Abdominal CT: Biliary system and Pancreas
Evaluating the biliary system and pancreas
The biliary system includes
- Gallbladder
- Intrahepatic bile ducts
- Common bile duct
- Pancreatic duct
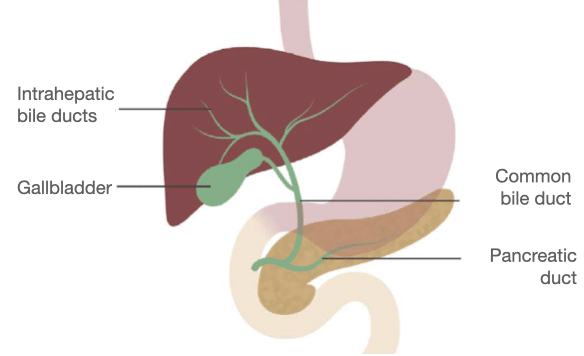
Gallbladder
A normal gallbladder will have a thin, barely perceptible wall, and will not appear dilated. The bile will look similar to fluid in density.
Some patients have calcified gallstones that are visible on CT and look like small bright dots. In the images shown next (middle image), we can see numerous small, calcified gallstones filling the gallbladder.
You may also encounter a patient with no gallbladder if it has been surgically removed. In this case, you will see clips near the cystic duct, which are bright on CT because they are made of metal.

Intrahepatic bile ducts
The bile ducts in the liver are normally very small and are often barely visible on CT. When they become mildly dilated, you will see thin, dark, tubular structures throughout the liver branching from the hepatic hilum. When they are severely dilated, it is hard to overlook them as they twist and branch throughout the liver, indicating biliary obstruction.

Common bile duct
The bile ducts inside the liver drain into the common hepatic duct, which joins with the cystic duct to become the common bile duct. It is helpful to evaluate the common hepatic and common bile ducts in their long axis on coronal images.
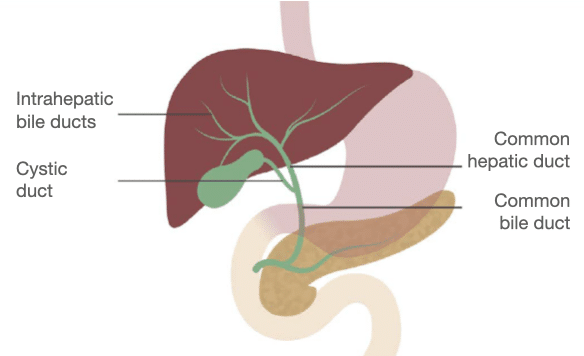
The normal common bile duct is smooth and measures about 6–7 mm or less in diameter. It commonly becomes a little dilated after the gallbladder is surgically removed. When it becomes obstructed, it can dilate to 10 mm or more.

Pancreatic duct
The major parts of the pancreas include the uncinate process, head, neck, body and tail
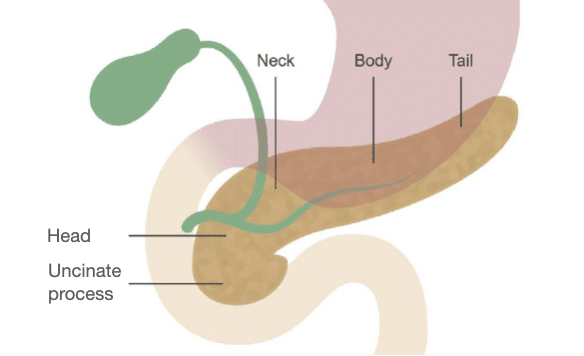
The common bile duct crosses the pancreas head and joins with the main pancreatic duct at the ampulla, where they then drain into the duodenum.

The normal pancreas enhances uniformly and has a thin (often barely perceptible) duct running through it. The pancreatic duct can become mildly dilated when obstruction or inflammation is present.
It can also become more severely dilated and lose normal pancreas tissue, which is referred to as atrophy. In cases like this, there may be a malignant mass causing obstruction. In the example below (on the right), pancreas ductal obstruction and atrophy is caused by a pancreas head adenocarcinoma.

Knowledge iteration
To solidify the core anatomy from the last two lessons, go through a search pattern of the liver, biliary system, and pancreas, by clicking on the image below to scroll through a set of images in a PACS viewer. The featured images show a normal CT appearance of the liver, biliary system, and pancreas. For a guided tour, please see this lesson’s video.

- Starting with the axial images and looking at the liver, you can evaluate the tissue for enhancement, contour, and masses.
- At the top of the liver, you can see the right, middle, and left hepatic veins. Notice that the main, right, and left portal veins are open.
- Next, take a look at the gallbladder, intrahepatic ducts, and common bile duct.
- The pancreas uncinate process, head, body, and tail have normal enhancement and contours, and the duct is small in caliber and normal.
- Notice the bright splenic vein along the back of the pancreas body and tail, and note how the pancreas tail points toward the spleen.
- The coronal images help us understand the relationship between the liver, portal vein, common bile duct, and pancreas. You can see the pancreas head, a segment of the normal duct in the neck and body, and you can follow the tail toward the spleen.
This is an edited excerpt from the Medmastery course Abdominal CT Essentials by Michael P. Hartung, MD. Acknowledgement and attribution to Medmastery for providing course transcripts.
- Hartung MP. Abdominal CT: Common Pathologies. Medmastery
- Hartung MP. Abdominal CT: Essentials. Medmastery
- Hartung MP. Abdomen CT: Trauma. Medmastery
References
- Top 100 CT scan quiz. LITFL
Radiology Library: Abdominal CT: Imaging the abdominal organs and bowel
- Hartung MP. Abdominal CT: Evaluating the liver
- Hartung MP. Abdominal CT: Evaluating the biliary system and pancreas
- Hartung MP. Abdominal CT: Imaging the spleen and adrenal glands
- Hartung MP. Abdominal CT: Mastering the genitourinary system
- Hartung MP. Abdominal CT: Evaluating the lower oesophagus and stomach
- Hartung MP. Abdominal CT: Imaging the small bowel
- Hartung MP. Abdominal CT: Viewing the peritoneal cavity
- Hartung MP. Abdominal CT: Running the large bowel and appendix
Abdominal CT interpretation
Assistant Professor of Abdominal Imaging and Intervention at the University of Wisconsin Madison School of Medicine and Public Health. Interests include resident and medical student education, incorporating the latest technology for teaching radiology. I am also active as a volunteer teleradiologist for hospitals in Peru and Kenya. | Medmastery | Radiopaedia | Website | Twitter | LinkedIn | Scopus
MBChB (hons), BMedSci - University of Edinburgh. Living the good life in emergency medicine down under. Interested in medical imaging and physiology. Love hiking, cycling and the great outdoors.


