Half an 8 ball
aka Ophthalmology Befuddler 030
A 26 year-old man sustained an injury of uncertain mechanism to his left eye while at the bottom of a ruck during a game of rugby. Fortunately, his team went on to win 24-16.
However he still has a problem. His left eye looks like this:
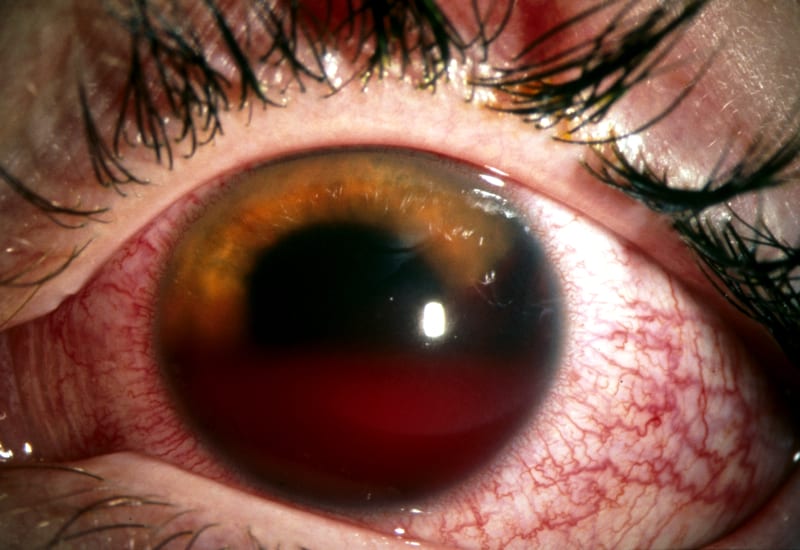
Questions
Q1. What is the likely diagnosis?
Answer and interpretation
Anterior hyphema — a collection of blood or clot in the anterior chamber, it is usually visible to the naked eye. There is also diffuse conjunctival injection.
When clot fills the anterior chamber it is called an 8-ball hyphema. Over time red cells tend to settle on the bottom of the anterior chamber if the patient is upright. When lying down the hyphema may be detectable as a diffuse haziness in the anterior chamber. A microhyphema is only detectable with a slit lamp.
Q2. What features should be obtained on history and examination?
Answer and interpretation
History:
- Symptoms — pain, blurred vision, loss of vision — time course of vision loss may suggest rebleed if recurrent, or continued bleed if longer duration.
- Injury — Blunt trauma? What happened? When? How?
(spontaneous hyphemas may occur in those with diabetic neovascularisation, previous surgery or a bleeding diathesis) - Bleeding diathesis? — disorders, medications, history of sickle cell disease (glaucoma more likely)
- Use of eye protection
Examination:
- Visual acuity — variable
- External examination — check for concomitant head and facial/ periorbital injury.
- Pupils — direct response to light may be decreased in large hyphemas or the pupil may be obscured by blood.
- Tonometry — check for secondary glaucoma.
- Slit lamp exam — measure extent (height) of hyphema, assess for clots. Check for microhyphema. Rule out penetrating injury and other eye injuries.
- fundoscopy and red reflex — blood may cause loss of red reflex, look for retinal injury.
Hyphema grades:
- Grade 1: Layered blood occupying less than one third of the anterior chamber
- Grade 2: Blood filling one third to one half of the anterior chamber
- Grade 3: Layered blood filling one half to less than total of the anterior chamber
- Grade 4: Total clotted blood, often referred to as blackball or 8-ball hyphema
Q3. What is the investigation and management of this condition?
Answer and interpretation
Consider CT or XR orbits if concerned about blowout fracture or head injury.
Management:
- oral analgesia and topical cycloplegics for comfort. Consider antiemetics.
- The patient should remain upright (helps RBCs settle so that they do not plug the trabecular meshwork which may lead to high intraocular pressures (IOPs))
- Apply an eye shield — not a patch, which may prevent recognition of sudden visual loss form a rebleed
- Avoid agents that may contribute to a bleeding diathesis.
- Treat secondary glaucoma
- Surgical evacuation may be required if the hyphema fails to resolve, there is a rebleed or secondary glaucoma occurs.
- Associated injuries need to be identified and treated
Paracentesis as treatment for glaucoma secondary to blunt eye trauma with hyphema (RootAtlas)
Q4. Which patients with this condition require admission to hospital?
Answer and interpretation
Admission for bedrest is now no longer the norm. Admission is usually indicated in these settings:
- noncompliant patients
- children (especially if suspected NAI or <age 8 years due to risk of amblyopia)
- increased IOPs
- sickle cell disease
- bleeding diathesis or blood dyscrasia
Q5. What is appropriate follow up for patients that are discharged? What advice should be given to the patient?
Answer and interpretation
- Ophthalmology follow up on a daily basis (or on day 3 for a microhyphema).
- Ask the patient to refrain from strenuous physical activities (including Valsalva maneuvers) for 1 week after the initial injury or a rebleed. This period should be extended if blood remains in the anterior chamber
Q6. What are the possible complications of this condition?
Answer and interpretation
- rebleeding (do not confuse with hemolysis)
- glaucoma
- corneal staining
- traumatic iritis
Your patient is discharged from the emergency department with ophthalmology follow up arranged. However, he returns after 3 days with throbbing eye pain, tearing and photophobia.
Q7. What is the likely diagnosis?
Answer and interpretation
Traumatic iritis
Inflammation of the iris occurring within 3 days of trauma, typically presenting as a dull aching/ throbbing pain, with tearing and photophobia (both direct and consensual).
For more on uveitis check out Ophthalmology Befuddler 016
Q8. What are the examination findings of this new condition?
Answer and interpretation
Examination:
- Visual acuity — normal or decreased
- Pupils — The affected pupil may be smaller and dilate poorly, or larger in the presence of iris sphincter tears. There is pain in the traumatised eye on direct and consensual light exposure.
- Slit lamp: Anterior chamber — cells and flare; Perilimbal conjunctival injection may be present.
- Tonometry — IOPs may be high or low.
Q9. What is the management of this new condition?
Answer and interpretation
Management:
- Oral analgesia
- Topical cycloplegics to prevent synechiae formation and ciliary spasm
- An ophthalmologist may use topical steroids in the highly symptomatic patient (but not if there is an epithelial defect)
- Ophthalmology follow up should occur within a week.
References
- Ehlers JP, Shah CP, Fenton GL, Hoskins EN. The Wills Eye Manual: Office and Emergency Room Diagnosis and Treatment of Eye Disease Lippincott Williams & Wilkins
- NSW Statewide Opthalmology Service. Eye Emergency Manual — An illustrated Guide. [Free PDF]
OPHTHALMOLOGY BEFUDDLER
Chris is an Intensivist and ECMO specialist at The Alfred ICU, where he is Deputy Director (Education). He is a Clinical Adjunct Associate Professor at Monash University, the Lead for the Clinician Educator Incubator programme, and a CICM First Part Examiner.
He is an internationally recognised Clinician Educator with a passion for helping clinicians learn and for improving the clinical performance of individuals and collectives. He was one of the founders of the FOAM movement (Free Open-Access Medical education) has been recognised for his contributions to education with awards from ANZICS, ANZAHPE, and ACEM.
His one great achievement is being the father of three amazing children.
On Bluesky, he is @precordialthump.bsky.social and on the site that Elon has screwed up, he is @precordialthump.
| INTENSIVE | RAGE | Resuscitology | SMACC
