CICM SAQ 2010.1 Q6
Question
6. A 20 year old primi-gravida presents at 37 weeks gestation with jaundice, headache, blurred vision and hypertension (140/90mmHg). The antenatal period was otherwise unremarkable. She is febrile, drowsy, pale, icteric and has pedal oedema. The uterus is palpated as for a full term pregnancy with a normal CTG trace. Examination is otherwise normal.
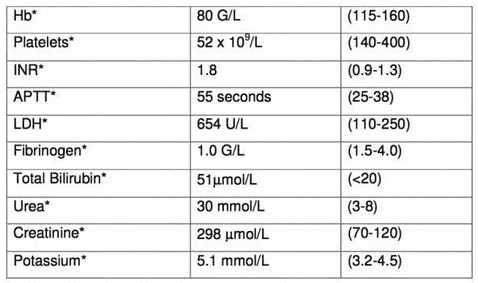
The following are her early blood results:
- (a) List 4 likely differential diagnoses for this clinical presentation.
- (b) What other investigations would you order for this patient and why?
- (c) List the important management interventions for each of your differential diagnoses.
Answers
Answer and interpretation
(a) List 4 likely differential diagnoses for this clinical presentation.
- Pre-eclampsia
- HELLP Syndrome
- Sepsis with DIC
- HUS-TTP
- Acute fatty liver of pregnancy
(b) What other investigations would you order for this patient and why?
- Transaminases (full liver function tests)
— Assessment of HELLP - Peripheral blood film smear
— Evidence of haemolysis or MAHA - Reticulocyte count, haptoglobins, conjugated/unconjugated bilirubin
— Haemolysis screen - Blood, sputum, urine and vaginal swab for MC&S
— Septic screen - Urinalysis – protein, WBCs, RBCs, casts
— Evidence of infection or proteinuria (pre-eclampsia) - Renal tract ultrasound
— Rule out obstruction
(c) List the important management interventions for each of your differential diagnoses.
Pre-eclampsia
- Deliver baby
- Control BP
- Hydralazine, beta blockers
- SNP/GTN if intravenous agent required.
- Prevention of seizures
- Magnesium sulphate
HELLP Syndrome
- Deliver baby
- Regular monitoring of platelet count and liver function
- Supportive measures whilst observing in HDU for dangerous complications – hepatic haemorrhage/rupture, progressive renal failure, pulmonary oedema.
- Sepsis with DIC
- Timely delivery of baby in consultation with obstetrician.
- Early broad spectrum antibiotics.
- Cardiovascular support – adequate volume resuscitation and establish a MAP > 65mmHg.
HUS-TTP
- Deliver the baby
- Fresh frozen plasma
- Therapeutic plasma exchange
- Corticosteroid therapy
- Monoclonal antibody therapy – Rituximab
Acute fatty liver of pregnancy
- Timely delivery of baby once mother stabilised
- Correction of DIC
- Supportive therapy
- Monitoring and treatment of complications post delivery eg pancreatitis
- Consideration for liver transplantation in irreversible severe liver failure despite delivery and aggressive supportive care

Examination Library
CICM
Chris is an Intensivist and ECMO specialist at The Alfred ICU, where he is Deputy Director (Education). He is a Clinical Adjunct Associate Professor at Monash University, the Lead for the Clinician Educator Incubator programme, and a CICM First Part Examiner.
He is an internationally recognised Clinician Educator with a passion for helping clinicians learn and for improving the clinical performance of individuals and collectives. He was one of the founders of the FOAM movement (Free Open-Access Medical education) has been recognised for his contributions to education with awards from ANZICS, ANZAHPE, and ACEM.
His one great achievement is being the father of three amazing children.
On Bluesky, he is @precordialthump.bsky.social and on the site that Elon has screwed up, he is @precordialthump.
| INTENSIVE | RAGE | Resuscitology | SMACC