Rutherford Morison

James Rutherford Morison (1853-1939) was an English surgeon.
Morison was a pioneer of modern surgery in the North of England with views on surgery some twenty years ahead of his time. As early as 1889 he operated on the stomach and colon; sutured patella fractures with catgut, and operated on torn semilunar cartilages. Along with Sir David Drummond (1852–1932), Morison introduced omentopexy as a cure for ascites
Renowned as a great teacher, Morison founded a school of surgery in Northumberland and Durham, and described as a ‘maker of surgeons’. A medallion portrait was presented by his former house surgeons and led by Mr G. Grey Turner, on his retirement in 1915. The medallion was hung in the theatres of the Royal Victoria Infirmary, Newcastle.
Eponymously remembered for his description of the posterior right subhepatic space known often as the pouch of Rutherford Morison or Morison’s pouch.
Biography
- Born on October 10, 1853 in Hutton-Henry, County Durham. Son of surgeon John Morison surgeon to the Wingate Grange, Trindon Grange, and Rodridge Collieries
- 1874 – LRCP
- 1875 – MB, Edinburgh University
- 1876-1878 Dresser to Joseph Lister (1827-1912); house surgeon to Patrick Heron Watson (1832-1907) at the Edinburgh Royal Infirmary; resident physician to the obstetric ward then resident medical officer to the Cowgate Dispensary
- 1878 – Postgraduate training under Theodor Billroth (1829-1894) in Vienna
- 1879 – FRCS; Commenced general practice in Hartlepool
- 1881 – Elected physician to the Hartlepool Hospital
- 1888 – Assistant surgeon at the Royal Victoria Hospital, Newcastle under the influence of Sir David Drummond (1852 – 1932)
- 1890 – MRCS
- 1897 – Editor of the Journal of the Northumberland and Durham Medical Society
- 1905 – Staff surgeon at the Royal Naval Volunteer Reserve
- 1910 – Professor of surgery at the University of Durham until 1921
- 1916 – Whilst serving in the Northumberland War Hospital, he introduced BIPP to operations
- 1919 – Hon LLD; MA; and DCL Durham. Elected fellow of the American College of Surgeons
- Died on January 9, 1939 in Newcastle-upon-Tyne
Medical Eponyms
Pouch of Rutherford Morison (1894)
Morison pouch, also known as the posterior right subhepatic space, hepatorenal fossa; or subhepatic recess, is a potential space which separates the liver from the right kidney.
As a potential space, it is not filled with any fluid in normal conditions. However, as one of the lowest dependent spaces in the peritoneal cavity, fluid such as ascites or blood often may fill the potential space. It is also a preferential site for metastases and abscesses.
The posterior right subhepatic space is separated from the anterior right subhepatic space by the transverse mesocolon. The space communicates with the right subphrenic space; right paracolic gutter; and the lesser sac (via the epiploic foramen of Winslow).
1894 – Morison published his anatomic description of the hepatorenal space; its role in the surgical treatment of gallbladder disease; and proposed the value of postoperative drainage of that space.
Morison indicated that with the liver retracted upward and the transverse colon downward, one would expose a potential space. The proposed space has an anterior wall bounded right to left by the peritoneal surface of the diaphragm and the undersurface of the right lobe of the liver and gallbladder, extending to the gastrohepatic ligament. The posterior wall formed by the ascending mesocolon over the right kidney and by the duodenum.
