Fever in a spinal patient
aka Microbial Mystery 006
A 20 year-old female with a pre-existing complete spinal cord injury (C5 ASIA A) from an MVA at the age of 2, presents with a 4 day history of fevers, lethargy, headaches and nausea. She has a long and complex medical history, including a sub-rectus sheath intrathecal baclofen pump inserted 2 years ago, several spinal fixation operations for spinal stability (the last 5 years ago), and chronic excoriation of both flanks from scratching.
On examination she is GCS 15, her neurological level is unchanged, she has chronic neck stiffness but no photophobia. She is afebrile, her BP is her usual 90/60 mmHg, HR 100/min. Sats 97% RA, RR 14/min. Apart from the scratch marks, the rest of her skin is intact with no pressure areas. Respiratory, cardiovascular, gastrointestinal, genitourinary and musculoskeletal exams are unremarkable.
Initial investigations reveal an elevated WCC and CRP.
Questions
Q1. What’s the differential diagnosis?
Answer and interpretation
The major diagnoses to consider are:
- Meningitis
- Infected baclofen pump
- Septicemia from skin infection/cellulitis
- Epidural abscess +/- infected internal metal rods
- Another source of sepsis, such as LRTI, UTI, intra-abdominal sepsis
Handy tips:
- Spinal patients with no sensation below their neurological level of injury will not present in the usual fashion if they have pathology below their level
- Approach to sepsis must be open-minded and rely more heavily on investigations and imaging.
- Spinal patients have altered calcium regulation/excretion and renal calculi are much more common, with their complications. They must always be sought for and excluded.
- look for infected pressure sores!
- Other basic principles apply, i.e. find the source, find the bug, treat empirically and narrow therapy as soon as possible, whilst providing concomitant supportive management.
Q2. What investigations would you do next?
Answer and interpretation
Investigations:
- Blood tests:
- Baseline bloods already done, e.g. FBC, UEC, LFTs, lipase, CRP.
- Cultures — see O’Grady et al (2008):
- Blood cultures are vital:
ideally 3 sets in 24hrs from different sites collected in a sterile fashion. 10ml of blood per 20ml BC bottle. - Sputum
- Urine (invariably from a suprapubic catheter in these patients, so this means changing the SPC and taking CSU from new SPC)
- Swabs from excoriated skin
- Blood cultures are vital:
- Chest Xray
- Lumbar puncture:
- this proved technically impossible as the patient had a fused spine
- Interrogation of and CSF sampling from baclofen pump
- CT abdomen for calculi & intra-abdominal sepsis
- MRI brain & spinal cord
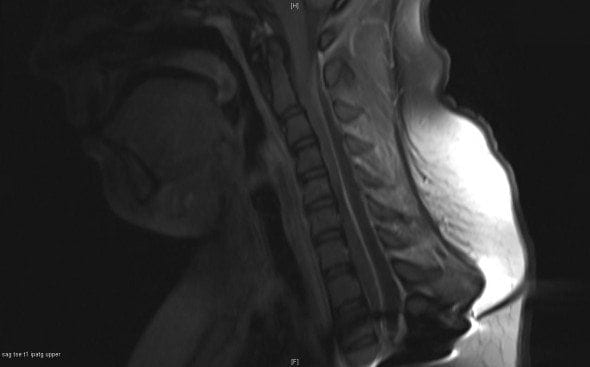
The MRI of the spine is shown below:
Q3. Describe the key findings on the image shown in the answer to Q2?
Answer and interpretation
A large posterior epidural collection compressing the epidural sac involves the visualised spine, with the superior margin at the C2 level. The inferior margin of the collection is not visualised due to artefact from metal internal fixation at the T2 level.
The CSF from the baclofen pump showed no organisms and a normal WCC. Blood cultures grew a penicillin sensitive Staphyloccus aureus, and high dose IV penicillin was commenced.
The patient was taken urgently to theatre and the extensive epidural abscess was drained. Post op the patient woke from anaesthetic, and taken to ICU for recovery.
Find out what happens next in Neurological Mind-boggler 006…
References
- Bersten AD, Soni N. Oh’s Intensive Care Manual (6th edition). Butterworth-Heinemann, 2008.
- Montgomerie JZ. Infections in patients with spinal cord injuries. Clin Infect Dis. 1997 Dec;25(6):1285-90; quiz 1291-2. PMID: 9431366.
- O’Grady NP, et al. Guidelines for evaluation of new fever in critically ill adult patients: 2008 update from the American College of Critical Care Medicine and the Infectious Diseases Society of America. Crit Care Med. 2008 Apr;36(4):1330-49. PMID: 18379262 [fulltext]
- Pradilla G, Ardila GP, Hsu W, Rigamonti D. Epidural abscesses of the CNS. Lancet Neurol. 2009 Mar;8(3):292-300. Review. PMID: 19233039.
CLINICAL CASES
Microbial Mystery
Chris is an Intensivist and ECMO specialist at The Alfred ICU, where he is Deputy Director (Education). He is a Clinical Adjunct Associate Professor at Monash University, the Lead for the Clinician Educator Incubator programme, and a CICM First Part Examiner.
He is an internationally recognised Clinician Educator with a passion for helping clinicians learn and for improving the clinical performance of individuals and collectives. He was one of the founders of the FOAM movement (Free Open-Access Medical education) has been recognised for his contributions to education with awards from ANZICS, ANZAHPE, and ACEM.
His one great achievement is being the father of three amazing children.
On Bluesky, he is @precordialthump.bsky.social and on the site that Elon has screwed up, he is @precordialthump.
| INTENSIVE | RAGE | Resuscitology | SMACC