CT Case 002
A 2yo presents following fall from a chair. She has a GCS of 5 on arrival to ED. This child was intubated and taken for urgent CT brain.
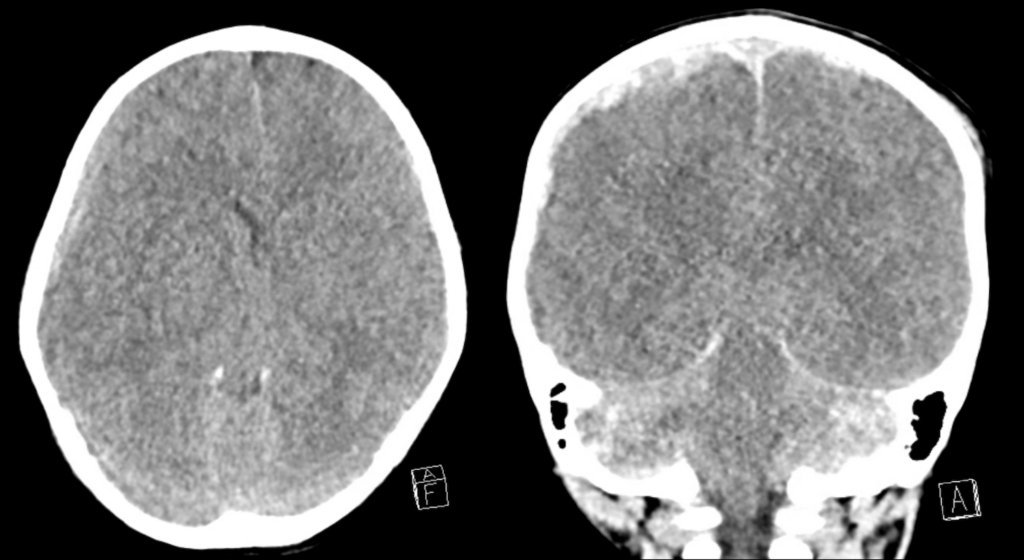
Describe and interpret the images
CT INTERPRETATION
CLINICAL PEARLS
This CT scan shows acute subdural haematoma.
We know it is subdural rather than extradural because of its shape and distribution. A subdural haematoma typically has a crescentic shape as it ‘wraps’ itself around the cerebral cortex. Unlike an extradural haematoma it is not limited by the coronal or lambdoid sutures. In this case we can see that the subdural haematoma on the right crosses the coronal suture.
The blood on this scan is of mixed density and this suggests blood of different ages within the haematoma. On CT, acute blood has a hyperdense (white) appearance, hyperacute blood is less dense as it has not yet clotted.
There are also worrying features of raised intracranial pressure.
While the ventricles are expected to look small in a child compared to an adult, these ventricles are particularly small (ventricular effacement) due to increased intracranial pressure from the haematoma compressing them.
There is also 8mm of midline shift (this is measured at the septum pellucidum).
When there is generalised raised intracranial pressure, brain herniation patterns should be assessed for.
In this case bone windows should also be reviewed to assess for a skull fracture.
This case should also trigger suspicion for non-accidental injury (NAI). While we typically see subdural haemorrhages in older adults after minor trauma (or at times no trauma at all), or in younger adults following higher energy trauma, a subdural haemorrhage in a young child is an unusual finding.
Outcome
This child was taken to theatre for urgent decompression and had a very good recovery.
[cite]
TOP 100 CT SERIES
Dr Leon Lam FRANZCR MBBS BSci(Med). Clinical Radiologist and Senior Staff Specialist at Liverpool Hospital, Sydney
Emergency Medicine Education Fellow at Liverpool Hospital NSW. MBBS (Hons) Monash University. Interests in indigenous health and medical education. When not in the emergency department, can most likely be found running up some mountain training for the next ultramarathon.
Sydney-based Emergency Physician (MBBS, FACEM) working at Liverpool Hospital. Passionate about education, trainees and travel. Special interests include radiology, orthopaedics and trauma. Creator of the Sydney Emergency XRay interpretation day (SEXI).




