Fluid administration device flow rates
Reviewed and revised 26 July 2015
OVERVIEW
- rapid fluid administration is potentially life-saving in the resuscitation setting
- flow rates achieved depend on the devices used in fluid administration, largely in agreement with Poiseuille’s law
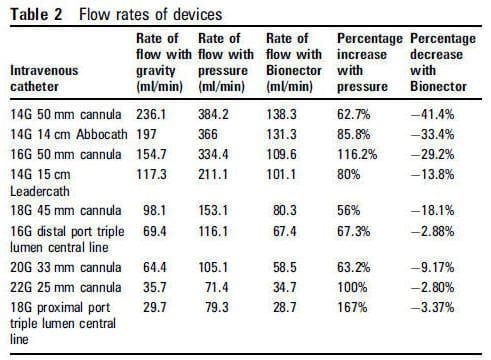
FLOW RATES
PRACTICAL TIPS
General rules of thumb
- a large bore cannula is preferable to a narrow bore cannula
- a shorter cannula is preferable to a longer cannula
- a larger proximal vein is preferable to smaller distal vein
- upper limbs are preferable to lower limbs, especially in CPR
Choice of vascular access
- a peripheral cannula of size 18G or greater is preferable to infusion by central line for rapid fluid delivery
- if a central line is the only obtainable access then the addition of a pressure bag makes a greater difference to rate of flow than it would with a peripheral cannula
- An over the needle FEP large-bore cannula inserted into a large vein is likely to give a greater flow rate than a Seldinger type polyurethane catheter and would be preferable if all other factors are equal
- A needle-free intravenous access connector (a “bung”) should not be used when rapid fluid resuscitation is required as it slows the rate offlow by up to 40% with peripheral cannulae
Intraosseous access
- Flow rates of 60–100 ml/min of crystalloid, via a 15 gauge tibial intraosseous needle, have been achieved in the adult using the hydraulic pressure of a large syringe, attached to the needle by a three way tap and fed from a standard infusion bag
- In a resuscitation setting, IO access is preferable to CVC insertion if peripheral vascular access cannot be obtained rapidly
— higher success rates on first attempt (85% versus 60%, p=0.024)
— shorter procedure times (2.0 versus 8.0 min, p<0.001)
References and Links
Journal articles
- Leidel BA, Kirchhoff C, Bogner V, Braunstein V, Biberthaler P, Kanz KG. Comparison of intraosseous versus central venous vascular access in adults under resuscitation in the emergency department with inaccessible peripheral veins. Resuscitation. 2012 Jan;83(1):40-5. PMID: 21893125.
- Reddick AD, Ronald J, Morrison WG. Intravenous fluid resuscitation: was Poiseuille right? Emerg Med J. 2011 Mar;28(3):201-2. PMID: 20581377.
- Waisman M, Waisman D. Bone marrow infusion in adults. J Trauma. 1997 Feb;42(2):288-93. PMID: 9042884.

Critical Care
Compendium
Chris is an Intensivist and ECMO specialist at The Alfred ICU, where he is Deputy Director (Education). He is a Clinical Adjunct Associate Professor at Monash University, the Lead for the Clinician Educator Incubator programme, and a CICM First Part Examiner.
He is an internationally recognised Clinician Educator with a passion for helping clinicians learn and for improving the clinical performance of individuals and collectives. He was one of the founders of the FOAM movement (Free Open-Access Medical education) has been recognised for his contributions to education with awards from ANZICS, ANZAHPE, and ACEM.
His one great achievement is being the father of three amazing children.
On Bluesky, he is @precordialthump.bsky.social and on the site that Elon has screwed up, he is @precordialthump.
| INTENSIVE | RAGE | Resuscitology | SMACC

Thanks for the awesome site. I do have to point out the following though….
It is not the case that ” flow rates are largely in agreement with Poiseuille’s law”
It’s clear from looking at the data that the relationship between radius and flow is roughly r^1.5, not r^4. That’s a huge difference.
A 22g piv has a higher flow rate than a 18g cvc, even though the internal radius of a 22g is about half of a 18g. Length trumps radius in that regard. Poiseuille’s law doesn’t apply to turbulent flow, which starts around 1-10m/s. These fluids are moving > 50m/s
We should stop teaching Poiseuille’s law. It doesn’t apply.
Thanks!
Dan