Compartment Syndrome CCC
Background
Musculoskeletal compartment syndrome is a limb threatening condition resulting from increased pressure within a muscular compartment, which causes compression of the nerves, muscles and vessels within the compartment.
Causes
Compartment syndrome is usually caused by fractures (about 75% of cases):
- especially tibia, humeral shaft, combined radius and ulna fractures, and supracondylar fractures in children
- may be open or closed
Compartment syndrome can also occur after a soft tissue injuries due to:
- crush injury
- snake bite
- excessive exertion
- prolonged immobilisation
- constrictive dressings and plaster casts
- soft tissue infection
- seizures
- extravasation of intravenous fluids and medications
- burns
- tourniquets
Patients with a coagulopathy are at particular risk of compartment syndrome.
Pathophysiology
Muscles are contained within inelastic fascial sheaths. When injured muscles swell, a hematoma forms, or external compression is applied, the pressure within the fascial compartment increases. If the pressure rises high enough, capillary pressure is exceeded and circulation is compromised. This results in ischemic injury to the muscles and nerves within the fascial compartment.
Normal tissue pressure ranges between zero and 10 mmHg. Capillary blood flow within the compartment may be compromised at pressures > 20 mmHg. Muscle and nerve fibers are at risk for ischemic necrosis at pressures >30 to 40mmHg. These pressures may still be tolerated — depending on the perfusion pressure, hence a recent trend towards using delta pressures, although most treatment recommendations are still based on absolute pressures:
- Delta pressure = diastolic blood pressure (DBP) — intracompartment pressure
- A delta pressure <30 mmHg is suggestive of compartment syndrome
Ischemic injury to muscles and nerves occurs after 4 hours of complete ischemia. This becomes irreversible at some point over the next 4 hours (i.e. 4-8 hours after the onset of ischemia), resulting in local rhabdomyolysis and neuropraxis progresses to axonotmesis as nerve injury worsens.
Compartment syndrome can affect many regions of the body:
- the forearm (volar compartment) and leg (the anterior compartment — the anatomical leg being the bit below the knee…) are most commonly affected.
- compartment syndrome can occur in other regions, including the back, buttocks, thigh, abdomen and foot
- compartment syndrome of the deep posterior compartment of the leg is easily missed
Complications include:
- gangrene or loss of limb viability requiring amputation
- ischemic contracture and loss of function
- rhabdomyolysis and renal failure
Assessment
History
- suspect if:
- one of the fractures listed above is present
- one of the soft tissue injuries listed above is present (e.g. crush injury)
- patient has a coexistent bleeding dosorder or coagulopathy
- Remember the 6Ps
1. pain (especially on passive stretching)
2. pallor
3. perishingly cold
4. pulselessness
5. paralysis
6. paraesthesiae
- Pain is the key symptom. It occurs early, is persistent, tends to be disproportionate compared with the original injury and is not relieved by immobilisation.
Examination
- Pain is exacerbated by passive stretching, which is the most sensitive sign.
- The extremity may be swollen and affected compartments may feel tense and tender on palpation.
- Assess loss of sensation by light touch and two-point discrimination, rather than just pinprick, which is less sensitive.
- Refer to a surgeon if compartment syndrome is suspected — do not rely on clinical signs — have a high index of suspicion!
Palpable distal pulses and normal capillary refill does not exclude compartment syndrome. Pulse oximetry is insensitive and is not recommended in the detection of compartment syndrome.
Compartment pressure measurement
- Measurement of elevated compartment pressures are not essential for the diagnosis if the clinical picture is compelling.
- At least with tibial fractures, measurements should be taken in both the anterior and deep posterior compartments at the level of the fracture as well as at proximal and distal locations to reliably determine the highest tissue pressure measurement. This measurement should be used to determine the need for fasciotomy.
- A commercial device like the Stryker STIC Device is probably the easiest and most accurate means of measuring compartment pressures.
- Compartment pressures may also be obtained using an angiocath connected to a blood pressure transducer (e.g. arterial line set up).
- Other options for measuring compartment pressures include the needle technique, the wick catheter, and the slit catheter.
