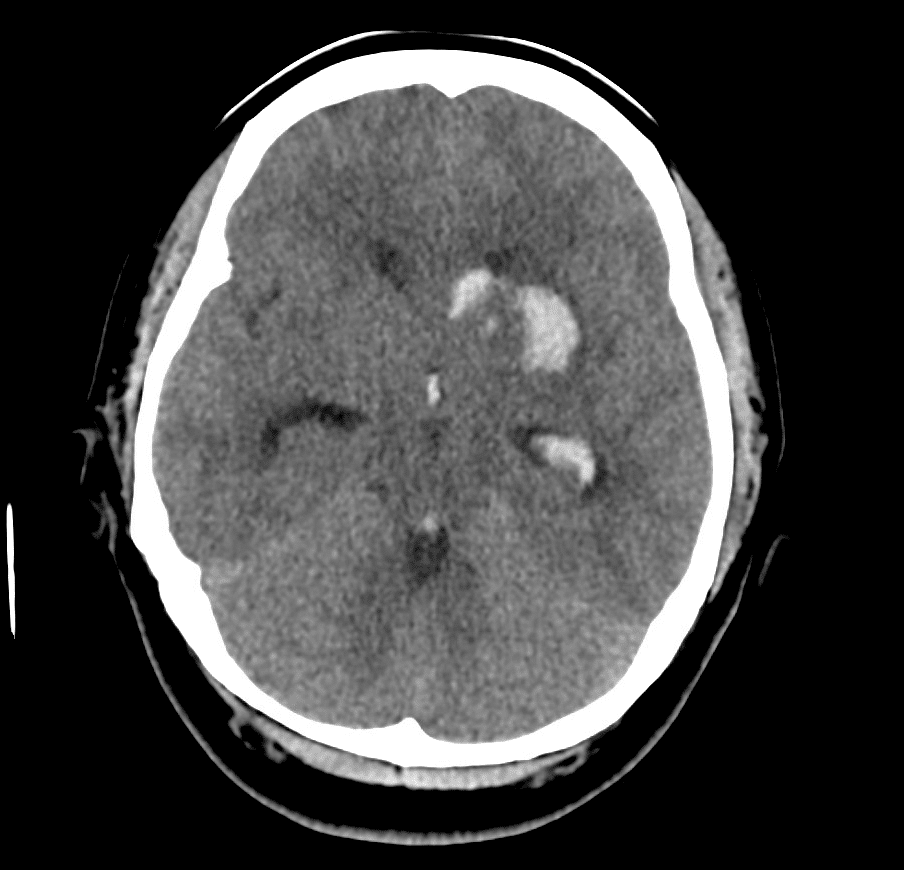

Describe and interpret the CT images
CT INTERPRETATION
There is acute intraparenchymal haemorrhage within the left basal ganglia and external capsule, with mild surrounding oedema.
There is direct intraventricular extension into the frontal horn of the left lateral ventricle with further extension into the third ventricle and cerebral aqueduct.
A basal ganglia haemorrhage is the most common location of haemorrhagic stroke. It is usually a primary intraparenchymal haemorrhage (meaning there is no underlying brain lesion) and is normally the result of poorly controlled long-standing hypertension.
Secondary intraparenchymal haemorrhages occur when there is an underlying lesion, such as a vascular malformation, cerebral venous thrombosis or a tumour, that has led to haemorrhage


CT angiography of the Circle of Willis and post-contrast CT was performed to look for an underlying vascular abnormality
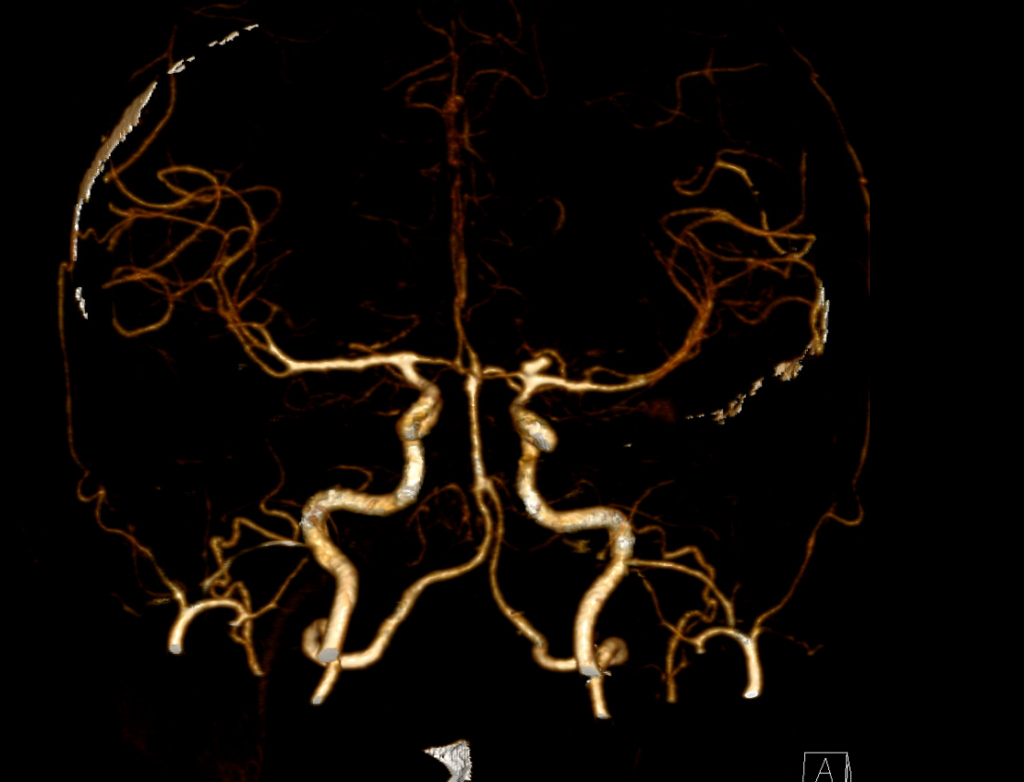
CTA INTERPRETATION
Note, this is called a VRT image. VRT stands for Volume Rendering Technique, it is used to display information in a 3D format, it can help to display anatomy in a more simplified perspective and can assist with surgical planning.
Here we see a bilobed saccular aneurysm arising from the left ICA bifurcation (where it splits into the ACA and MCA).

CLINICAL CORRELATION
Generally, when a cerebral aneurysm ruptures, they cause subarachnoid haemorrhage, however, they can also result in bleeding into the brain parenchyma causing intracerebral haemorrhage, as in this case.
Haemorrhage may decompress into the nearby low resistance ventricular system resulting in intraventricular bleeding and later obstructive hydrocephalus.
This patient had urgent EVD insertion for management of hydrocephalus, as well as endovascular repair (coiling) of her aneurysm.
[cite]
TOP 100 CT SERIES
Dr Leon Lam FRANZCR MBBS BSci(Med). Clinical Radiologist and Senior Staff Specialist at Liverpool Hospital, Sydney
Sydney-based Emergency Physician (MBBS, FACEM) working at Liverpool Hospital. Passionate about education, trainees and travel. Special interests include radiology, orthopaedics and trauma. Creator of the Sydney Emergency XRay interpretation day (SEXI).
Provisional fellow in emergency radiology, Liverpool hospital, Sydney. Other areas of interest include paediatric and cardiac imaging.
Emergency Medicine Education Fellow at Liverpool Hospital NSW. MBBS (Hons) Monash University. Interests in indigenous health and medical education. When not in the emergency department, can most likely be found running up some mountain training for the next ultramarathon.




