Left Posterior Fascicular Block (LPFB)
ECG Criteria
- Right axis deviation (RAD) (> +90 degrees)
- rS complexes in leads I and aVL
- qR complexes in leads II, III and aVF
- Prolonged R wave peak time in aVF
Note: The diagnosis of LFPB can only be made after excluding other causes of RAD. There should be:
- No evidence of right ventricular hypertrophy
- No evidence of any other cause for right axis deviation

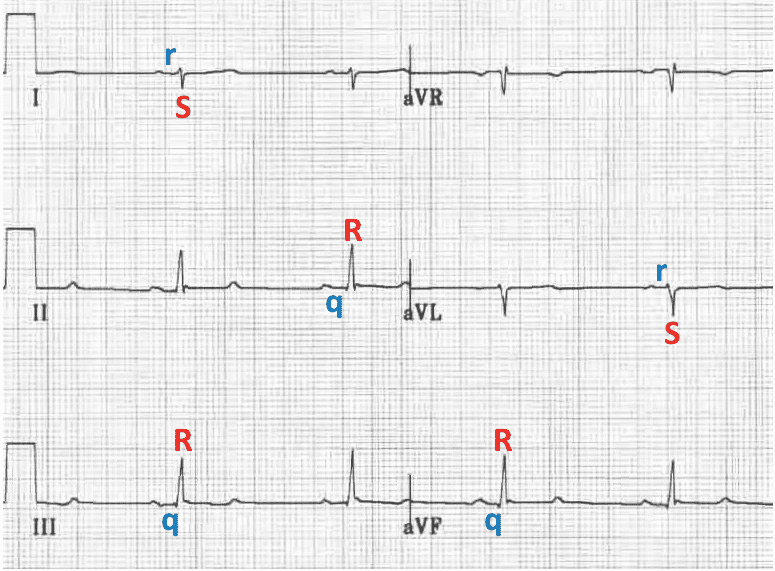
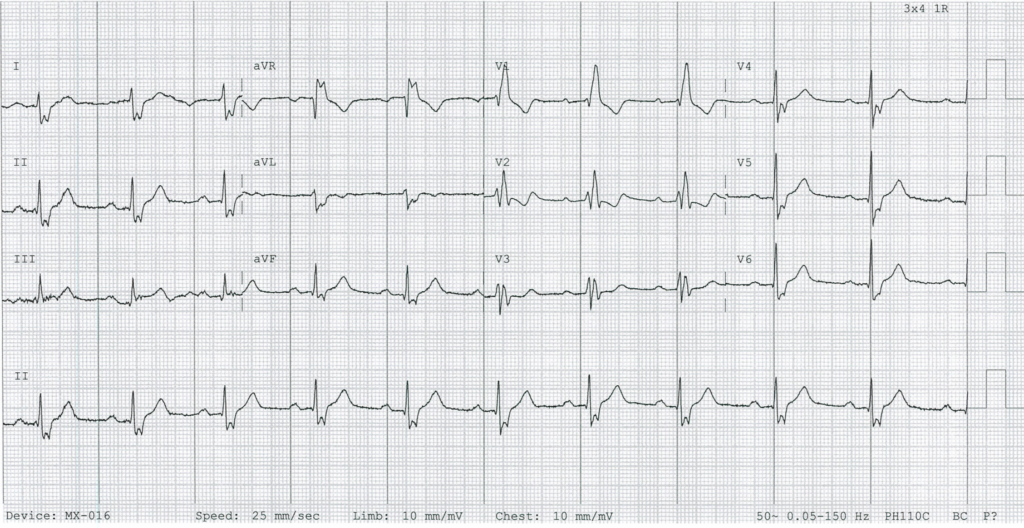
Typical ECG of LPFB, demonstrating slightly prolonged QRS duration, prolonged R wave peak time in aVF, and:
- rS complexes in leads I and aVL, with small R waves and deep S waves
- qR complexes in leads II, III and aVF, with small Q waves and tall R waves
- Right Axis Deviation (RAD): Leads II, III and aVF are POSITIVE; Leads I and aVL are NEGATIVE
Associated features include:
- QRS duration normal or slightly prolonged (80-110ms)
- Increased QRS voltage in limb leads
Electrophysiology
In LPFB, impulses are conducted to the left ventricle (LV) via the anterior fascicle, which inserts into the upper, lateral wall of the LV along its endocardial surface.
- Depolarisation spreads from endocardium to epicardium and thus the initial vector is directed upwards and leftwards, towards lateral leads. This produces small R waves in I and aVL, and small Q waves in inferior leads (II, III, aVF)
- The major wave of depolarisation then spreads along the free LV wall in a downward and rightward direction, producing tall R waves in inferior leads and deep S waves in the lateral leads.