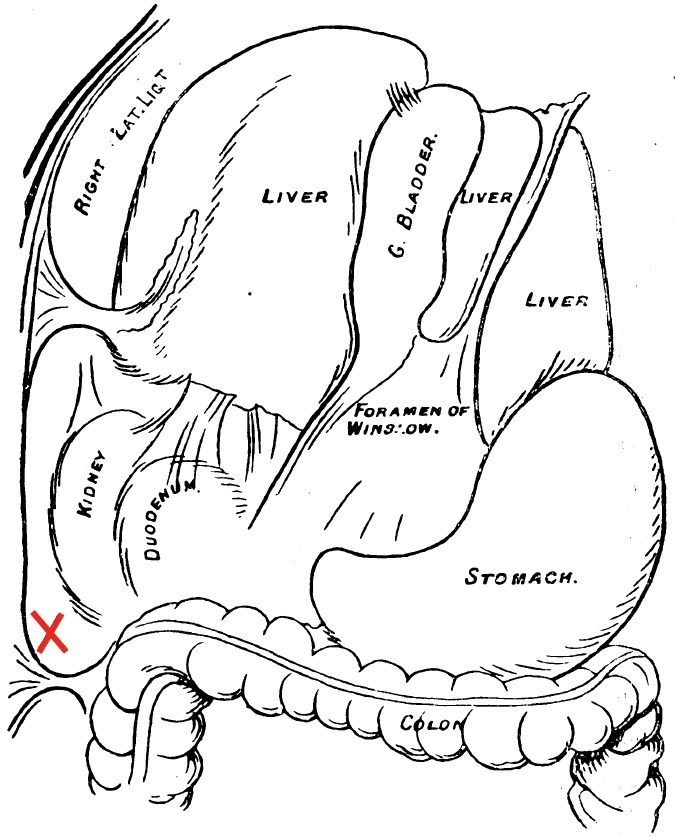
X marks the point for drainage. Rutherford Morison 1894
…underneath the right lobe of the liver there exists a pouch hitherto undescribed, shut off by natural barriers from the general peritoneal cavity….By the relation of nine cases in which the operation for gall-stone was performed in accordance with the principles I was advocating, I endeavored to show that the secret of success in gall-stone operations was efficient drainage of the pouch demonstrated.
Rutherford Morison 1895
Morison proposed that the drain tract for this space would most advantageously exit in the area of the lower pole of the right kidney. Morison viewed provision for adequate postcholecystectomy drainage of this dependent space as a paramount feature of a successful operation.
BIPP: Bismuth, iodoform and paraffin paste
Morison introduced “BIPP” for the prophylaxis of sepsis in traumatic war wounds sutured primarily.
WOUND infection has been the great surgical curse of this war. Until recently all the means I had seen tried at our War Hospital had failed to satisfy the most moderate surgical ambitions. Since I have now developed a simple method, necessitating but few dressings, by which many wounds can be sterilised at once, while in the remainder, so far as my present experience goes, the spread of infection can be checked and limited, I consider it a duty to submit results without further delay.
The paste : Bismuth subnitrate, 1 oz.; iodoform 2 oz.; paraffin liq. q.s. to make a thick paste. I suggest for this the name “Bipp.” A convenient means of applying it was suggested to me by Sister Middleton, of Ward 20. She gave me two bone eggspoon , one to lift the paste and the second to plaster it in and on with.
Rutherford Morison: Lancet, 1916
In the Lancet 1916, I published a method of treating infected, suppurating war wounds, and claimed for it that in some cases sterilisation of the wound could be accomplished at once, and that in the remainder the spread of infection could be checked and limited…
Rutherford Morison: BJS, 1916
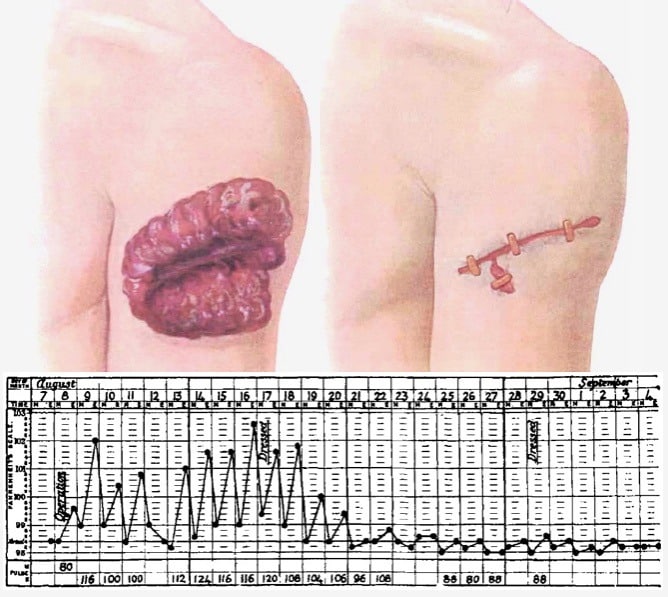
BIPP is still used today in many otolaryngology departments.
