Roger Manley
Roger Edward Wentworth Manley (1930 – 1991) was a British inventor, anaesthetist and engineer
Manley was the pioneer of the Manley Ventilator. His prototype ventilator was assembled from various parts including the bellows of the then Blease ‘Pulmoflator’ in his garage. It was easy to use as it only required a fresh gas flow, and was later refined to become the well-known ‘minute volume divider’ Manley ventilator.
Manly became managing director of the Blease Company and later Cape Engineering. He founded his own engineering company was a consultant to others; adviser in medical engineering to Westminster Hospital; and an honorary clinical assistant in anaesthesia and intensive care at the Medical Research Council unit at Northwick Park.
He also developed the Manley Multivent (Penlon Manley), and was a major contributor to solving the problem of mechanical ventilation in the developing world.
Biography
- Born in 1930
- 1954 – Graduated in medicine and surgery from the Westminster Hospital Medical College, London
- 1959 – Senior House Officer, Department of Clinical Measurement Westminster Hospital. Manley attended a symposium on the treatment of ventilatory failure at the Royal college of Surgeons in London and within two days of the meeting, produced a prototype ventilator
- 1960 – The Manley ventilator was refined and marketed by John Blease (1906 – 1985) as the MP2
- 1961 – Published on his “new mechanical ventilator” in the journal Anaesthesia
- 1990 – Designs a new ventilator (later known as the Manley Multivent) for use in the developing world however dies prior to its production
- Died on December 11, 1991
Medical Eponyms
Manley ventilator (Blease Manley ventilator)
The Manley ventilator required no external power source, was connected to the fresh gas outlet of the anaesthetic machine and delivered the gas to the patient as a minute volume divider.
Inflation was achieved by adjusting a variable weight loaded bellows to deliver a pre-set volume; the weight on the bar above the bellows helped set the inspiratory pressure and a rotameter was used to set minute volume. Inspiratory pressures up to 30cmH2O could be achieved

Fig 1. The ventilator. Manley RW. Anaesthesia. 1961
During inspiration:
- Valve 1 (V1) is closed
- Fresh gas flows into the bellows (B1) and fills
- Valve (V2) is open, Valve 3 (V3) is closed
- Weight (W) on top of the bellows forces the gas into the patient’s lungs and inflation occurs
- Duration of inspiration depends on height of B1
- At end of inspiration V1 opens, pressure in chamber falls and V2 closes; V3 opens
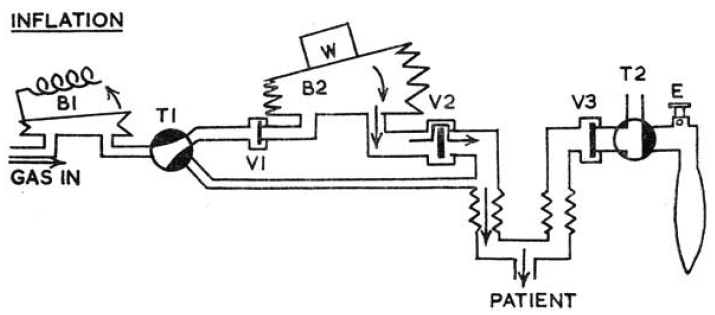
Manley RW. A new mechanical ventilator. Anaesthesia. 1961
During expiration:
- Patients’ lungs are open to the atmosphere
- Gas from B1 flows via V1 to B2
- Duration of expiration depends on height of B2 before lever system closes V1
- When V1 closes, pressure in chamber rises causing V3 to close and opening V2 and dthe cycle repeats
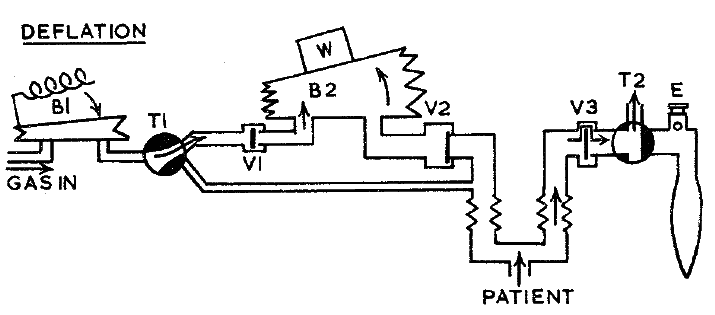
Manley RW. A new mechanical ventilator. Anaesthesia. 1961
There was no electronic alarm for low or high pressures rather the anaesthetist had to be attuned to the audible changes of a disconnected or obstructed circuit. In an obstructed circuit or where there was increased air resistance (coughing), the bellows could not deliver the full tidal volume and so “clunking” could be heard as the ventilator alternated between inspiratory and expiratory phases. In a disconnected circuit, there was no air ways resistance so a “thump” could be heard as the bellows fell onto the rubber stopper on the ventilator casing
Manley Multivent Ventilator (Penlon Manley Multivent)
A simple and extremely versatile ventilator, the Manley Multivent came into production after Manley’s death and has made major contribution to mechanical ventilation in the developing world.
It is an automatically powered version of the Oxford inflating bellows. There are only 3 controls – tidal volume, respiratory rate and I:E ratio which is pre-set to 1:2. Either oxygen or compressed air from a mains electricity or 12V DC car battery, can be used to drive the ventilator.
If oxygen is used, it has dual role in elevating the bellows as well as supplementing the inspired gas mixture to increase the fiO2. If ether is used as anaesthetic, then an alternate version of the Manley Multivent is available which includes an electronic gas circuit that is separated from the gas mixture by a distance of 25cm. This reduces the risk of an explosion.
Major Publications
- Manley RW. A new mechanical ventilator. Anaesthesia. 1961; 16: 317-323.
- Brooks DK, William WG, Manley RW, Whiteman P. Respiratory changes in haemorrhagic shock. The association of respiratory failure with gross changes in biochemistry and osmolarity. Anaesthesia. 1963; 18: 363-376
- Williams WG, Manley RW, Drew C. Pulmonary circulatory arrest. Thorax. 1965; 20(6): 523-527.
- Manley RW. Il respiratore Blease Automan [The Blease Automan respirator]. Minerva Anestesiol. 1967; 33(1): 29-32
References
Biography
- Forward RFM. Obituary, REW Manley. BMJ 1992; 304: 1050
- McKenzie AG. The inventions of John Blease. Br J Anaesth. 2000; 85(6): 928-935.
- Maltby JR. Manley ventilator. In: Notable Names in Anaesthesia. The Choir Press, 2013: 129-131
Eponymous terms
- Feldman S. The Manley Ventilator. Anaesthesia 1995; 50: 64.
- Eltringham RJ, Varvinski A. The Oxyvent. An anaesthetic machine designed to be used in developing countries and difficult situations. Anaesthesia. 1997; 52(7): 668-672
- Stanga DF, Beck G, Chniak JM. Evaluation of respiratory support devices for use in the hyperbaric chamber. Navy experimental diving unit. 2003
- Westhorpe RN, Ball C. The Manley ventilator. Anaesth Intensive Care. 2012; 40(5): 749-750.
[cite]

eponym
the person behind the name
FACEM. Emergency physician and researcher at Sir Charles Gairdner Hospital, Perth
BA MA (Oxon) MBChB (Edin) FACEM FFSEM. Emergency physician, Sir Charles Gairdner Hospital. Passion for rugby; medical history; medical education; and asynchronous learning #FOAMed evangelist. Co-founder and CTO of Life in the Fast lane | On Call: Principles and Protocol 4e| Eponyms | Books |



