Cullen sign
Cullen sign: superficial oedema with bruising in the subcutaneous fatty tissue around the peri-umbilical region. Originally described in association with ectopic pregnancy.
Cullen sign has been described in myriad clinical scenarios including acute pancreatitis; rectus sheath haematoma; massive ovarian enlargement; amoebic liver abscess; splenic rupture; perforated duodenal ulcer; metastatic thyroid cancer; intra-abdominal non-Hodgkin’s lymphoma and as a complication of anticoagulation.
History of the Cullen sign
1905 – Joseph Louis Ransohoff II described a man of fifty-three who presented a somewhat obscure abdominal condition. This was associated with jaundice of the umbilicus and of the umbilical region. At operation rupture of the common duct was found and the abdomen contained a large quantity of free bile. The abdominal wall was especially thin at the umbilicus, and the absorption of bile was clearly seen at this point.
1918 – Thomas Stephen Cullen first described a bluish black discoloration of the periumbilical skin in a female patient with a ruptured extrauterine pregnancy with ‘no history of injury‘
He concluded that the umbilical appearance was due to intra-abdominal haemorrhage secondary to an ectopic pregnancy. He originally described the finding at the 43rd annual meeting of the Transactions of the American gynecological society, Pennsylvania May 16-18, 1918
The patient, a woman, thirty-eight years of age, suddenly developed abdominal pain and distention. Dr. Cullen saw her three weeks later. The umbilical region was bluish black, although she gave no history of injury. Vaginal examination yielded nothing on account of the abdominal distention. Under ether, however, a mass 8 X 6 cm. was clearly felt to the right of the uterus. Dr. Cullen at once diagnosed extrauterine pregnancy, although the patient had missed no period and there was no uterine bleeding. On opening the abdomen he found a right-sided extrauterine pregnancy and about one and a half quarts of free blood in the abdomen.
Cullen TS 1918
Cullen expanded on this report in Contributions to Medical and Biological Research, a two volume tome dedicated to Sir William Osler on the occasion of his seventieth birthday on July 12, 1919.
Bearing Dr. Ransohoff’s 1905 case in mind I dictated the following note prior to opening the abdomen: “The bluish black appearance of the navel unassociated with any history of injury, together with the mass to the right of the uterus, makes the diagnosis of extrauterine pregnancy relatively certain.”
I record this case in order that subsequent ruptured extrauterine pregnancies may be examined for this sign. Whether it will prove to be of common occurrence or very rare, I cannot say, but we shall naturally expect it only where there is free blood in the abdomen and shall probably be more likely to encounter it in thin individuals.
Cullen TS 1919
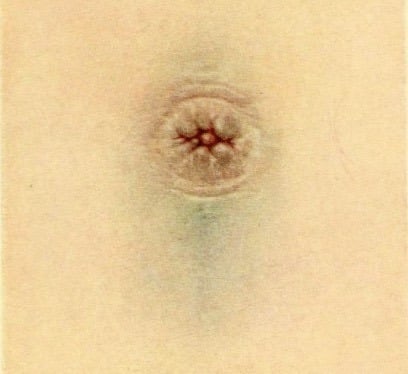
Cullen 1919: 420-422
Clinical context
Despite the original description, most literature relates Cullen sign of periumbilical ecchymosis to acute pancreatitis (being recorded in 1-3% cases) rather than secondary to an ectopic pregnancy.
In most described cases, it takes 3-5 days for Cullen sign to present and the sign been associated with a broad range of clinical conditions
| Cause | Reference |
|---|---|
| Retroperitoneal necrotizing fasciitis | Pryor et al 2001 |
| Strangulated umbilical hernia | Orient JM, Sapira JD 2005 |
| Strangulation of ileum with hemorrhage | Orient JM, Sapira JD 2005 |
| Renal sarcoma metastatic to the peritoneum | Orient JM, Sapira JD 2005 |
| Ovarian cyst hemorrhage | Orient JM, Sapira JD 2005 |
| Hypothyroid myopathy | Orient JM, Sapira JD 2005 |
| Hepatocellular carcinoma | Orient JM, Sapira JD 2005 |
| Cirrhosis with portal hypertension | Orient JM, Sapira JD 2005 |
| Bilateral acute salpingitis with IUP | Orient JM, Sapira JD 2005 |
| Hemorrhaging ascites from hepatic tumor | Mabin, Gelfand 1974 |
| Ischemic and gangrenous bowel | Kelley ML 1961 |
| Rectus sheath hematoma | Guthrie, Stanley 1996 |
| Perforated duodenal ulcer | Evans DM 1971 |
| Splenic rupture | Chung et al 1992 |
| Percutaneous liver biopsy | Capron et al 1977 |
| Acute Pancreatitis | Bosmann et al 2009 |
| Ruptured abdominal aortic aneurysm | Armour et al 1978 |
Epperla N, Mazza JJ, Yale SH. A Review of Clinical Signs Related to Ecchymosis. WMJ. 2015; 114(2): 61-65.
Associated Persons
- John Henry Bryant and Bryant sign (1903)
- Thomas Stephen Cullen and Cullen sign (1918)
- George Grey Turner and Grey Turner sign (1919)
- Francis Edward Stabler and Stabler Sign (1934)
- John Adrian Fox and Fox sign (1966)
Alternative names
- Cullen’s sign
- Peri-umbilical ecchymosis
Controversies
The topographic location of the ecchymosis of Grey Turner and Cullen do not point to the aetiology with any degree of certainty.
Cullen sign lacks sensitivity and specificity for its original description. It has been described in acute pancreatitis, rectus sheath haematoma, splenic rupture, perforated ulcer, intra-abdominal cancer, and ruptured ectopic pregnancy, and as a complication of anticoagulation [Am J Med. 2008]
References
Original articles
- Ransohoff J. Gangrene of the gall bladder: Rupture of the common bile duct, with new sign. Transactions of the Southern Surgical and Gynecological Association 1905; 18: 48-68
- Ransohoff J. Gangrene of the gall bladder: Rupture of the common bile duct, with new sign. JAMA 1906; 46(6): 395–397.
- Cullen TS. A new sign in ruptured extrauterine pregnancy. American journal of obstetrics and diseases of women and children. 1918; 78: 457
- Cullen TS. Bluish discolouration of the umbilicus as a diagnostic sign when ruptured extrauterine pregnancy exists. In: Contributions to Medical and Biological Research. 1919; 1: 420-422
Review articles
- Chung KM, Chuang SS. Cullen and Grey Turner signs in idiopathic perirenal hemorrhage. CMAJ. 2011 Nov 8;183(16):E1221
- Harris S, Naina HV. Cullen’s sign revisited. Am J Med. 2008; 121(8): 682-683.
- Rahbour G, Ullah MR, Yassin N, Thomas GP. Cullen’s sign – Case report with a review of the literature. Int J Surg Case Rep. 2012; 3(5): 143–146.
- McKennedy C. Cullen sign: Eponym A Day. Instagram
- Cadogan M. Non-traumatic Abdominal Ecchymosis. LITFL
eponymictionary
the names behind the name
MB BCh BAO, Queen’s Belfast. Recently moved to Australia, interested in Emergency Medicine, Medical Education and Paediatrics. Keen baker & tea drinker!
BA MA (Oxon) MBChB (Edin) FACEM FFSEM. Emergency physician, Sir Charles Gairdner Hospital. Passion for rugby; medical history; medical education; and asynchronous learning #FOAMed evangelist. Co-founder and CTO of Life in the Fast lane | On Call: Principles and Protocol 4e| Eponyms | Books |

