Plaster slab
First job of the shift today was to review the elbow of a patient 3 days after the application of a forearm cast.
The patient was a stoic young chap suffering from a minor sprain of his ulna collateral ligament following a fall from a skateboard earlier in the week. Unlike some of my self-diagnosing hypochondriacal colleagues, he was actually suffering from a ‘real’ illness at the time of his initial presentation…
Unfortunately on the day of his presentation we were not able to provide an appropriate light-weight splint to assist with immobilisation of the affected digit, and instead the resident was directed to create a temporary splint from plaster of Paris (POP) to alleviate his discomfort.
Prior to examining the patient I try to run through the potential complications of POP applications in my head to make the examination rapid and effective. In general we see ‘bouncebacks‘ following POP applications for a variety of reasons. I examine the affected limb for evidence of neurovascular compromise, look for iatrogenic local causes for pain and enquire as to the potential patient related causes of persisting discomfort.
- Vascular
- Impaired arterial supply (pale skin with cool, pulseless, painful distal parts)
- Impaired venous return (swelling, discomfort or pain, and a blue colour in the skin and under the nails)
- Neurological
- Loss of power, tingling and numbness distal to the cast secondary to nerve impingement, local swelling and neuropraxia
- Local pain
- Plaster sores or fracture blisters (burning, itching or stabbing pain following swelling post fracture reduction or post cast application)
- Poorly fitted cast with local compression
- Systemic
- Deep venous thrombosis secondary to immobilisation leading to pulmonary embolism
- Patient related
- Falling off the same device that caused the injury in the first place
- Having a bath/shower/swim with the cast in situ etc etc
However, in this case it was the proximal joint (the elbow) which was troublesome…and, having reviewed the 15 layer thick, 1.4kg circumferential forearm ‘slab’ I now have to add proximal joint tenosynovitis and epicondylitis to the list of potential iatrogenic complications…
Further Reading
- A better way to get plastered
- Getting a leg over
- Buddy strap no more
- Simon and Neil get plastered
- Plaster slab

TRAUMA LIBRARY
BA MA (Oxon) MBChB (Edin) FACEM FFSEM. Emergency physician, Sir Charles Gairdner Hospital. Passion for rugby; medical history; medical education; and asynchronous learning #FOAMed evangelist. Co-founder and CTO of Life in the Fast lane | On Call: Principles and Protocol 4e| Eponyms | Books |

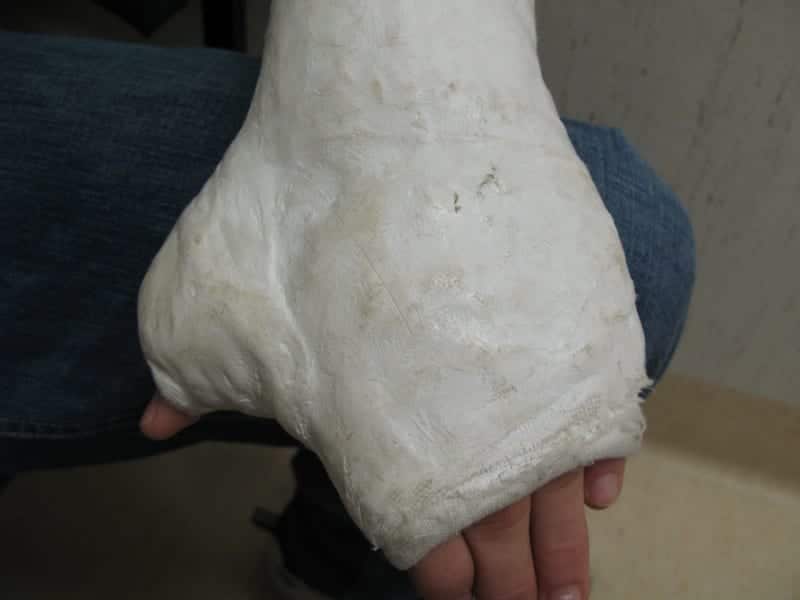


Glad I’m not sawing that off