Tick Paralysis
OVERVIEW
Tick paralysis is a rare life-threatening disorder caused by envenoming from ixodid tick bites
- can cause respiratory paralysis
- less than 5 cases of severe envenoming each year in Australia
- no deaths in Australia since 1945 and the advent of improved respiratory support
CAUSE
Only 3 species of ixodid or ‘hard’ tick (out of over 70 species in Australia) cause tick paralysis:
- Ixodes holocyclus
- Ixodes hirsti
- Ixodes cornuatus

Venom
- Ixodid tick saliva contains neurotoxins and various agents that modulate the hemostatic and inflammatory responses of the host
- I. holocyclus neurotoxins are ~ 5 kDa proteins known as holocyclotoxins that prevent acetylcholine release from presynaptic nerve terminals
Transmission
- Both male and female adult ticks attach onto humans
- Ticks find a host by ‘questing‘ — they climb up vegetation waiting for host to pass by
- Natural hosts in Australia include bandicoots, koalas, possums and kangaroos
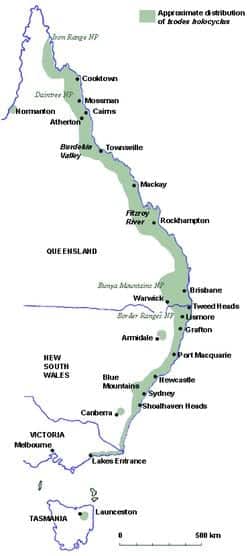
Distribution
- confined to the bush and scrub lands near the eastern coast of Australia, from North Queensland to Victoria
- also reported in Tasmania
Tick paralysis also occurs in many other parts of the world where members of the Ixodidae family are found:
- Dermacentor andersoni — Western United States and Canada (British Columbia)
- D. variabilis — Central and Eastern United States
- Ixodes holocyclusand I. hirsti — Eastern Australia
- I. cornuatus — Tasmania (Australia)
- I. tancitarius — Mexico
- I. rubicundus — Africa
- Rhipicephalus simus — South Africa, Somalia
- R. evertsi evertsi — Africa
CLINICAL MANIFESTATIONS
Severe toxicity and death is usually seen in children under the age of 3 years
- onset of symptoms is usually 4-5 days after tick attachment
- there may be local itch and swelling at the tick attachment site. Local nerve palsies (e.g. CN7 palsy) may occur in proximity to the tick attachment site. Allergic reactions may occur
- systemic toxicity is heralded by a nonspecific prodrome of ataxia (unsteady gait) and drowsiness or lethargy
- a progressive ascending symmetrical flaccid paralysis occurs over a period of days
- eventually cranial nerve palsies occur — typically ptosis, extraocular palsies, CN7 palsies, dysphagia and impaired airway reflexes
- death may result following the onset of respiratory paralysis
In the Australian setting, paralysis may progress for about 2 days following the removal of the tick in the symptomatic patient.
INVESTIGATIONS
- diagnosis is made clinically
MANAGEMENT
Resuscitation
- Life threats include loss of airway reflexes and respiratory paralysis
- Intubation and ventilation may be required, and once performed is usually continued for day to weeks
Removal of the tick as soon as possible
- use fine forceps or suture material to grasp the tick’s mouth parts close to the skin at the site of attachment
- Remove the tick, with mouth-parts intact, by carefully applying steady traction
- Don’t worry about twisting clockwise or anti-clockwise!
- ensure that there are no retained mouth-parts, which may lead to granuloma formation
- it is controversial whether the tick should be killed before removal, due to concerns about toxin release during removal
Supportive care and monitoring
- Spirometry or serial peak expiratory flow monitory may be used to monitor the progression of respiratory paralysis
- Regular neurological observations
Antidote
- CSL Tick paralysis antivenom is no longer available for use in humans
Disposition
- Patients with the potential for respiratory failure require HDU/ ICU level care
- Symptomatic patients should not be discharged until ongoing neurological recovery is observed
- The asymptomatic patients does not need to be admitted for observation following the removal of a tick!
References and Links
CCC Toxicology Series
General
Approach to acute poisoning, ECGs in Tox, Evidenced-based Tox, Toxicology literature summaries, Does anti-venom work?
Toxins / Overdose
Amphetamines, Barbituates, Benzylpiperazine, Beta Blockers, Calcium Channel Blocker, Carbamazepine, Carbon Monoxide, Ciguatera, Citrate, Clenbuterol, Cocaine, Corrosive ingestion, Cyanide, Digoxin, Ethanol, Ethylene Glycol, Iron, Isoniazid, Lithium, Local anaesthetic, Methanol, Monoamine oxidase inhibitor (MAOI), Mushrooms (non-hallucinogenic), Opioids, Organophosphate, Paracetamol, Paraquat, Plants, Polonium, Salicylate, Scombroid, Sodium channel blockers, Sodium valproate, Theophylline, Toxic alcohols, Tricyclic antidepressants (TCA)
Envenomation
Marine, Snakebite, Spider, Tick paralysis
Syndromes
Alcohol withdrawal, Anticholinergic syndrome, Cholinergic syndrome, Drug withdrawals in ICU, Hyperthermia associated toxidromes, Malignant hyperthermia (MH), Neuroleptic malignant syndrome (NMS), Opioid withdrawal, Propofol Infusion Syndrome (PrIS) Sedative toxidrome, Serotonin syndrome, Sympatholytic toxidrome, Sympathomimetic toxidrome
Decontamination
Activated Charcoal, Gastric lavage, GI Decontamination
Enhanced Elimination
Enhanced elimination, Hyperbaric therapy for CO
Antidotes
Antidote summary, Digibind, Glucagon, Flumazenil, HIET – High dose euglycaemic therapy, Intralipid, Methylene Blue, N-Acetylcysteine (NAC), Naloxone
Miscellaneous
Cocaine chest pain, Digoxin and stone heart theory, Hyperbaric oxygen, Hypoxaemia in tox, Liver failure in tox, Liver transplant for paracetamol, Methaemoglobinaemia, Urine drug screen
LITFL
- Toxicology Conundrum 039 — Paralysis and a head lump
Journal articles and textbooks
- Brown AF, Hamilton DL. Tick bite anaphylaxis in Australia. J Accid Emerg Med. 1998 Mar;15(2):111-3. PMC1343038.
- Edlow JA, McGillicuddy DC. Tick paralysis. Infect Dis Clin North Am. 2008 Sep;22(3):397-413, vii. PMID: 18755381.
- Grattan-Smith PJ, Morris JG, Johnston HM, Yiannikas C, Malik R, Russell R, Ouvrier RA. Clinical and neurophysiological features of tick paralysis. Brain. 1997 Nov;120 ( Pt 11):1975-87. PMID: 9397015.

Critical Care
Compendium
Chris is an Intensivist and ECMO specialist at The Alfred ICU, where he is Deputy Director (Education). He is a Clinical Adjunct Associate Professor at Monash University, the Lead for the Clinician Educator Incubator programme, and a CICM First Part Examiner.
He is an internationally recognised Clinician Educator with a passion for helping clinicians learn and for improving the clinical performance of individuals and collectives. He was one of the founders of the FOAM movement (Free Open-Access Medical education) has been recognised for his contributions to education with awards from ANZICS, ANZAHPE, and ACEM.
His one great achievement is being the father of three amazing children.
On Bluesky, he is @precordialthump.bsky.social and on the site that Elon has screwed up, he is @precordialthump.
| INTENSIVE | RAGE | Resuscitology | SMACC
