Rudolph Matas

Rudolph Matas (1860-1957) was an American vascular surgeon
Matas led a long medical career with many distinctions; oft referred to as he ‘Father of vascular surgery’.
Matas was a strong advocate for laparotomy for acute appendicitis; the first to confirm its intraperitoneal nature; and the first to attempt to use the intravenous drip to administer fluids in the treatment for acute hypovolemia and other disorders. He was propelled to fame following his novel technique for repair of brachial aneurysm in 1888 by endoaneurysmorrhaphy and went on to perform 622 aneurysmal repairs over his career.
Outside of surgery, Matas was the first to demonstrate successful spinal anaesthesia via a lumbar approach in the US. He experimented and detailed the effective application of regional anaesthesia and campaigned for its use over general anaesthesia in surgery. Indeed, while he was Chair of Surgery at Charity Hospital, only 30% of surgeries were performed under general anaesthesia compared to all surgical cases prior to his appointment, and the rest were all done under either spinal or regional anaesthesia.
Matas was a pioneer in addressing the ‘pneumothorax’ problem in thoracic surgery. He collaborated with Dr Smythe and modified the Fell-O’Dwyer apparatus for artificial respiration for safe use in thoracic surgery.
Over the span of his career, which went well into his nineties, Matas authored over 600 articles and was involved in the education of generations of physicians. A gentleman who is remembered for his encyclopaedic memory, innovative mind and penchant for hard work, Matas was a prominent figure and pioneer to the fields of both surgery and anaesthesia.
Biography
- Born on September 12, 1860 at Bonnet Carre, 30miles from New Orleans
- 1877 – enrols in the medical department at the University of Louisiana (now known as Tulane University). Whilst a student, appointed as interpreter of the Yellow Fever Commission of the National Board of Health and went with the Committee to Cuba. Matas meets Dr Carlos Finlay who is the first physician to suggest mosquitos as a vector for Yellow Fever. Matas becomes one of the few physicians to champion the mosquito theory.
- 1880 – graduates MD aged 19 and works as resident at Charity Hospital in New Orleans; assisted at the first laparotomy performed under Listerian ritual, including the use of carbolic acid spray.
- 1882 – editor of the New Orleans Medical and Surgical Journal
- 1885-1887 publishes papers which identify the appendix and caecum as intraperitoneal structures – and to rectify historical error; appointed Demonstrator of Anatomy at Tulane University.
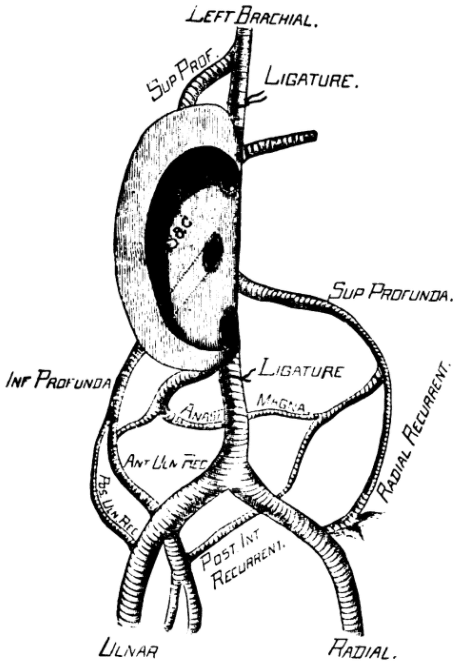
- 1888 – treats a patient with a leaking brachial artery aneurysm using an intrasaccular technique. Current practice at the time was to ligate both the distal and proximal portions of the inlet and outlet vessels – ‘Hunterian’ ligation – and was associated with high rates of gangrene, amputation and death.
- Matas’ technique is hailed as the ‘greatest advance in vascular surgery in 200 years’. Publishes case report titled “Traumatic aneurysm of the left brachial artery” in 1888 and the Annals of Surgery in 1903. In regards to the technique Matas writes: This procedure served me so satisfactorily, that I cannot but heartily recommend it to those who may be placed in similar circumstances
- 1894 – Professor and chairman of the Department of Surgery at Tulane University and holds this position until 1927
- 1899 – performs for the first time in the United States, spinal anaesthesia by injecting subarachnoid eucaine (synthetic cocaine substitute) for a patient undergoing haemorrhoid surgery via a lumbar approach. This is atypical to the norm where his colleagues were performing spinal anaesthetics at the sixth cervical space
[Drs Tait and Dr Caglieri] believe that the spinal cord like the brain is tolerant of trauma and do not fear the possibility of injuring it permanently with a fine needle while introducing the cocaine solution. Notwithstanding their confidence and the repeated successes, they have obtained, I cannot consider it a safe route to the spinal canal, and cannot recommend it in the regular practice of spinal anaesthesia
Matas, 1900
- Becomes a strong advocate for spinal anaesthesia at the lumbar level as well as regional anaesthesia in lieu of general anaesthesia for surgical cases.
