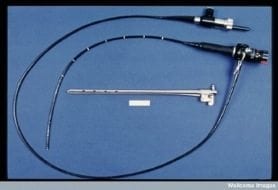
Flexible bronchoscope
OVERVIEW
- flexible bronchoscope may be fibre optic, video or hybrid systems
USES
Diagnosis
- diagnose diseases of the tracheobronchial tree (e.g. burns, tumours)
- obtain lung samples (e.g. airway biopsies, bronchial washings, bronchoalveolar lavage (BAL) specimens)
Therapies and procedures
- difficult intubation (e.g. awake fiberoptic intubation)
- suction of secretions or blood from the airways
- guide placement of a percutaneous tracheostomy, double-lumen tube, bronchial blockers and endobronchial valves
- treatment of specific disorders (e.g. control bleeding from focal lesions)
DESCRIPTION
- Flexible long, thin plastic tube enclosing a fibre optic system that attaches to a light source and transmits views from the distal tip to an eyepiece
- eyepiece can attach to a camera and/or video system that displays images on a screen
- flexible tip can be moved to negotiate passage of the tip into the airways using a lever controlled by the operators hand (Bowden cable system)
- suctioning channel connected to the tip and controlled on the proximal hand piece
- instrumentation port (for inserting instruments such as brushes or biopsy forceps or injecting saline)
- ergonomic design of the control section that fits the hand
- 120° field of view with 180° up and 130° down angulation
- Range of tip diameters (e.g. 2.8 mm to 5.9 mm for Olympus scopes), sizes of instrument channels and lengths (e.g. longer length with smaller diameter needed for double-lumen tubes)
- Accessories can be either disposable or autoclavable (e.g. suction connector; instrument channel cover)
METHOD OF INSERTION/ USE
- assemble bronchoscope (details are device dependent)
- patients’ airway is anesthetised (e.g. either deep sedation or topical local anaesthetic)
- adjust ventilator settings and alarms as required
- set high peak pressures
- administer FiO2 1.0
- use volume-controlled ventilation
- full monitoring
- suction airway
- insert a Y connector
- perform diagnostic and/or therapeutic bronchoscopy
(see videos below) - turning: combine flex/ extend with rotation
- lavage with saline with suction into a Lukens trap
COMPLICATIONS
- Trauma to the airways
- coughing and bronchospasm (if inadequate anaesthesia)
- loss of PEEP with derecruitment and oxygen desaturation
- barotrauma
- bronchoscope damage (e.g. biting; friction from inadequate lubrication especially if a tight fit down a tube; needle injury during a tracheostomy if not sufficiently pulled back while the procedure is being performed)
- infection (scope to patient and patient to operator especially if inadequate respiratory precautions adopted)
- accidental extubation
OTHER INFORMATION
- Cleaning and engineering maintenance is critical — inadequate sterilisation can lead to transmission of infective organisms
- Bowden cable system involves a flexible cable that converts a mechanical force by movement of an inner cable relative to the outer housing
References and Links
FOAM and web resources
- Bronchoscopy International Youtube Channel
- Bronchoscopy Simulator (ThoracicAnaesthesia.com)
- American Thoracic Society — Bronchoalveolar lavage
Lots of great videos on the Bronchoscopy International Youtube Channel

Critical Care
Compendium
Chris is an Intensivist and ECMO specialist at The Alfred ICU, where he is Deputy Director (Education). He is a Clinical Adjunct Associate Professor at Monash University, the Lead for the Clinician Educator Incubator programme, and a CICM First Part Examiner.
He is an internationally recognised Clinician Educator with a passion for helping clinicians learn and for improving the clinical performance of individuals and collectives. He was one of the founders of the FOAM movement (Free Open-Access Medical education) has been recognised for his contributions to education with awards from ANZICS, ANZAHPE, and ACEM.
His one great achievement is being the father of three amazing children.
On Bluesky, he is @precordialthump.bsky.social and on the site that Elon has screwed up, he is @precordialthump.
| INTENSIVE | RAGE | Resuscitology | SMACC

Nice, Chris. There are also some useful links, videos and info sections on OpenAirway.org, and the OpenAirway YouTube channel. Feel free to share!