Face Masks
OVERVIEW
- multiple types of face mask are used for personal protection
USES
- personal protection
- protection of patient from health care nasopharyngeal secretions
DESCRIPTION
Standard Surgical Facemask (some come with a visor attached)
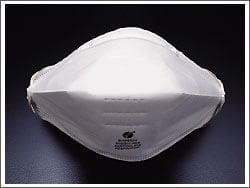
N95 Face Mask (‘duckbill’)
N100 Face Mask
- see here
METHOD OF INSERTION AND/OR USE
- placed over the mouth and nose
OTHER INFORMATION
Surgical Face Mask
- designed to catch bacteria shed in liquid droplets and aerosol form from the wearer’s mouth and nose
- can protect wearer from being splashed in the mouth from body fluids
- also serves as a reminder not to touch mouth or nose
- they do not prevent inhalation of bacteria or viruses
N95
- Used for respiratory droplet infection spread (eg SARS, influenza, Tb) for general presence in room (not procedures)
- used for reverse barrier nursing in severely immunocompromised patients
- certified to filter 95% of particles of a particular test size
- The N refers to the ability to resist oil (N stands for Non-oil resistant). R means resistant to oil and P means oil proof
- filters out the droplets that carry viruses (the viruses themselves would be small enough to pass through the filter)
- should not be put back on if removed
- should be replaced every 6 hours (WHO recommendation)
N100
- more expensive
- highest filtering of respiratory particles/diseases
- CDC recommends masks better than N95 for procedures likely to produce droplets (e.g. airway suctioning, intubation) if airborne precautions are needed

Critical Care
Compendium
Chris is an Intensivist and ECMO specialist at The Alfred ICU, where he is Deputy Director (Education). He is a Clinical Adjunct Associate Professor at Monash University, the Lead for the Clinician Educator Incubator programme, and a CICM First Part Examiner.
He is an internationally recognised Clinician Educator with a passion for helping clinicians learn and for improving the clinical performance of individuals and collectives. He was one of the founders of the FOAM movement (Free Open-Access Medical education) has been recognised for his contributions to education with awards from ANZICS, ANZAHPE, and ACEM.
His one great achievement is being the father of three amazing children.
On Bluesky, he is @precordialthump.bsky.social and on the site that Elon has screwed up, he is @precordialthump.
| INTENSIVE | RAGE | Resuscitology | SMACC