- The needle technique according to Perron et al (2006) is described as follows:
The needle technique has the advantage that it can be performed with items that are readily available in every ED. An 18-gauge needle is attached to an intravenous extension tube and then to a stopcock. Approximately half the tubing is filled with sterile saline — being certain that air is not allowed into the tubing. A second intravenous extension tube is attached to the 3-way stopcock with the opposite end attached to the blood pressure manometer. The needle is then placed in the compartment and the apparatus kept at the level of the needle. The stopcock is then turned so that it is open in the direction of the intravenous tubing on either side of a syringe. The syringe filled with air is slowly compressed, causing air to move into both extension tubes. The meniscus created by the saline in the extension tube attached to the 18-gauge needle is watched carefully for any movement. As soon as movement occurs in the fluid column, the compartment pressure is read from the blood pressure manometer. This technique, although simple to perform with minimal equipment, may be inaccurate.
Imaging
Imaging has no role in the diagnosis of compartment syndrome, but may show the presence of fractures and soft tissue injuries that are associated with the condition.
Management
Resuscitation
- attend to any coexistent life threats
- ensure adequate oxygenation and systemic circulation if compartment syndrome is potentially present
Specific treatment
- arrange immediate fasciotomy
- remove all constrictive dressings
- elevate the limb to the level of the heart
- consider injury specific measures:
- relieve flexion of the elbow if the forearm is involved
- apply traction for a partially reduced supracondylar fracture
- if there is no relief within 30 minutes, go straight to the operating theatre
Indications for fasciotomy
- A delta pressure <20 mmHg is a definite indication for fasciotomy, <30 mmHg may be a relative indication
- clinical signs of acute compartment syndrome
- absolute pressure is >30 mmHg and the clinical picture is consistent with compartment syndrome
- arterial perfusion has been interrupted for 4 or more hours
Supportive care and monitoring
- provide adequate analgesia
- provide IV hydration to maintain an adequate urine output in case of rhabdomyolysis
- frequent monitoring of compartments and neurovascular status of the affected limb
Disposition
- urgent surgical referral (usually an orthopedic surgeon) and transfer to the operating theatre
- patients require admission for ongoing monitoring
— click to enlarge
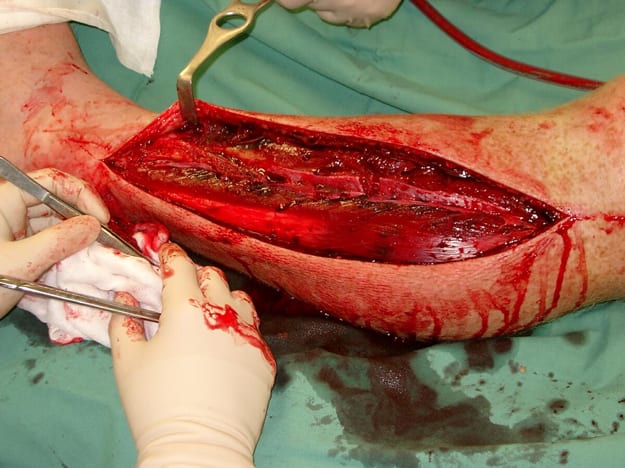
Fasciotomy of the forearm
Fasciotomy of the leg
References and links
LITFL
- Bone and Joint Bamboozler 002 — Muscular Claustrophobia
Journal articles and textbooks
- Newton EJ, Love J. Acute complications of extremity trauma. Emerg Med Clin North Am. 2007 Aug;25(3):751-61, iv. PMID: 17826216.
- Perron AD, Brady WJ, Keats TE. Orthopedic pitfalls in the ED: acute compartment syndrome. Am J Emerg Med. 2001 Sep;19(5):413-6. PMID: 11555801.
Social media and other web resources
- EP Monthly — Diagnosing Compartment Syndrome
- Wheeless’ Textbook of Orthopedics. Compartment Syndrome and Volkmann Contracture.

Critical Care
Compendium
Chris is an Intensivist and ECMO specialist at The Alfred ICU, where he is Deputy Director (Education). He is a Clinical Adjunct Associate Professor at Monash University, the Lead for the Clinician Educator Incubator programme, and a CICM First Part Examiner.
He is an internationally recognised Clinician Educator with a passion for helping clinicians learn and for improving the clinical performance of individuals and collectives. He was one of the founders of the FOAM movement (Free Open-Access Medical education) has been recognised for his contributions to education with awards from ANZICS, ANZAHPE, and ACEM.
His one great achievement is being the father of three amazing children.
On Bluesky, he is @precordialthump.bsky.social and on the site that Elon has screwed up, he is @precordialthump.
| INTENSIVE | RAGE | Resuscitology | SMACC