- Develops a hand pump for the delivery of large volumes of weak anaesthetic solutions for use in surgeries requiring only local anaesthesia. The hand pump avoids the use of multiple syringes and skin punctures
- 1902 – collaborates with Dr John Smythe to modify the Fell-O’Dwyer apparatus for artificial respiration to allow for safe thoracic surgery and provides the solution to the ‘pneumothorax problem’
Until the danger of seriously interfering with the respiratory functions by inducing acute collapse of the lung is clearly eliminated or is reduced to a safe minimum, the analogy between the pleura and the peritoneum from the surgical point of view will never exist
Matas, 1900
- 1912 – on October 20, performed the first Kondoléon operation (to relieve chronic lymphoedema and for elephantiasis) that was done on the Western Hemisphere. The original communication by Kondoléon was in the Zentralblatt für Chirurgie on July 27, 1912
- 1913 – one of the 12 founders of the American College of Surgeons and president in 1925-26
- 1917 – founds the American Association for Thoracic Surgery and becomes third president in 1919
- 1923 – performed the first aortic ligation. Matas reported to the American Surgical Association (1925, 1940) on a case of ligation of the abdominal aorta for an aneurysm involving both common iliac arteries including bifurcation of the aorta
- Matas has emphasized the systemic effects of arteriovenous aneurysm; called attention to the desirability of delaying repair in order to favor the development of collaterals. He popularized Branham sign and eponymised Harris Miller Branham (1862-1936). Bradycardia that follows the sudden occlusion of an artery entering an arteriovenous fistula, which Matas believed held not only diagnostic but prognostic value in arteriovenous aneurysm
- 1924 – Matas was one of the first to advocate gastric drainage, emphasising the value of the use of the nasogatric Jutte tube. He stated:
By draining the stomach, the gastric tube acts in reality as an artificial anus which empties the upper intestine of its toxic contents and diminishes the abdominal distention caused by pent up gases, thereby adding enormously to the comfort of the patient.
Matas 1924
- Died on September 23, 1957 in New Orleans
Medical Eponyms
Rudolph Matas Award
This award recognizes a lifetime of excellence, achievement and contributions to the field of Vascular Surgery, and service to the Southern Association for Vascular Surgery. List of recipients.
Gentleness, compassion, tenderness do not exclude firmness. Persuasiveness and authority may travel hand in hand. Neither are resoluteness and an inflexible will incompatible with an inexhaustible patience and genuine sympathy
Matas: The Soul of the Surgeon, 1915
Key Medical Contributions
Matas intravenous drip
Matas is the first to use intravenous saline to treat acute hypotension secondary to blood loss in a patient post above knee amputation for leg sarcoma.
It is, I believe, historically correct to state that no attempt prior to July, 1888, had been made to infuse intravenously saline solution for the relief of acute anemia
Matas 1891
Delivery of fluids at that time (in a patient not taking oral fluid) was either via the rectum (protoclysis) or subcutaneously (hypodermoclysis). Following intravenous saline, Matas remarks of the patient:
Now, as the water flowed into the vein, he felt as if a delightful cool wave were gently spreading over his body and was giving him new strength and life and wonderfully appeasing his thirst. The pulse in the meantime improved immensely, it became fuller, more resistant to the finger, then slower, and finally quite strong and regular, the pulsation having been reduced from 150 to 100 and less when the injection was stopped.
Matas 1891
Although the patient dies later, Matas continues to experiment with intravenous saline and develops a hanging bottle and clamp method for fluid administration
Matas published ‘The continued intravenous “drip”.’ in the Annals of Surgery in 1924
“the purpose…of this communication is to direct attention to the value and advantages of the intravenous route for the direct and continuous instillation of fluids intended to replace the volume of lost blood….as may be required to restore the vascular equilibrium and rally the patient until the defensive cardiovascular mechanism has had time to assert itself…
Matas 1924
He highlights the pitfalls of current routes for fluid administration:
…the rectal drip…is of little or no service; it is frequently not absorbed especially when the portal circulation is stagnant…it is frequently not retained or tolerated and therefore fails when it is most needed
hypodermoclysis…also fails when the capillary circulation is at a standstill or failing from shock after the operation…very little fluid is absorbed and remains in great oedematous collections under the skin.
