Abdominal CT: body wall
Evaluating the body wall
It might be tempting to overlook the bones, body wall, and musculoskeletal structures as these are rarely the reason for ordering a CT exam, but there may be important findings to be discovered and described. Let’s start by working through the evaluation of the body wall.
Musculature of the body wall
The first thing you will notice is that we can finally benefit from symmetry. Specifically, we can use the symmetry of the musculature and bones to help us identify an abnormality.
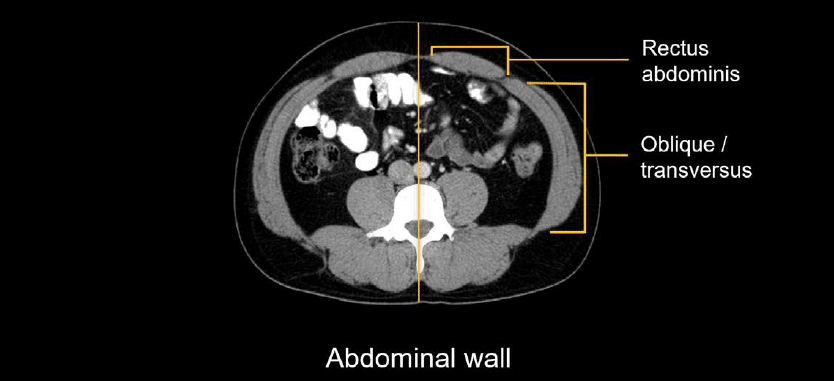
The important musculature of the abdominal wall includes the paired rectus abdominis muscles anteriorly (i.e., the abs) and the oblique and transversus abdominis muscles found on the lateral body wall.
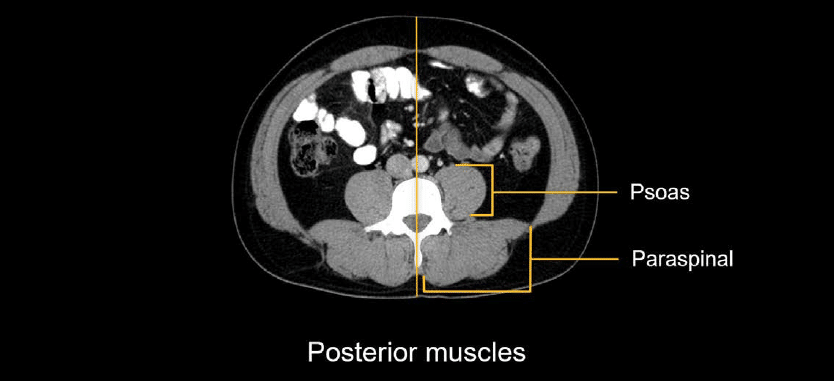
The grouping of posterior muscles surrounding the spine have individual names but are commonly referred to collectively as the paraspinal muscles. Let’s not forget the psoas muscles running along the medial spine in the retroperitoneum.
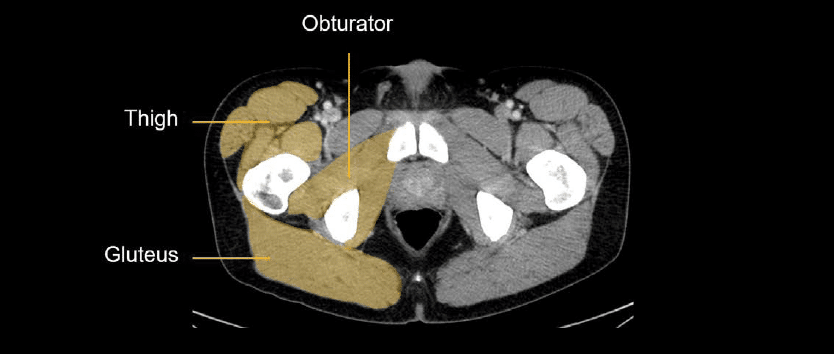
In the pelvis are the gluteus muscles posteriorly, obturators in the deep pelvis, and several different upper thigh muscles.
Rather than trying to memorize them, I’ve found it helpful to deepen my knowledge of the specific muscles on CT when they were involved in various pathologies, looking them up when needed so I can report with greater accuracy. So, give yourself a little time and experience to learn the musculature in detail.
Subcutaneous fat
The subcutaneous fat might seem boring to evaluate, and it should be! You should expect relatively dark and featureless areas characterized by a few small vessels.
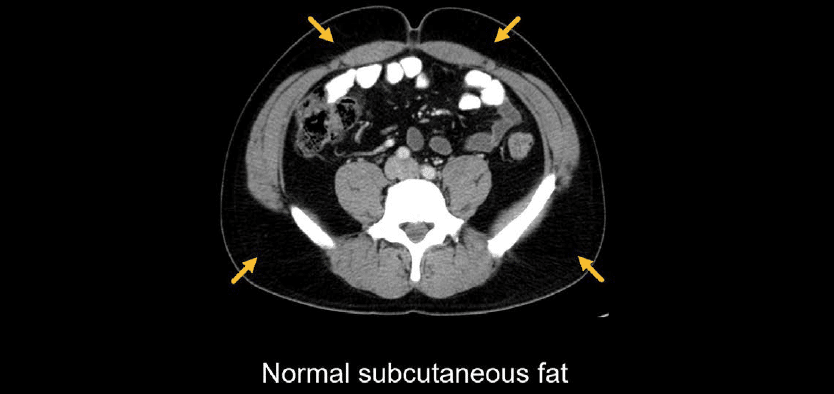
Don’t let the darkness lull you to sleep! Subcutaneous fat can be involved in disease processes as well. Stranding throughout the normally dark fat indicates fluid. This is often related to the movement of fluid out of the vasculature and into the soft tissue, referred to as third spacing, which can be caused by a variety of medical conditions such as heart failure, low albumin, and sepsis.
