Automated Radiodiagnostic Security Entrance
UCEM‘s research boffins are perpetually pondering possible solutions for the great challenges facing Waiting Room Medicine. For example:
Violence in emergency departments is on the rise. Patients can possess all manner of potential weapons… machetes, firearms, smelly socks and even a hospital bed from time to time. Could such patients be immediately detected and disarmed on arrival, thus ensuring the safety of staff and other patients?
Since the advent of the four picosecond rule, the pressure on Waiting Room Medicine subspecialists to make early management and disposition decisions has been intense. But not every patient has obvious Signs of Imminent Admission or fits the admission criteria for a Patient Without Discernible Pathology. How can the diagnostic process be optimally accelerated?
Those of us that do not work in dyshopia face limited resources, constant bed shortages and understaffing. How can we ensure that valuable resources be distributed to only those that will benefit?
Patients with inconveniently placed foreign bodies dread protracted attempts at their removal…. as do the medical staff tasked with such extractions. Could there be some way of guaranteeing rapid removal without tying up medical staff unnecessarily?
Each one of these problems seems insurmountable.
If UCEM could find a solution for any of them we’d all be flabbergasted. But what if UCEM actually developed a single solution that solves them all?!
The solution is the ‘Automated Radiodiagnostic Security Entrance‘
Weapons and Violence
Early prototypes used metal detectors to identify armed patients, but the problem of actually removing the dangerous objects remained. Thanks to integrated MRI technology, UCEM’s new Automated Radio-diagnostic Security Entrance instantly detects AND removes metallic weapons with a minimum of fuss.
The photograph below demonstrates the utility of MRI in swiftly neutralising the threat posed by a malcontented bed-wielding geriatric patient:
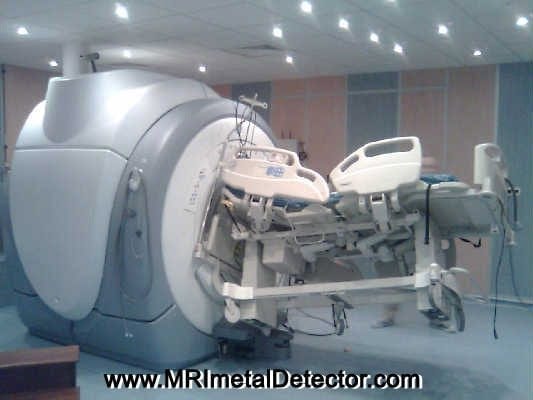
Rapid diagnosis
Patients entering through the Automatic Radiodiagnostic Security Entrance will be diagnosed by MRI even before they’re triaged or clerked. No longer will the astute Waiting Room physician have to rely on the Signs of Imminent Admission to make disposition decisions. Furthermore, all of a sudden, the four picosecond rule becomes a feasible target. Hallelujah!
Rapid removal of foreign bodies
As explained in ‘MRI — From Diagnostics to Therapeutics: Investigating new ways of removing metallic foreign bodies’ (a presentation at the UCEM Waiting Room Medicine Conference 2011) the Automatic Radiodiagnostic Security Entrance will be a boon to all those who subspecialise in foreign body-ectomies. Afflicted patients understandably want inconveniently situated foreign bodies extracted as soon as possible (atleast once the batteries have run out). Thanks to the powerful magnets lodged within the device, the Automatic Radiodiagnostic Security Entrance wastes no time in removing all things hard and shiny, and it does so by the most direct route…
Cost effective
Hospitals that decide to install this new technology in their waiting rooms will find it a cost effective way of distributing resources. Given the sizable initial outlay required to purchase an Automatic Radiodiagnostic Security Entrance, this statement may seem counter-intuitive. But remember that the sickest patients incur the greatest healthcare costs… and because critically ill patients rarely survive passage through an Automatic Radiodiagnostic Security Entrance, hospital coffers will soon be brimming with cash.
Design features
Note the following features:
- A capacious interior, will an uncannily inviting natural look.
- A well lubricated passageway to ensure the smooth transit of patients.
- A segmented structure that reduces obstructions to patient thoroughfare and a system of one-way valves preventing retrograde patient flow.
- An intuitive design that ensures that the exit is not mistaken for an entrance.
- Flame retardant outer materials that prevent your Automatic Radiodiagnostic Security Entrance from turning into a burning ring of fire should it fall victim to arsonists.
Yes, we’ve seen the future of Waiting Room Medicine…
It’s an Automated Radiodiagnostic Security Entrance.
UCEM Core Content
- Utopian College of Emergency for Medicine (UCEM)
- UCEM Publications and Position Statements
- UCEM Mission Statement and Essential Roles and Core Competencies
- About the Utopian College. Including Education; Examinations; and Collegial Hierarchy
- Utopian Medicine General News

Chris is an Intensivist and ECMO specialist at The Alfred ICU, where he is Deputy Director (Education). He is a Clinical Adjunct Associate Professor at Monash University, the Lead for the Clinician Educator Incubator programme, and a CICM First Part Examiner.
He is an internationally recognised Clinician Educator with a passion for helping clinicians learn and for improving the clinical performance of individuals and collectives. He was one of the founders of the FOAM movement (Free Open-Access Medical education) has been recognised for his contributions to education with awards from ANZICS, ANZAHPE, and ACEM.
His one great achievement is being the father of three amazing children.
On Bluesky, he is @precordialthump.bsky.social and on the site that Elon has screwed up, he is @precordialthump.
| INTENSIVE | RAGE | Resuscitology | SMACC