BIPP has relatively few adverse effects when used in small quantities. Incidence of BIPP allergy has been estimated as high as 12 per cent with previous exposure, or 1 per cent without. Large quantities have been associated with both bismuth and iodoform toxicity, occasionally causing fatalities. This was first seen by some British army surgeons who deviated from Morrison’s initial regime of a “smear” as well as in modern practice. BIPP should therefore be used with caution when packing large cavities such as those following maxillectomy.
On CT imaging, BIPP can cause image degradation and streak artefacts due to its high attenuation (>3000 Hounsfield units).
Major Publications
- Morison JR The anatomy of right hypochondrium relating especially to operations for gall stones. Br Med J 1894; 2: 968-971 [Morison Pouch]
- Morison R. On Gall-stones. Ann Surg. 1895; 22(2): 181–204. [Morison Pouch]
- Morison R. A Case of ascites due to liver cirrhosis treated by operation. Ann Surg. 1903; 38(3): 361-6
- Morison R. XI. A Clamp for the Fixation of Ununited Fractures. Ann Surg. 1909; 50(6): 1114–1117.
- Rutherford Morison J. An introduction to surgery. 1910
- Rutherford Morison, Richardson WG. Abdominal injuries. 1915
- Rutherford Morison J. The treatment of infected suppurating war wounds. The Lancet, 1916; 188(4850): 268-272. [BIPP]
- Rutherford Morison J. The treatment of infected suppurating war wounds. British Journal of Surgery 1916; 4(16): 659-678 [BIPP]
- Rutherford Morison. Surgical contributions from 1881-1916 – General Surgery. 1916
- Rutherford Morison. Surgical contributions from 1881-1916 – Abdominal Surgery. 1916
- Rutherford Morison J. BIPP treatment of war wounds. 1918
References
Biography
- Biography: Presentation to Rutherford Morison. Br Med J 1915; 2: 455
- Obituary: James Rutherford Morison. Br Med J 1939;1:139; 1939;1:194
- Obituary: James Rutherford Morison. Lancet; 233(6021): 178
- Biography: James Rutherford Morison. Plarr’s Lives of the Fellows Online. Royal College of Surgeons of England.
- Bibliography. James Rutherford Morison. World Cat Identities
Eponymous terms
- Gilliam JW Jr, Schein CJ. The Morison Pouch. Arch Surg. 1976; 111(3): 227-228
- Hajdu N, de Lacey G. The Rutherford Morison pouch; a characteristic appearance on abdominal radiographs. Br J Radiol. 1970; 43(514): 706-9
- Crossland, G., & Bath, A. (2011). Bismuth iodoform paraffin paste: a review. The Journal of Laryngology & Otology, 2011; 125(9): 891-895.
Rutherford Morison Medallion Portrait
You, Sir, might be disappointed if I did not say that we have all felt the value of your chastening, but your honesty of purpose and absolute fairness always supplied the balm with the Sting, and we gratefully acknowledge the lessons impressed in this way.
George Grey Turner, presenting medallion to his boss in 1915

Rutherford Morison Medallion Portrait
Brit med J 1915, 2, 455
Eponym
the person behind the name
DM (UWA), BM (Indiana), FMusA, LMusA. Resident Medical Officer, Sir Charles Gairdner Hospital. Basic Surgical Streaming Program. Professional violinist, now aspiring surgeon. Loves music, opera, and operating.
BA MA (Oxon) MBChB (Edin) FACEM FFSEM. Emergency physician, Sir Charles Gairdner Hospital. Passion for rugby; medical history; medical education; and asynchronous learning #FOAMed evangelist. Co-founder and CTO of Life in the Fast lane | On Call: Principles and Protocol 4e| Eponyms | Books |


Many thanks for this item. I worked for George Feggetter, who worked for Grey Turner, who worked for Rutherford Morison, who was Lister’s dresser in Edinburgh. I was in the Newcastle RVI from 1966 as a houseman until 1980 when I went to Middlesbrough as a consultant surgeon. I remember the plaque outside Theatre One very well as I was on the Prof’s unit for a year.