Chronic daily headaches
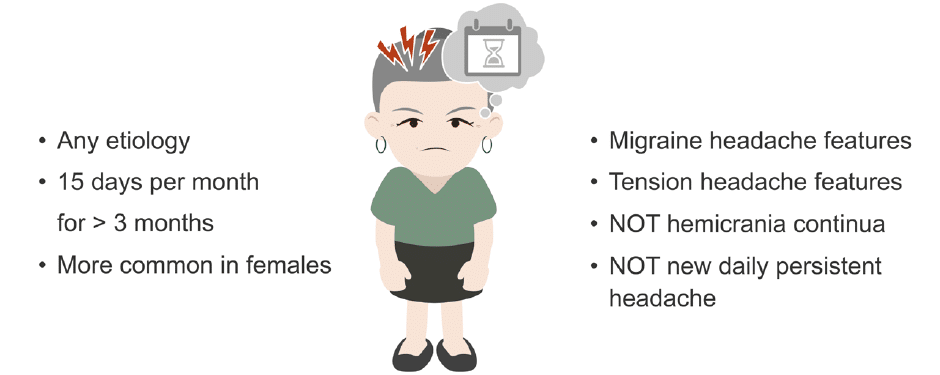
Chronic daily headaches are defined as headaches which occur at least 15 days or more per month for at least three months, regardless of the underlying headache aetiology.
Chronic daily headaches can have migraine features, tension headache features, or even a mixture of the two. However, in order to be considered a chronic daily headache there must not be any characteristics of hemicrania continua (HC) or new daily persistent headache (NDPH).
Prevalence of chronic daily headaches
Chronic daily headaches are most common among middle-aged adults between 30 and 50 years of age. The female to male ratio is around 3:1. The prevalence of chronic headache is 4–5%, with an incidence of 3% per year. The incidence of new onset chronic migraine in patients with episodic migraine is around 2.5% per year.
Diagnosing chronic daily headaches
Accurately diagnosing chronic daily headaches can be difficult. It may be difficult to identify the primary headache type. Given the overlap in symptoms, it may be almost impossible to differentiate chronic migraine without aura from chronic tension headaches. For example, sometimes migraine without aura evolves slowly, leading to misdiagnosis as chronic tension headache.
The defining moment of when a headache becomes chronic may also be difficult to pinpoint. While cluster headaches also are a type of headache that occurs repeatedly over a number of days, cluster headaches only become chronic when they are characterized by a lack of periodic remission normally seen in the cluster syndrome.
The diagnosis can easily become even more muddled when complicated by responses to headache medications such as triptans.
Complicating secondary factors
Secondary factors can further complicate the diagnosis of chronic daily headaches.
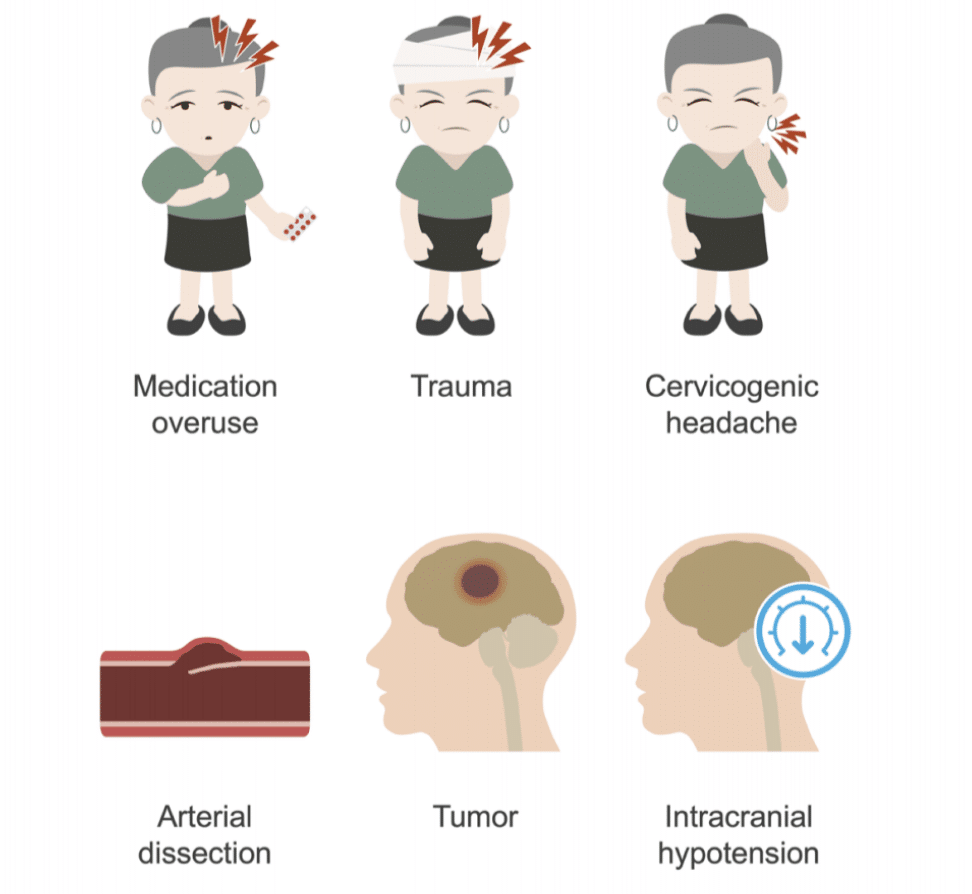
Diagnosis of chronic daily headaches can be further complicated by secondary factors, such as medication overuse, post traumatic headache, cervicogenic headache, and other more serious causes such as arterial dissection, tumour, and intracranial hypotension from a cerebrospinal fluid leak or pseudotumor cerebri.
