CT Case 005
A 75 yo female is found on the floor at home with reduced level of consciousness. She was last seen well over 12 hours prior.
She has a background of atrial fibrillation on apixaban.
On hospital arrival she was found to have a GCS of 7 and a dense right sided hemiparesis.
A non-contrast CT scan of the brain and CT angiogram are performed.
Describe and interpret the images
CT INTERPRETATION
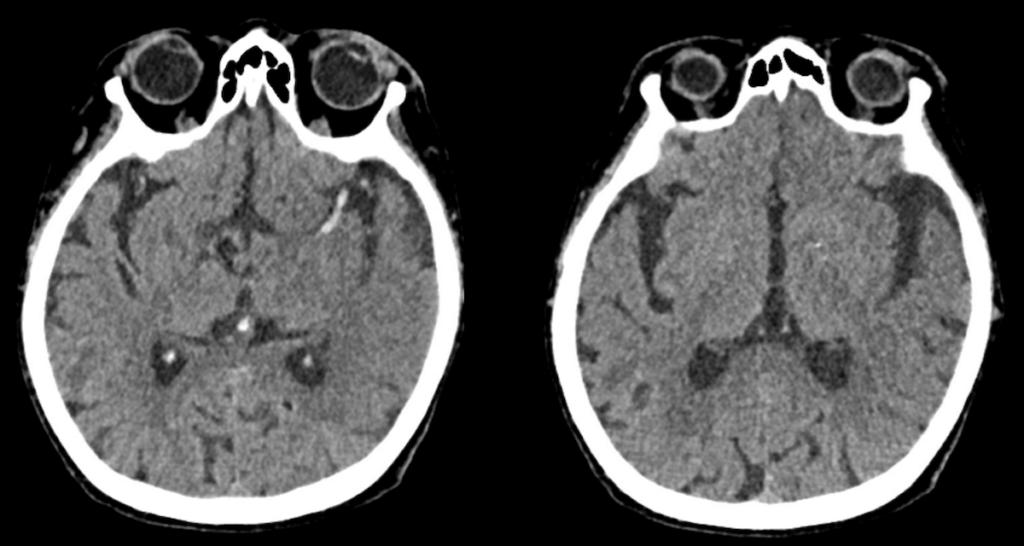
CT non-contrast
- There is no sign of intracranial haemorrhage.
- There is reduced grey-white matter differentiation in the left insula cortex and temporal lobe
- There is a long hyperdense thrombus in the terminal left internal carotid artery (ICA) and middle cerebral artery (MCA) (M1).

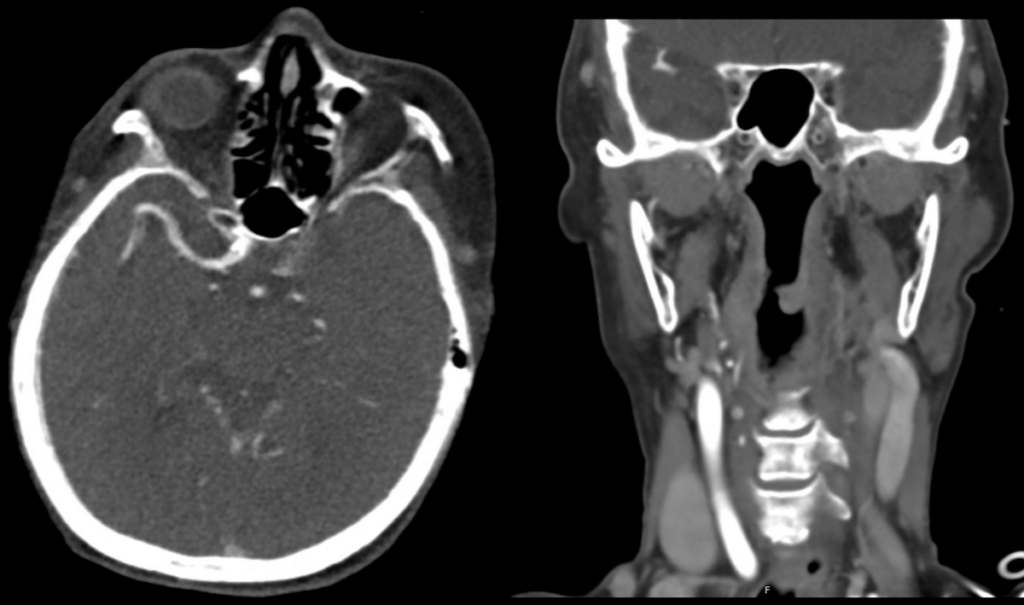
CT angiogram COW (Circle of Willis)
- There is no enhancement of the terminal ICA and MCA.
- The left common carotid is poorly opacified.

