Ultrasound Case 086
Presentation
A 75 year old man with a history of fibrosing alveolitis, on home oxygen presented with chest and neck pain, a strange and altered voice and itchy sensation in his throat, and swelling of his neck. It had gradually worsened over 10 days prior to presentation. He feels slightly short of breath and has noticed a crackling sensation when he pressed his skin over his upper chest and neck.
He describes blowing his nose ‘vigorously’ under water each morning in an attempt to clear his nostrils of dried secretions (secondary to the the intranasal oxygen) and associated ear and neck pain whilst performing these Valsalva manoeuvres.
You are sure he has subcutaneous emphysema and wonder if he has a pneumothorax associated with this. Can ultrasound help? Have a listen…then have a look.
AUDIO
ULTRASOUND
Initial probe view: Longitudinal view, second or third interspace mid clavicular line
View 2 …a little gentle probe pressure
View 3 …longer firmer probe pressure
Describe and interpret these scans
IMAGE INTERPRETATION
Audio 1: Voice changes of the patient
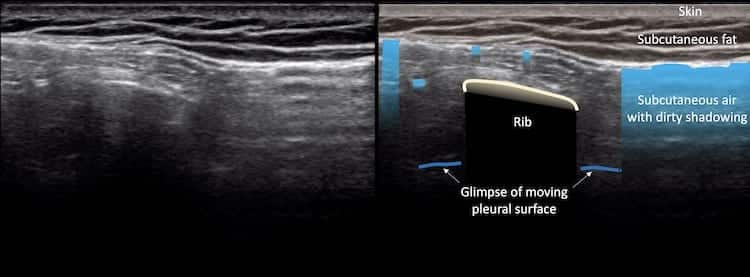
Image 1: Longitudinal view, second interspace mid clavicular line.
The skin and subcutaneous fat is well seen, but a layer of air lies over the muscles of the chest wall, completely obscuring the ribs, the pectoral and intercostal muscles and the pleural surface. The air interface is relatively static and should not be confused with pneumothorax.
Image 2: Same probe position, some gentle probe pressure moves some of the air out to the sides and a glimpse of underlying rib and moving pleura is seen.
Image 3: Same probe position, more gentle firm pressure and the view of the pleural surface improves more. The movement at the pleural interface means at that point anyway there is no pneumothorax.
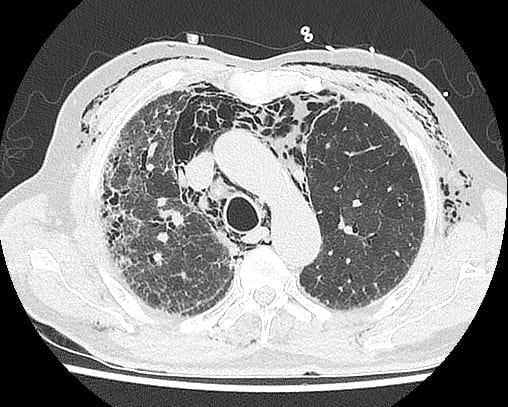
Image 4: CT demonstrating subcutaneous emphysema, extensive pneumomediastinum, but no pneumothorax. There is underlying pulmonary fibrosis.
CLINICAL CORRELATION
Subcutaneous emphysema following Valsalva manoeuvre
Subcutaneous emphysema obscures visualisation of deeper tissues. In this case the ribs and pleural line are obscured and it is impossible to determine whether or not there is an underlying pneumothorax. Persistent firm but gentle pressure slowly pushes any subcutaneous air out of the way and allows the pleural line to be examined – and in this case exclude the presence of pneumothorax.
[cite]
TOP 100 ULTRASOUND CASES
An Emergency physician based in Perth, Western Australia. Professionally my passion lies in integrating advanced diagnostic and procedural ultrasound into clinical assessment and management of the undifferentiated patient. Sharing hard fought knowledge with innovative educational techniques to ensure knowledge translation and dissemination is my goal. Family, wild coastlines, native forests, and tinkering in the shed fills the rest of my contented time. | SonoCPD | Ultrasound library | Top 100 | @thesonocave |