Headache classification
Deconstructing headache classification
Headache is a symptom like any other patient complaint, such as back pain. The headache may be a primary headache disorder, such as a cluster headache, or it might be secondary to another issue, such as a brain tumour.
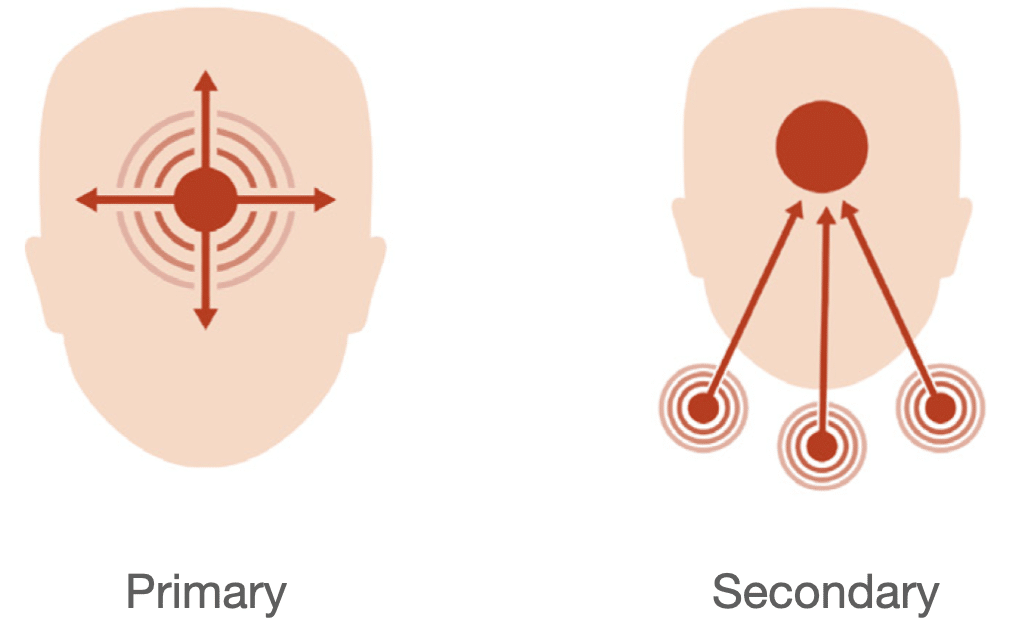
The main difference between primary and secondary headache disorders is whether or not it is the primary or secondary clinical condition.
Primary headache disorders
Over 90% of patients presenting to their primary care physician with headache have one of the four primary headache disorders:
1. Migraine
This can include migraine with aura or without aura, and aura without headache. An aura refers to a group of symptoms—visual, sensory, or other central nervous system symptoms—which are fully-reversible, develop gradually, and are usually followed by headache and other migraine symptoms such as nausea.
2. Tension-type headaches
This type of headache includes episodic and frequent tension-type headaches.
3. Trigeminal autonomic cephalalgias
This is a broad category which includes cluster headaches, paroxysmal hemicrania, and short-lasting, unilateral neuralgiform headache with conjunctival injection and tearing (SUNCT).
4. Other primary headaches
Other primary headache disorders include cough headache, exercise headache, and hypnic headaches.

The four categories of primary headache disorders according to the International Classification of Headache Disorders (ICHD-3) are migraine, tension, trigeminal autonomic cephalalgias, and other (which includes cough headache, exercise headache, and hypnic headaches).
Secondary headache disorders
In general, a headache should be considered secondary if it appears or worsens during another illness, and especially if the headache fluctuates with changes in the underlying condition.
There are eight secondary headache disorders according to the International Classification of Headache Disorders (ICHD-3)
- Headache attributable to trauma
- Vascular disorders
- Nonvascular intracranial disorders
- Substance use or withdrawal
- Infection
- Disorders of haemostasis
- Disorders affecting the structures of the head or neck
- Psychiatric disorders
The International Classification of Headache
The International Headache Society designed a classification system to help classify the many different potential presentations of headache. Currently in its third edition, the International Classification of Headache Disorders (ICHD-3) identifies 14 major categories of headache, which themselves are divided into three broad groups: the primary headache disorders (comprising categories 1–4), the secondary headache disorders (composed of categories 5–12), and finally, categories 13 and 14, representing the cranial neuropathies and neuralgias.
The ICHD-3 system was modelled on the Diagnostic and Statistical Manual of Mental Disorders, Fifth Edition (DSM-V). It incorporates both clinical criteria and laboratory features to establish diagnoses. It is hierarchical and one can characterise using multiple levels of complexity that are characterised by sequential numbering (however, it often isn’t necessary to break down your patient’s headache into the smallest of subcategories). The first and second digits of the classification are useful in primary care, and the third, fourth, and fifth digits are useful for neurology and headache specialty centres.
Using the classification system
- Use the characteristics of the headache to categorise the headache type, not characteristics of the patient.
- The headache phenotype that is present currently, and especially over the last year, is considered to be the most current diagnosis.
- All the criteria in the classification scheme must be fulfilled in order to achieve an accurate diagnosis.
- The criteria often include a specific number of attacks that must have been experienced before any one headache type can be diagnosed.
- Many patients may have more than one headache type, and multiple headache types must be assessed and diagnosed individually.
This is an edited excerpt from the Medmastery course Headache Masterclass by Robert Coni, DO, EdS, FAAN. Acknowledgement and attribution to Medmastery for providing course transcripts.
- Coni R. Headache Masterclass. Medmastery
- Coni R. Clinical Neurology Essentials. Medmastery
- Simmonds GR. Neurology Masterclass: Managing Common Diseases. Medmastery
- Simmonds GR. Neurology Masterclass: Managing Emergencies. Medmastery
References
Neurology Library: The primary headache disorders
- Coni R. Deconstructing headache classification. LITFL
- Coni R. Headache aetiology. LITFL
- Coni R. Migraine headache. LITFL
- Coni R. Tension headache. LITFL
- Coni R. Cluster headache. LITFL
- Coni R. Trigeminal autonomic cephalalgias. LITFL
- Coni R. Other primary headaches. LITFL
- Coni R. Chronic daily headaches. LITFL
Neurology Library
Robert Coni, DO, EdS, FAAN. Vascular neurologist and neurohospitalist and Neurology Subspecialty Coordinator at the Grand Strand Medical Center in South Carolina. Former neuroscience curriculum coordinator at St. Luke’s / Temple Medical School and fellow of the American Academy of Neurology. In my spare time, I like to play guitar and go fly fishing. | Medmastery | Linkedin |
BMBS (The University of Nottingham) BMedSci (The University of Nottingham). Emergency Medicine RMO at Sir Charles Gairdner Hospital Perth, WA. Interested in Medical Education and Emergency Medicine. Swimmer and frequent concert attendee.