In the example below of a patient with diffuse oedema throughout the body wall fat, there is normal dark fat posteriorly but diffuse stranding anteriorly in the fat, making it look greyer.

Sometimes you will see stranding, nodules, or calcifications related to the injection of subcutaneous medications like insulin. These are called injection granulomas.
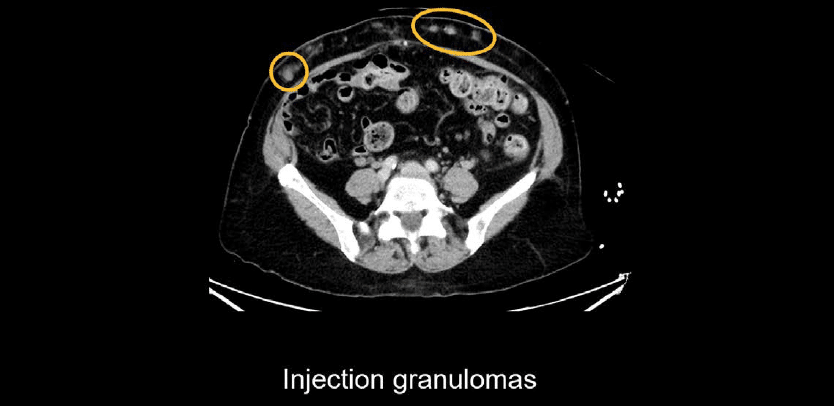
Skin
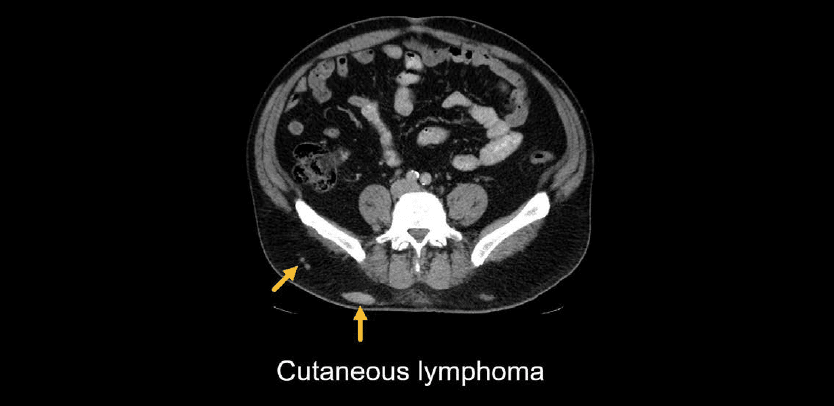
Some tumours like lymphoma and melanoma can spread to the skin and cause thickening or nodules. These would need to be distinguished from injection granulomas by carefully evaluating the patient’s medical history.
Knowledge iteration
Try out an evaluation of the body wall by reviewing this set of images with an online PACS viewer
- Starting with the body wall, evaluate the key muscular structures for any asymmetry or abnormal enhancement. Look at the anterior abdomen, paraspinal region, and pelvis.
- The muscular structures you should be familiar with include the following:
- rectus abdominus anteriorly
- oblique / transversus laterally
- paraspinal muscles posteriorly
- psoas muscles (flank both sides of the lumbar spine)
- iliopsoas muscles (heading into the pelvis)
- gluteus muscles posteriorly
- obturators
- upper thigh muscles
- Also look at the subcutaneous fat to make sure it is uniformly dark except for a few small vessels coursing through it.
This is an edited excerpt from the Medmastery course Abdominal CT Essentials by Michael P. Hartung, MD. Acknowledgement and attribution to Medmastery for providing course transcripts.
- Hartung MP. Abdominal CT: Common Pathologies. Medmastery
- Hartung MP. Abdominal CT: Essentials. Medmastery
- Hartung MP. Abdomen CT: Trauma. Medmastery
References
- Top 100 CT scan quiz. LITFL
Radiology Library: Abdominal CT: Imaging important abdominal structures
- Hartung MP. Abdominal CT: Checking the abdominal arteries
- Hartung MP. Abdominal CT: Checking the abdominal veins
- Hartung MP. Abdominal CT: Screening the lymph nodes
- Hartung MP. Abdominal CT: Evaluating the body wall
- Hartung MP. Abdominal CT: Evaluating the bones
- Hartung MP. Abdominal CT: Reporting checklist
Abdominal CT interpretation
Assistant Professor of Abdominal Imaging and Intervention at the University of Wisconsin Madison School of Medicine and Public Health. Interests include resident and medical student education, incorporating the latest technology for teaching radiology. I am also active as a volunteer teleradiologist for hospitals in Peru and Kenya. | Medmastery | Radiopaedia | Website | Twitter | LinkedIn | Scopus
MBChB (hons), BMedSci - University of Edinburgh. Living the good life in emergency medicine down under. Interested in medical imaging and physiology. Love hiking, cycling and the great outdoors.