Risk factors for chronic daily headaches
- Socioeconomic status: more common in individuals of lower income and / or less education.
- Obesity is a risk factor, for unknown reasons.
- Other neurological conditions: A history of migraine and depression is frequently found in those who suffer from chronic daily headaches. And, sufferers tend to report a higher incidence of other pain associated conditions, particularly musculoskeletal pain.
- Stress: Those that suffer from chronic daily headaches also tend to report associated stressful life events including death in the family or illness, moves, job changes, marital status changes, and child-related issues.
- Sleep disturbances; particularly snoring, are more common in patients with chronic daily headaches. And studies show this to be independent of obstructive sleep apnoea. Interestingly, chronic daily headache patients tend to sleep either too much or not enough.
- High medication use: Individuals with chronic daily headaches tend to have high medication use, as documented by many authors. It is estimated that approximately one third of chronic daily headache patients overuse medicines.
Treating chronic daily headaches
Due to all these complicating factors, frequent or daily to near-daily headaches are challenging to treat and will often lead to referral to a tertiary centre.
Still, by accurately categorising these headaches treatments can be successful. First, potential causes of secondary headaches must be excluded. Treatment approaches will then vary based on the type of primary headache which has become chronic.
For example, a chronic migraine versus chronic tension headache versus new daily persistent headache may all have individual and differing treatment strategies.
This is an edited excerpt from the Medmastery course Headache Masterclass by Robert Coni, DO, EdS, FAAN. Acknowledgement and attribution to Medmastery for providing course transcripts.
- Coni R. Headache Masterclass. Medmastery
- Coni R. Clinical Neurology Essentials. Medmastery
- Simmonds GR. Neurology Masterclass: Managing Common Diseases. Medmastery
- Simmonds GR. Neurology Masterclass: Managing Emergencies. Medmastery
References
- The International Classification of Headache Disorders 3rd edition
- Rizzoli P, Mullally WJ. Headache. Am J Med. 2018 Jan;131(1):17-24.
- Goadsby PJ. Trigeminal autonomic cephalalgias. Continuum (Minneap Minn). 2012 Aug;18(4):883-95
- Burish M. Cluster Headache and Other Trigeminal Autonomic Cephalalgias. Continuum (Minneap Minn). 2018 Aug;24(4, Headache):1137-1156
Neurology Library: The primary headache disorders
- Coni R. Deconstructing headache classification. LITFL
- Coni R. Headache aetiology. LITFL
- Coni R. Migraine headache. LITFL
- Coni R. Tension headache. LITFL
- Coni R. Cluster headache. LITFL
- Coni R. Trigeminal autonomic cephalalgias. LITFL
- Coni R. Other primary headaches. LITFL
- Coni R. Chronic daily headaches. LITFL
Neurology Library
Robert Coni, DO, EdS, FAAN. Vascular neurologist and neurohospitalist and Neurology Subspecialty Coordinator at the Grand Strand Medical Center in South Carolina. Former neuroscience curriculum coordinator at St. Luke’s / Temple Medical School and fellow of the American Academy of Neurology. In my spare time, I like to play guitar and go fly fishing. | Medmastery | Linkedin |
BMBS (The University of Nottingham) BMedSci (The University of Nottingham). Emergency Medicine RMO at Sir Charles Gairdner Hospital Perth, WA. Interested in Medical Education and Emergency Medicine. Swimmer and frequent concert attendee.