- This process takes up to 20 milliseconds longer than simultaneous conduction via both fascicles, resulting in a slight widening of the QRS.
- Because impulses reaches the inferior leads later than normal, there is an increased R wave peak time in aVF (time from onset of QRS to peak of R wave)
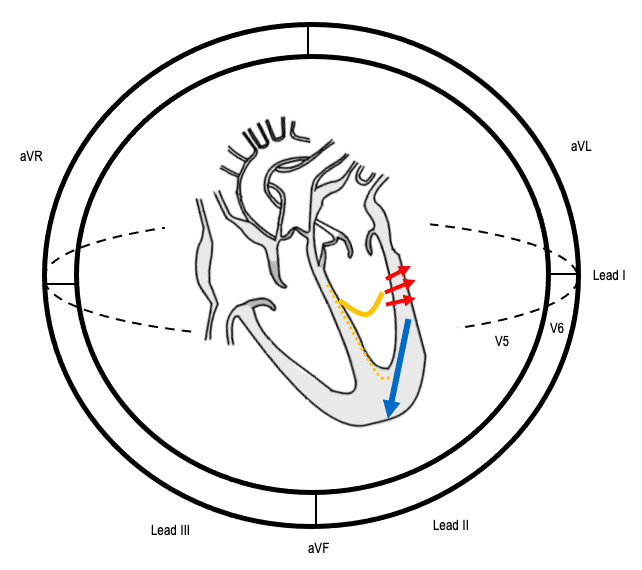
Sequence of conduction in LPFB
- YELLOW line: Impulses are conducted to the left ventricle only via the anterior fascicle
- RED arrow: Initial depolarisation vector is directed towards lateral leads
- BLUE arrow: Major depolarisation vector, which is slightly delayed, is directed towards inferior leads
Example ECG
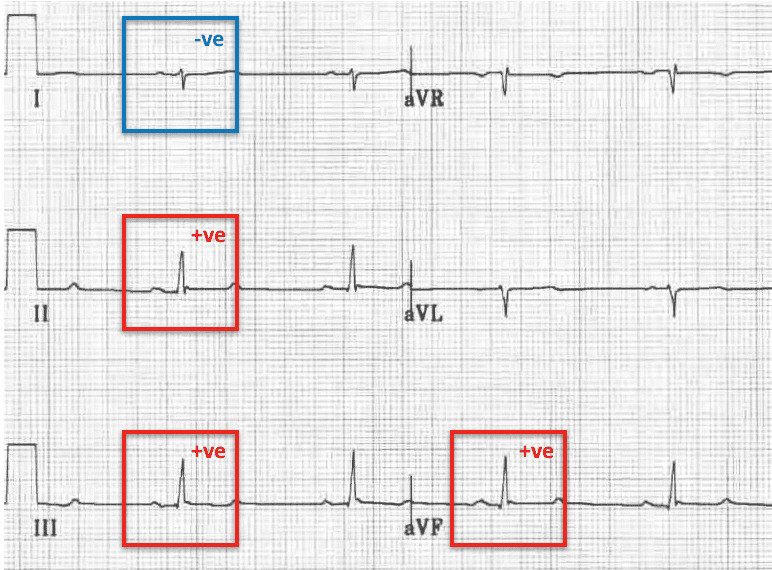
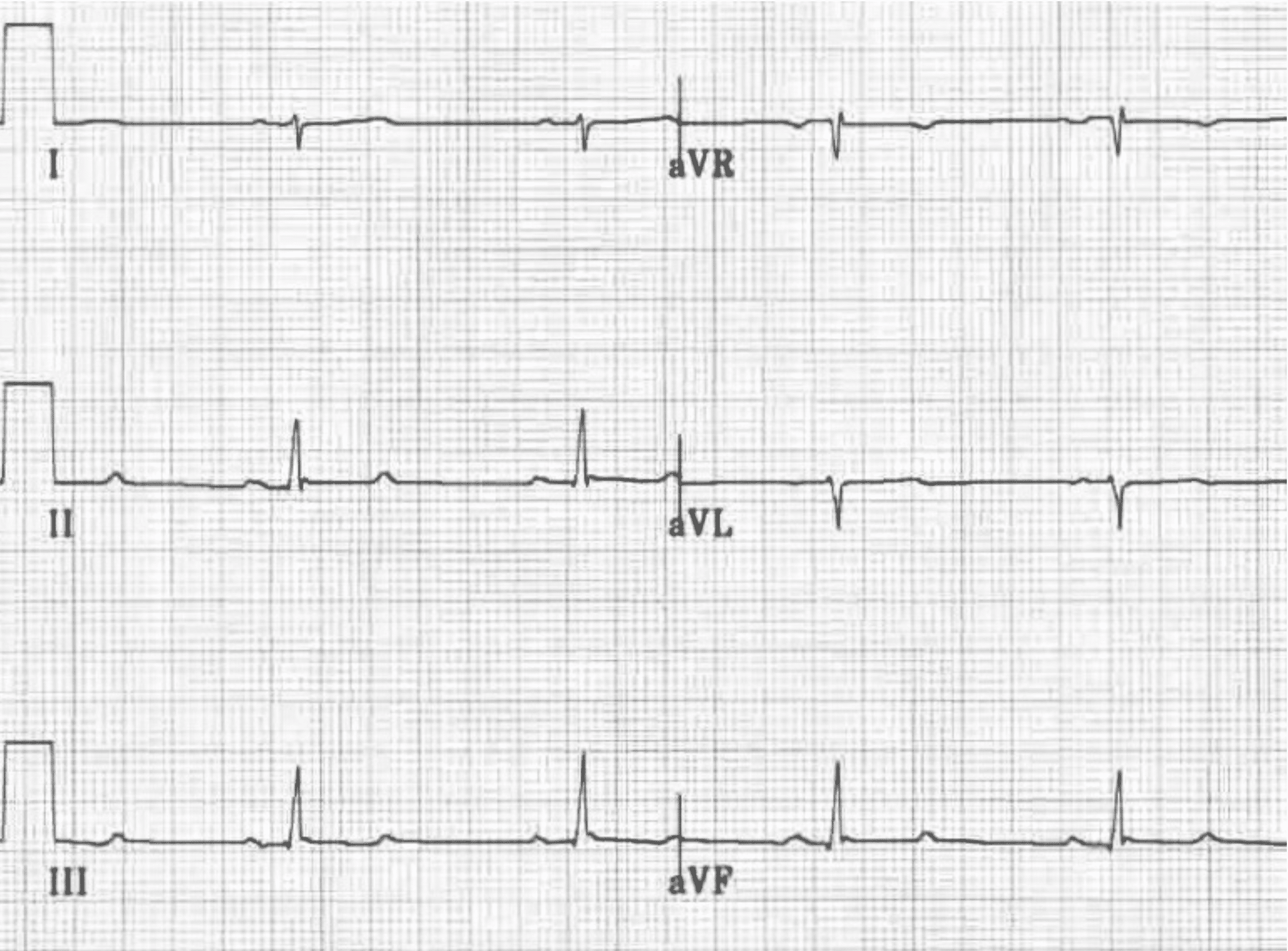
- As above, there are rS complexes in leads I and aVL, and qR complexes in leads II, III and aVF
Right Axis Deviation (RAD)
- Leads II, III and aVF are POSITIVE;
- Leads I and aVL are NEGATIVE
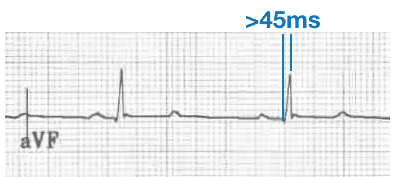
Prolonged R-wave peak time
- R-wave peak time: Time from onset of the QRS to the peak of the R wave in aVF > 45 ms
Handy Tips
- LPFB is much less common than LAFB, as the broad bundle of fibres that comprise the left posterior fascicle are relatively resistant to damage when compared with the slim single tract that makes up the left anterior fascicle.
- It is extremely rare to see LPFB in isolation. It usually occurs along with RBBB in the context of a bifascicular block.
- Do not be tempted to diagnose LPFB until you have ruled out more significant causes of right axis deviation: Example: acute pulmonary embolus; tricyclic overdose; lateral STEMI; and right ventricular hypertrophy.
