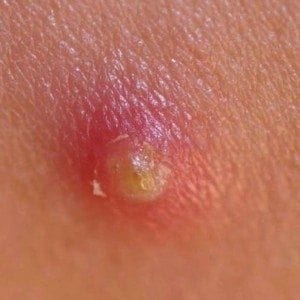
Furuncular myiasis
Beware the foreign traveler! Today we explore the evolving ‘furuncle’ or boil. A simple enough beast to deal with under normal circumstances – but in the returning traveler…myriad possibilities raise their ugly heads…
Overview
The common or garden furuncle is usually associated with infection (commonly staphylococcus aureus) at the base of a hair follicle where purulent material extends through the dermis into the subcutaneous tissue, and is evident by a small abscess.However, in the returning traveler furuncular myiasis caused by Dermatobia hominis must be on the differential diagnosis. Furuncular myiasis is endemic throughout Central and South America and produces boil-like lesions commonly misdiagnosed as a furuncle.
The furuncle has a central pore that intermittently exudes a serosanguinous discharge (the feces of the larva), and protrusion of the breathing tube of the larva frequently can be observed
The larvae are transmitted to vertebrate animals by hematophagous insects, most commonly mosquitoes, on whose abdomens the female botfly has deposited her eggs. When the blood-feeding vector encounters a warm-blooded animal, the change in temperature causes the botfly eggs to hatch. The larvae enter the vertebrate host either through a hair follicle, the bite site, or by directly burrowing in the skin. Over the next 4–18 weeks, the larva grows by eating the flesh of its host. At maturity it emerges from the wound, falls to the soil, and pupates.
Treatment
Although the botfly will, when mature, exit the site by itself, this is not usually acceptable to the patient…Botflies, when properly diagnosed, either are surgically removed or asphyxiated and then manually removed. Many methods for extracting the larvae have been described for the treatment of furuncular myiasis.
Bacon Therapy
I think using bacon fat is a good idea. It doesn’t take too long (about three hours), doesn’t leave dead larvae under the skin (as oil occlusion, lignocaine infiltration or larvacide treatment may), it’s non-invasive (avoids the need for incision and drainage) and is cheap. However, it may not be suitable for extreme cases of Tumbu larva infestation as the female fly lays 100-300 eggs in several batches – that would need a lot of bacon.
Procedure: The furuncles are left covered with bacon fat. This encourages the larvae to exit the skin, either due to suffocation or an attraction to bacon. After about 3 hours the bacon fat is carefully removed with forceps at the ready to help fully extricate the larvae.
What you do with the bacon and the larvae afterward is your business. And if you’ve got myiasis, try to look on the bright side, things could always be worse…
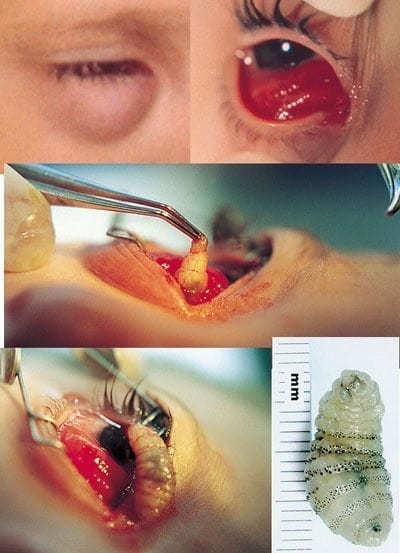
Asphyxiants
Duct Tape: Covering the location with adhesive tape results in partial asphyxiation and weakening of the larva, but is not recommended because the larva’s breathing tube is fragile and would be broken during the removal of the tape, leaving most of the larva behind.Petroleum jelly or vaseline can also be applied over the location, which prevents air from reaching the larva, suffocating it. It can then be squeezed out.
Nail Polish: A larva has been successfully removed by first applying several coats of nail polish to the area of the larva’s entrance, weakening it by partial asphyxiation.
Procedure: Apply nail polish to the central pore of the nodule. This leads to partial asphyxiation of the larva causing it to retract its spines and attempt to reposition its breathing tube to reach air. Although the larva may succeed in penetrating the first few applications of nail polish, eventually it is trapped and asphyxiated. This facilitates subsequent manual extraction of the entire larva provided that it is grasped well down its length. The breathing tube is fragile and breaks easily, contraindicating the use of duct tape which some use for larva removal
References:
- Bringing home the bacon
- Bhandari, Ramanath; David P. Janos and Photini Sinnis (March 2007). “Furuncular myiasis caused by Dermatobia hominis in a returning traveler“. The American journal of tropical medicine and hygiene 76 (3): 598–9.
- Boggild, Andrea K.; Jay S. Keystone and Kevin C. Kain (August 2002). “Furuncular myiasis: a simple and rapid method for extraction of intact Dermatobia hominis larvae“. Clinical Infectious Diseases 35 (3): 336–338.
BA MA (Oxon) MBChB (Edin) FACEM FFSEM. Emergency physician, Sir Charles Gairdner Hospital. Passion for rugby; medical history; medical education; and asynchronous learning #FOAMed evangelist. Co-founder and CTO of Life in the Fast lane | On Call: Principles and Protocol 4e| Eponyms | Books |