Matas 1924
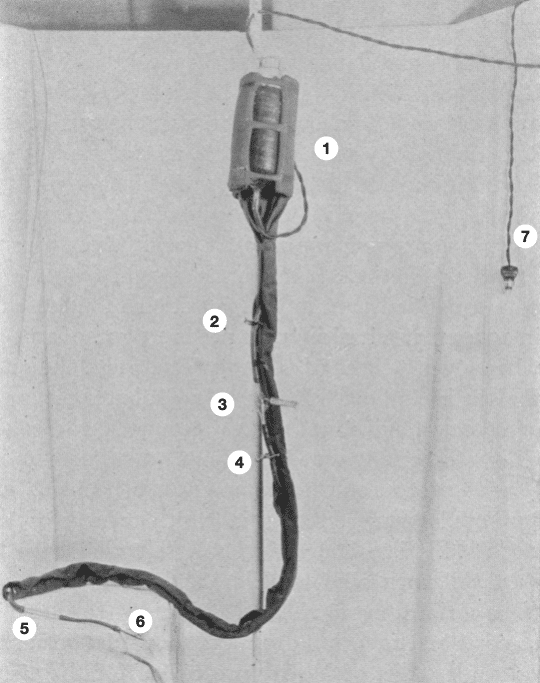
Fig 2. 1. Glass (Kelly) bottle containing glucose or saline solution with Duchesne Electric Heating Pad 2. Screw compressor to regulate the flow of the solution in the tubing 3. Murphy drip bulb showing a hypodermic needle inserted in the vent when the solution is to be medicated with stimulating or cardio-tonic drugs. The bulb is exposed to view so that the drop rate may be always under inspection. 4. Second screw compressor to control the flow in the bulb and maintain a constant visible level of the solution in the bulb, thereby excluding air from the drip. 5. Glass joint connecting the terminal tubing and cannula and exposed to view to detect any reflux of blood from the vein. 6. Cannula 7. Plug and cable attached to the Duchesne pad
Matas “Continued Intravenous Drip.” 1924
Controversies
The ‘secret’ operation of Matas famously circulated around New Orleans for many years. It was performed by friend Dr William Halsted for a ‘mass’ in 1903. It was never divulged during the life time of either man. Only upon autopsy following Matas’ death, was it noted that he had undergone a right orchidectomy.
Matas’ publication titled ‘Surgical peculiarities of the American Negro’ saw him become a ‘expert’ in the pathologies unique to ‘Blacks.’ He had a special interest in skin conditions afflicting African Americans and collected many photographs of disfiguring tumours and untreated infections. He noted an increased ‘predisposition’ of keloids and hyperplasia ‘at the least provocation;’ a problem he felt to be a ‘racial peculiarity’ to ‘Blacks.’ He observed a spectrum of pathologies and cited numerous other observations through his collection of cases at Charity Hospital tabulated on the basis of race: ‘white’ ‘coloured’ and ‘mulatto.’ Whilst hailed as an expert at that time, from today’s perspective, Matas work and conclusions on racial pathologies would imply underlying constitutional racism.
Matas personal life was plagued with tragedies. His parents were never happy together and separated. His mother and sister were never supportive and he became estranged from them later in life. Whilst happily married to his wife Adrienne, their only child was still born. When he was 48 years old, he lost his right eye to gonococcal conjunctivitis that he contracted during an operation on a patient with a tubo-ovarian abscess. It was said he was very self-conscious and would refuse to appear in public until an artificial eye was made for him. His wife died in 1918 from pneumonia, another emotional blow to Matas. In his old age, he became progressively forgetful and blind and eventually wheel chair bound from 1954 onwards. During his last 18mths of life, he was fed through a stomach tube.
Matas was exceptionally tardy and never met deadlines. He would talk for longer than required and when writing articles, deliver content in excess to what was preferred by his publishers. In fact, his work on a chapter in Keen’s Compendium of Surgery was submitted three years late and four times longer than expected!
Major Publications
- Matas R. Iliac phlegmons : some considerations of anatomical and surgical interest. Transactions of the Louisiana State Medical Society, April, 1886
- Matas R. The peritoneal relations of the caecum: rectification of an historical error. New Orleans medical and surgical journal, December 1887
- Matas R. Traumatic aneurysm of the left brachial artery. The Medical News, 1888; 53: 462-466
- Matas R. A Clinical Report on Intravenous Saline Infusion in the Wards of the New Orleans Charity Hospital from June, 1888 to June, 1891. New Orleans medical and surgical journal, 1891; 19(1): 1-31. and 19(2): 81-93
- Matas R. Surgical peculiarities of the American Negro. Transactions of the Meeting of the American Surgical Association. 1896; 14: 483-610
- Matas R. The surgery of the chest and some of the problems related to the treatment of its penetrating traumatisms and their immediate complications. Transactions of the Louisiana State Medical Society. 1898; 19: 125-173
- Matas R. The history fo the methods of Intralaryngeal Insufflation for the Relief of Acute Surgical Pneumothorax, with a description of the Latest devices for the Purpose. Transactions of the Southern Surgical and Gynecological Association. 1899; 12: 52-84
- Matas R. On the Management of Acute Traumatic Pneumothorax. Annals of Surgery, 1899; 29(4): 409–434
- Matas R. Intralaryngeal insufflation: for the relief of acute surgical pneumothorax. Its history and methods with a description of the latest devices for this purpose. JAMA. 1900; XXXIV(22): 1371-1375 and JAMA. 1900; XXXIV(23):1468-1473
- Matas R. Local and regional anesthesia with cocain and other analgesic drugs, including the subarachnoid method, as applied in general surgical practice. The Philadelphia Medical Journal, 1900; VI(18): 820–843
- Matas R. Artificial Respiration by Direct Intralaryngeal Intubation with a Modified O’Dwyer Tube and a New Graduated Air-pump in its Applications to Medical and Surgical Practice. Transactions of the Meeting of the American Surgical Association. 1901; 14: 483-610
- Matas R. An operation for the radical cure of aneurism based upon arteriorrhaphy. Annals of Surgery, 1903; 37(2): 161-196.
