CICM SAQ 2012.2 Q3
Q1. A 49-year-old female, with a history of pulmonary vasculitis is found collapsed in the ward with shallow breathing and a GCS of 6.
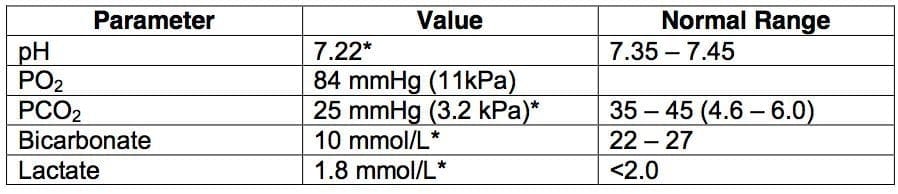
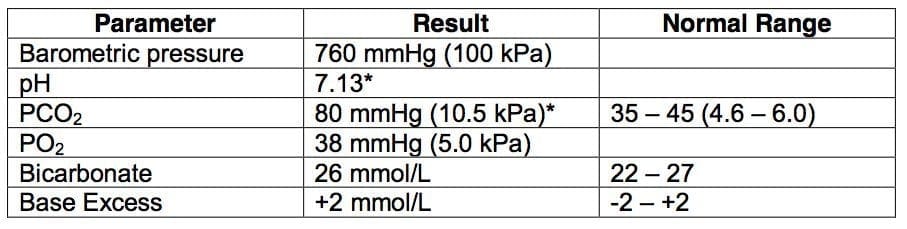
An initial arterial blood gas on room air (FiO2 0.21) reveals:
- What is the cause of the hypoxia? Give the reason for your answer
Q2. A 64-year-old man with a background of heavy alcohol consumption has been admitted to your ICU for several days with a sensitive staphylococcus aureus (MSSA) epidural abscess which has been surgically drained.
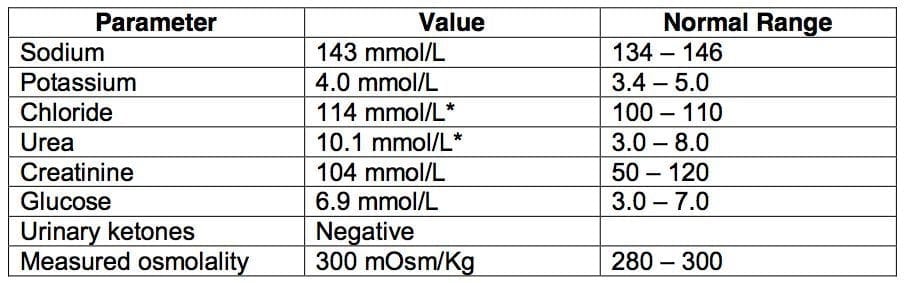
The following results were obtained:
On 30% oxygen arterial blood gas analysis as follows:
- What is the likely cause of the acid base disturbance?
- How would you investigate and manage it?
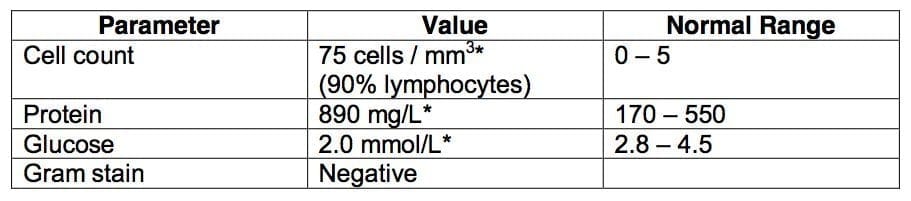
Q3. The following is a CSF sample from a 56-year-old woman with severe rheumatoid arthritis who has presented with fever, malaise and altered mental state.
Describe 4 further tests you would perform upon the CSF to establish an infective cause.
Answers
Answer and interpretation
Q1. What is the cause of the hypoxia? Give the reason for your answer
- Hypoventilation.
- No reason to believe there is parenchymal disease / vasculitis as the A-a gradient is 13 mmHg.
- This fits with the clinical picture of coma, shallow breathing and hypercapnia
Q2. What is the likely cause of the acid base disturbance? How would you investigate and manage it?
- High anion gap metabolic acidosis secondary to pyroglutamic acidaemia.
- Can be detected by requesting an organic acid screen, or by plasma or urine pyroglutamate levels.
- Management – cessation of precipitating drugs likely paracetamol and flucloxacillin in this case.
- N-Acetyl cysteine infusion has been advocated.
Q3. Describe 4 further tests you would perform upon the CSF to establish an infective cause.
- Herpes Simplex PCR
- Mycobacterium Tuberculosis PCR
- Mycobacterial Stain and Cultures
- India Ink Stain
- Cryptococcal Ag
- Fungal cultures
- Bacterial PCR
- Pass rate: 60%
- Highest mark: 9.3

Examination Library
CICM
Chris is an Intensivist and ECMO specialist at The Alfred ICU, where he is Deputy Director (Education). He is a Clinical Adjunct Associate Professor at Monash University, the Lead for the Clinician Educator Incubator programme, and a CICM First Part Examiner.
He is an internationally recognised Clinician Educator with a passion for helping clinicians learn and for improving the clinical performance of individuals and collectives. He was one of the founders of the FOAM movement (Free Open-Access Medical education) has been recognised for his contributions to education with awards from ANZICS, ANZAHPE, and ACEM.
His one great achievement is being the father of three amazing children.
On Bluesky, he is @precordialthump.bsky.social and on the site that Elon has screwed up, he is @precordialthump.
| INTENSIVE | RAGE | Resuscitology | SMACC