Spirometry
OVERVIEW
- Capacity = any combination of 2 or more volumes
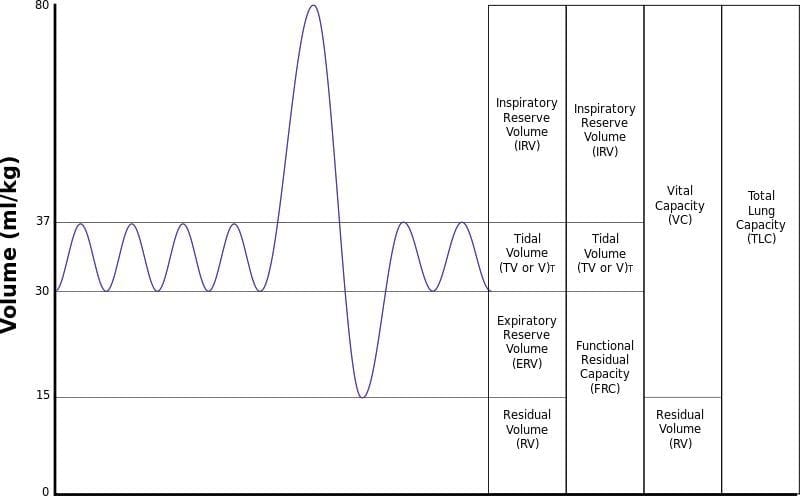
LUNG VOLUMES
FLOW VOLUME LOOP
PARAMETERS
- VC = 70mL/kg
= IRV + TV + ERV - IRV = 45mL/kg
- TV = 10mL/kg – volume breathed in & out during a normal breath (without extra effort)
- ERV = 15mL/kg – extra volume beyond normal expiration
- RV = 15mL\kg (not measured by spirometer)
- TLC = 85L\kg
- FRC = 30mL\kg
- FEV1 = forced expiratory volume in 1 second (normally 4L)
- FVC = forced vital capacity (a little lower than VC because of dynamic airway closure; normally ~5L)
- PEFR = peak flow rate over an expiration (normally 500L/min)
- FEV1/FVC (normal = 80%)
– obstructive disease = FEV1 reduced more than FVC, low FEV1/FVC
– restrictive disease = FEV1 & FVC reduced but FEV1/FVC normal or increased
– after a relatively small amount of gas has been exhaled -> flow is limited by airway compression determined by (1) elastic recoil force of lung & (2) resistance of airways upstream of the collapse point. - FEF50%
- FIF50%
- FEF/FIF50 = if > 1 -> inspiratory flow is affected more than expiratory -> extrathoracic site of obstruction
OBSTRUCTIVE DISEASE
- flow rate very low in relation to lung volume (c/o resistance to flow – scooped out appearance often seen following the point of maximum flow)
- total lung capacity is large, but expiration ends prematurely c/o early airway closure from increased smooth muscle tone of bronchi (asthma) or loss of radial traction from surrounding parenchyma (emphysema).
- equal pressure point is close to the alveolus and the transmural pressure gradient can become negative quickly -> collapse.
- encroachment of VC by an increased RV caused by hyperinflation (‘air trapping’)
RESTRICTIVE DISEASE
- total volume exhaled and flow rate reduced
- inspiration limited by reduced compliance of lung/chest wall or weakness of inspiratory muscles

Critical Care
Compendium
Chris is an Intensivist and ECMO specialist at The Alfred ICU, where he is Deputy Director (Education). He is a Clinical Adjunct Associate Professor at Monash University, the Lead for the Clinician Educator Incubator programme, and a CICM First Part Examiner.
He is an internationally recognised Clinician Educator with a passion for helping clinicians learn and for improving the clinical performance of individuals and collectives. He was one of the founders of the FOAM movement (Free Open-Access Medical education) has been recognised for his contributions to education with awards from ANZICS, ANZAHPE, and ACEM.
His one great achievement is being the father of three amazing children.
On Bluesky, he is @precordialthump.bsky.social and on the site that Elon has screwed up, he is @precordialthump.
| INTENSIVE | RAGE | Resuscitology | SMACC