- Matas R. The soul of the surgeon. Transactions of the Mississippi State Medical Association 1915; 48: 149-175.
- Matas R. Endo-Aneurysmorrhaphy: I. Statistics of the Operation; II. Personal Experiences and Observations on the Treatment of Arteriovenous Aneurisms by the Intrasaccular Method of Suture, Transactions of the Southern Surgical Association 1919; 32: 447-450 and 451-486
- Matas R. Branham’s Bradycardiac reaction. In: On the Systemic or Cardiovascular Effects of Arteriovenous Fistulae: A General Discussion Based upon the Author’s Surgical Experience, Transactions of the Southern Surgical Association 1923; 36: 623-682 [Branham sign]
- Matas R. The continued intravenous “drip.” Annals of Surgery 1924: 79(5): 643-661
- Matas R. William Stewart Halsted 1852-1922: an appreciation. Johns Hopkins Hospital Bulletin 1925; 36: 2-27
- Matas R. Primary Thrombosis of the Axillary Vein Caused by Strain, Am. J. Surg. 1934; 24(3): 642-666
- Matas R. Local and regional anesthesia: A retrospect and prospect. Am J Surg. 1934; 25(1): 189-196 and 1934; 25(2): 362-379.
- Matas R. Personal Experiences in Vascular Surgery, Ann. Surg. 1940; 112(5): 802-839.
- asdasdas
- asdasdas

in New Orleans), 1953
References
Biography
- Ochsner A. Dr. Rudolph Matas. AMA Arch Surg. 1956 Jan;72(1):1-19.
- Cohn I. Rudolph Matas a biography of one of the great pioneers in surgery. Doubleday, 1960
- Cordell AR. A lasting legacy: the life and work of Rudolph Matas. J Vasc Surg. 1985 Jul;2(4):613-9
- Nunn DB. Dr. Halsted’s secret operation on Dr. Matas. Ann Surg. 1992 Jul;216(1):87-93
- Ochsner J. The complex life of Rudolph Matas. J Vasc Surg. 2001 Sep;34(3):387-392.
- Hutson LR Jr, Vachon CA. Dr. Rudolph Matas: innovator and pioneer in anesthesiology. Anesthesiology. 2005 Oct;103(4):885-9
- Kenny SC. Capturing Racial Pathology: American Medical Photography in the Era of Jim Crow. Am J Public Health. 2020 Jan;110(1):75-83
- Nakayama DK. Surgical Peculiarities of the American Negro by Rudolph Matas (1896). Am Surg. 2021 Jan;87(1):5-7.
- Biography: Matas, Rudolph (1860 – 1957). Plarr’s Lives of the Fellows Online. Royal College of Surgeons of England.
- Bibliography. Matas, Rudolph 1860-1957. WorldCat Identities
Eponymous terms
- Trubuhovich RV. 19th century pioneering of intensive therapy in North America. Part 3: the Fell-O’Dwyer apparatus and William P Northrup. Crit Care Resusc. 2009 Mar;11(1):78-86
- Ardon AE. Positive-pressure ventilation, spinal anesthesia, and Rudolph Matas: the anesthetic contributions of an inquisitive surgical legend. J La State Med Soc. 2010 Jan-Feb;162(1):36-9.
- Trotter MC. Rudolph Matas and the first endoaneurysmorrhaphy: “a fine account of this operation”. J Vasc Surg. 2010 Jun;51(6):1569-71.
Eponym
the person behind the name
FACEM. Emergency physician and researcher at Sir Charles Gairdner Hospital, Perth
BA MA (Oxon) MBChB (Edin) FACEM FFSEM. Emergency physician, Sir Charles Gairdner Hospital. Passion for rugby; medical history; medical education; and asynchronous learning #FOAMed evangelist. Co-founder and CTO of Life in the Fast lane | On Call: Principles and Protocol 4e| Eponyms | Books |