CLINICAL CORRELATION
These scans show that our patient unfortunately has a very large and established infarct which is not amenable to thrombolysis or endovascular clot retrieval.
A CT stroke series includes 3 phases of scanning;
- CT non-contrast, CT angiogram and CT perfusion study.
CT non-contrast scan
Primarily helps to exclude a haemorrhagic stroke or other pathology (eg tumour).
A hyperacute ischaemic stroke may appear normal on non-contrast CT, especially if CT imaging is undertaken less than 4 hours post symptom onset.
Reduced or loss of grey-white matter differentiation is an early sign of acute ischemia or infarction.
The insula cortex has poor collateral blood supply and ischaemic occurs earlier here. For this reason, it is a good place to look for subtle signs of infarction, as changes can be seen here first.
Also look for a hyperdense clot sign. The acute thrombus within the occluded artery will appear hyperdense. It is only occasionally visible. In this case there was thrombus seen occluding the ICA, MCA.
CT angiogram COW (Circle of Willis)
An arterial phase scan, it can confirm vessel occlusion and can also be used to guide further treatment such as thrombolysis or interventional radiology.
On this particular scan there is also a trap for young players (myself included).
Note, that there is only limited contrast within the left common carotid artery.
At first glance this might be interpreted as a clot in the common carotid. Actually, there is no clot here, but it is just a sign of poor blood flow in the carotid. The clots more distal in the ICA and MCA are impeding distal flow, this causes a pressure build up so it is difficult for contrast media to reach the common carotid despite it being patent.
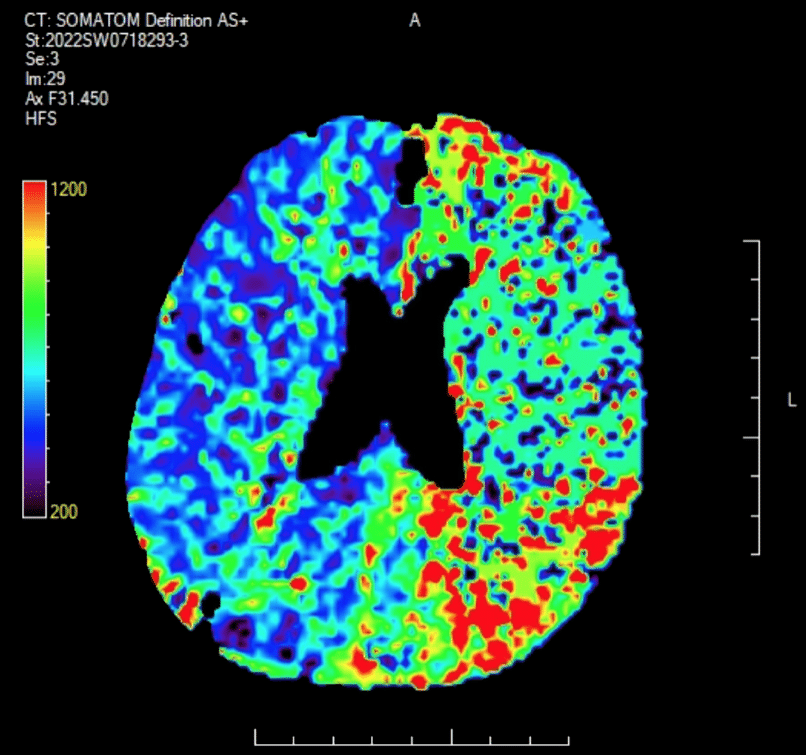
CT perfusion scan
Used to distinguish between salvageable ischaemic brain tissue (penumbra) and infarcted brain tissue (infarct core).
The penumbra is the part of brain tissue that has compromised blood flow but has not yet undergone infarction.
The infarct core on the other hand is the brain tissue which has already died and which cannot recover.
The degree of mismatch between the penumbra size and the infarct core size is one parameter used to determine if the patient will benefit from reperfusion therapies (thrombolysis or clot retrieval).
Logically, patients with small infarct core and large ischaemic penumbra are those most likely to benefit from reperfusion therapies.
[cite]
TOP 100 CT SERIES
Dr Leon Lam FRANZCR MBBS BSci(Med). Clinical Radiologist and Senior Staff Specialist at Liverpool Hospital, Sydney
Emergency Medicine Education Fellow at Liverpool Hospital NSW. MBBS (Hons) Monash University. Interests in indigenous health and medical education. When not in the emergency department, can most likely be found running up some mountain training for the next ultramarathon.
Sydney-based Emergency Physician (MBBS, FACEM) working at Liverpool Hospital. Passionate about education, trainees and travel. Special interests include radiology, orthopaedics and trauma. Creator of the Sydney Emergency XRay interpretation day (SEXI).