ECG Examples of LPFB
Example 1
Example 2
Example 3
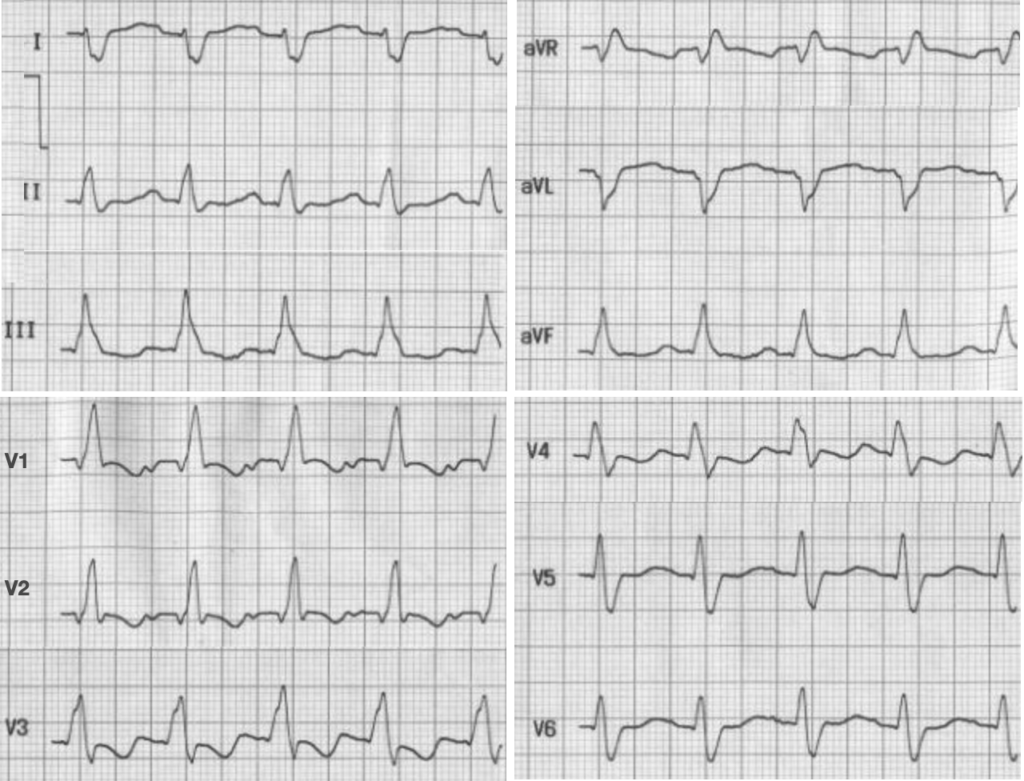
RBBB with LPFB
- RBBB with wide QRS, slurred S wave in lead I and slurred R in V1.
- Right axis deviation (dominant negative deflection in leads I and aVl) with dominant positive deflection in aVf along with rS pattern in lead I and qR pattern leads III and aVf, suggesting left posterior fascicular block.
Example 3b
RBBB with LPFB and RAD
Related Topics
- Left bundle branch block LBBB
- Right Bundle Branch Block RBBB
- Left anterior fascicular block LAFB
- Left posterior fascicular block LPFB
- Interventricular Conduction Delay IVCD
- Bifascicular block
- Trifascicular block
- Complete Heart block CHB
Advanced Reading
Online
- Wiesbauer F, Kühn P. ECG Mastery: Yellow Belt online course. Understand ECG basics. Medmastery
- Wiesbauer F, Kühn P. ECG Mastery: Blue Belt online course: Become an ECG expert. Medmastery
- Kühn P, Houghton A. ECG Mastery: Black Belt Workshop. Advanced ECG interpretation. Medmastery
- Rawshani A. Clinical ECG Interpretation ECG Waves
- Smith SW. Dr Smith’s ECG blog.
- Wiesbauer F. Little Black Book of ECG Secrets. Medmastery PDF
Textbooks
- Zimmerman FH. ECG Core Curriculum. 2023
- Mattu A, Berberian J, Brady WJ. Emergency ECGs: Case-Based Review and Interpretations, 2022
- Straus DG, Schocken DD. Marriott’s Practical Electrocardiography 13e, 2021
- Brady WJ, Lipinski MJ et al. Electrocardiogram in Clinical Medicine. 1e, 2020
- Mattu A, Tabas JA, Brady WJ. Electrocardiography in Emergency, Acute, and Critical Care. 2e, 2019
- Hampton J, Adlam D. The ECG Made Practical 7e, 2019
- Kühn P, Lang C, Wiesbauer F. ECG Mastery: The Simplest Way to Learn the ECG. 2015
- Grauer K. ECG Pocket Brain (Expanded) 6e, 2014
- Surawicz B, Knilans T. Chou’s Electrocardiography in Clinical Practice: Adult and Pediatric 6e, 2008
- Chan TC. ECG in Emergency Medicine and Acute Care 1e, 2004
LITFL Further Reading
- ECG Library Basics – Waves, Intervals, Segments and Clinical Interpretation
- ECG A to Z by diagnosis – ECG interpretation in clinical context
- ECG Exigency and Cardiovascular Curveball – ECG Clinical Cases
- 100 ECG Quiz – Self-assessment tool for examination practice
- ECG Reference SITES and BOOKS – the best of the rest
ECG LIBRARY
Emergency Medicine Specialist MBChB FRCEM FACEM. Medical Education, Cardiology and Web Based Resources | @jjlarkin78 | LinkedIn |
MBBS DDU (Emergency) CCPU. Adult/Paediatric Emergency Medicine Advanced Trainee in Melbourne, Australia. Special interests in diagnostic and procedural ultrasound, medical education, and ECG interpretation. Co-creator of the LITFL ECG Library. Twitter: @rob_buttner