ECG Case 112
35 yr old male who presented to the Emergency Department complaining of palpitations, dyspnoea, and lightheadedness for the preceding hour. He has no known past medical history.
Vital signs: BP 115/65, RR 20, sats 98% RA, T 36.6
Describe and interpret this ECG
ECG ANSWER and INTERPRETATION
Rate:
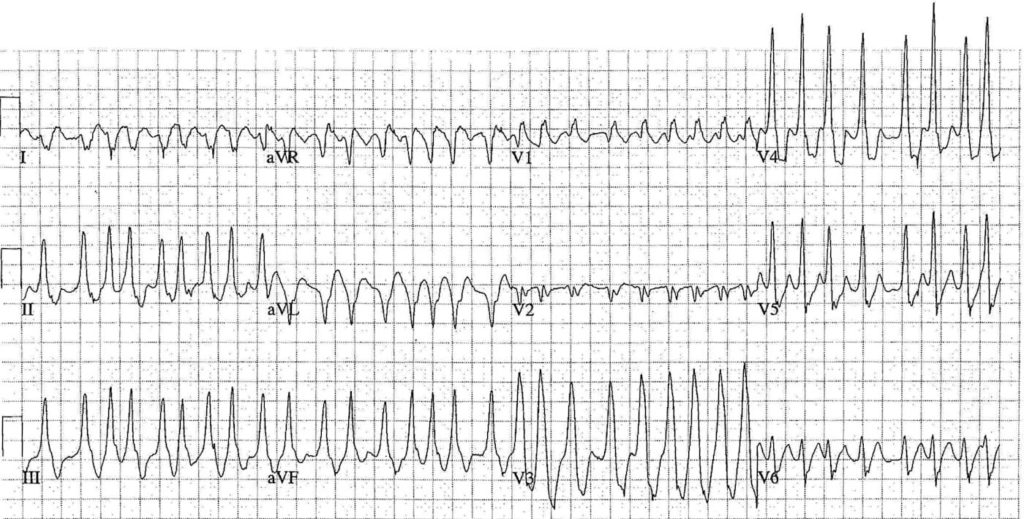
- Mean ventricular rate ~205 bpm
- Variable rate between 140 – 300 bpm
- The very high rates are due to conduction via an accessory pathway with a short effective refractory period
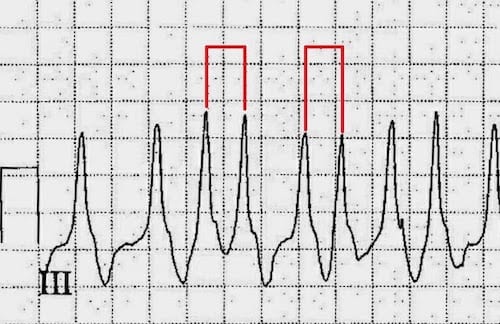
- Image below shows R-R interval of 200ms = rate 300bpm
Rhythm:
- Irregular
Axis:
- Right axis deviation (105 deg)
Intervals:
- QRS – Prolonged (160ms)
Additional:
- Variable QRS Morphology
Interpretation:
- Pre-excited Atrial Fibrillation (AF) a.k.a
- AF with Wolff-Parkinson-White (WPW)
- Fast Broad Irregular (FBI) tachycardia
CLINICAL PEARLS
Why is this so important ?
This is a clinical situation in which significant harm to the patient can occur if the ECG features are not recognised and acted on appropriately.
The concern with pre-excited AF is the ability for the accessory pathway to conduct at much higher rates than the AV node with the potential for degeneration into ventricular fibrillation.
It is for this reason that any drugs which block the AV node are ABSOLUTELY CONTRAINDICATED in this scenario including adenosine, calcium-channel blockers, beta-blockers and digoxin. If the AV node is blocked then there is increased conduction via the accessory pathway which may precipitate ventricular fibrillation.
Put simply if you give the patient AV nodal blocking drugs you might kill them.
The safest and easiest method to restore sinus rhythm is synchronized cardioversion.
If you have a patient you are concerned about the risks of sedation for cardioversion I would suggest getting expert assistance from anaesthetics and urgent cardiology advice on how to proceed.
Chemical cardioversion is a possible alternative in stable patients with iv procainamide being the commonly used agent. This drug is not readily available in Australia, and I personally have no experience using it.
Amiodarone is available in Australia although it’s utility in the treatment of stable AF with WPW is controversial. The Australian Resuscitation Council Guideline 11.9 Managing Acute Dysrhythmias states that ‘Amiodarone may be considered for hemodynamically stable patients with AF involving conduction over an accessory pathway’ [Class C, LoE III-2]. This statement should be tempered against case reports of potential harm, see the paper below:
- Tijunelis MA, Herbert ME. Myth: Intravenous amiodarone is safe in patients with atrial fibrillation and Wolff-Parkinson-White syndrome in the emergency department. CJEM. 2005 Jul;7(4):262-5
I’ll repeat the statement above that synchronised DC cardioversion is the safest method for treating stable and unstable pre-excited atrial fibrillation; if chemical cardioversion is being considered then urgent cardiology advice is required.
Remember all these patients must be referred to cardiology services for EP follow-up and consideration for ablation.
CLINICAL OUTCOME
What happened in this case?
Well the patient underwent synchronized DC cardioversion under sedation and the post cardioversion ECG is below.
This ECG shows WPW as evidence by short pr, QRS prolongation, and delta waves (best appreciated in leads V3-5). The delta wave axis suggests a left anterolateral accessory pathway, for more on accessory pathway localisation check out the references below:
- Arruda MS, McClelland JH, Wang X, Beckman KJ, Widman LE, Gonzalez MD, Nakagawa H, Lazzara R, Jackman WM. Development and validation of an ECG algorithm for identifying accessory pathway ablation site in Wolff-Parkinson-White syndrome. J Cardiovasc Electrophysiol. 1998 Jan;9(1):2-12. PMID: 9475572
- ECGpedia Wolff-Parkinson-White Pattern [Scroll down for Arruda et al. and Milsteinet al. algorithm charts]
- ECG Library – Pre-excitation syndromes
- Dr Smith’s ECG blog – Wide complex tachycardia
TOP 150 ECG Series
Emergency Medicine Specialist MBChB FRCEM FACEM. Medical Education, Cardiology and Web Based Resources | @jjlarkin78 | LinkedIn |


Question: Does the above ECG (AF + WPW) with widened QRS indicate orthodromic or antidromic conduction?
Neither. Wide QRS complex is due to abnormal ventricular depolarisation (ie not following the usual conduction pathway using bundle of his).
This is not an AVRT; due to the fact it’s not a re-entrant tachycardia. AF is just conducted at a very fast rate using accessory pathway. No AVRT; thus no ortho/anti.
How to differentiate AF+RBBB vs AF+WPW in this case?
Usually, AF with RBBB should have slow conduction rates since AV node does not allow for close to 300 bpm ventricular rate