ECG Exam Template
The following headings and prompts can be used as template for ECG-based exam questions.
Amjid Rehman (@amjidrehman) has made an easy interactive online template ‘ECG made easier‘ based on the template structure outlined
ECG type and recording
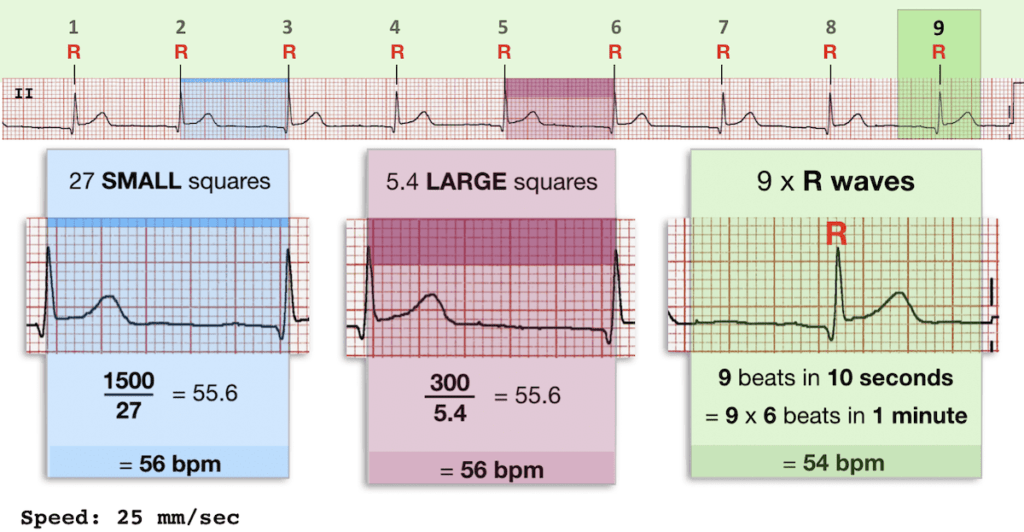
- 12 lead vs rhythm strip, rate (normal 25 mm/s)
- Calibration (5mm wide, 10mm high = 1mV)
- Unusual leads – right, posterior, lead grouping format
Rate
- normal 60 – 100/min
- tachy/bradycardia (SA node) vs –arrhythmia (not SA node)
- method: 300/RR interval (large squares) or number of QRS complexes x 6 (if 25mm/s)
Rhythm
- Pattern – regular/ regularly irregular/ irregularly irregular
- Seven step approach to rhythm analysis
Axis
Axis Methods:
- Quick look test (Lead I and aVF)
- Three Lead Analysis (Lead I, Lead II, aVF)
- Isoelectric Lead Analysis
- Super SAM the axis Man
P wave
- Present? (esp check II and V1)
- Amplitude + duration: normal <3mm high and wide (LAE/RAE/Biatrial)
- Contour: normal — inverted aVR, biphasic V1, upright I,II, aVF, V2-V6
PR interval + PR segment
- Duration 0.12-0.2s normal/ short/ long/ varying
- Heart blocks:
- PR depression
Q wave
- Normal: <25%R in I, aVL, AVF, V456
- Pathological: V23 > 0.02s, other >0.03s + >1mm deep
R wave
- Transition: normal V34, early: R>S in V1/2
- Poor R Wave Progression: R <3mm V3
QRS complex
- Duration: 60-110msec normal/ wide; R wave peak time
- Amplitude: normal/ large voltage/ low voltage/ alternans
- Morphology: notched/ RBBB/ LBBB
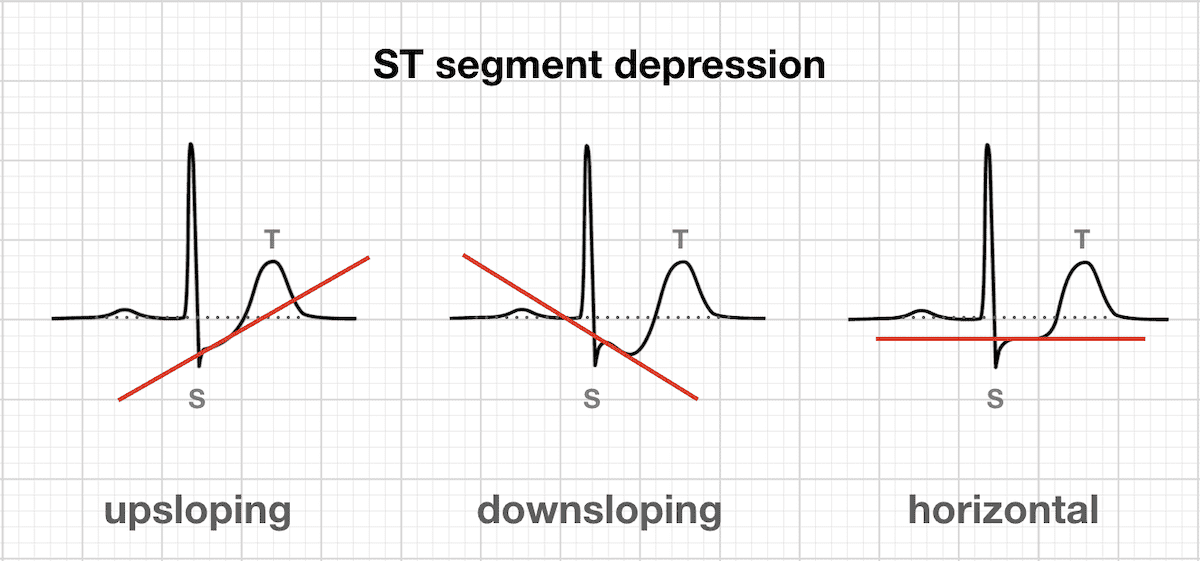
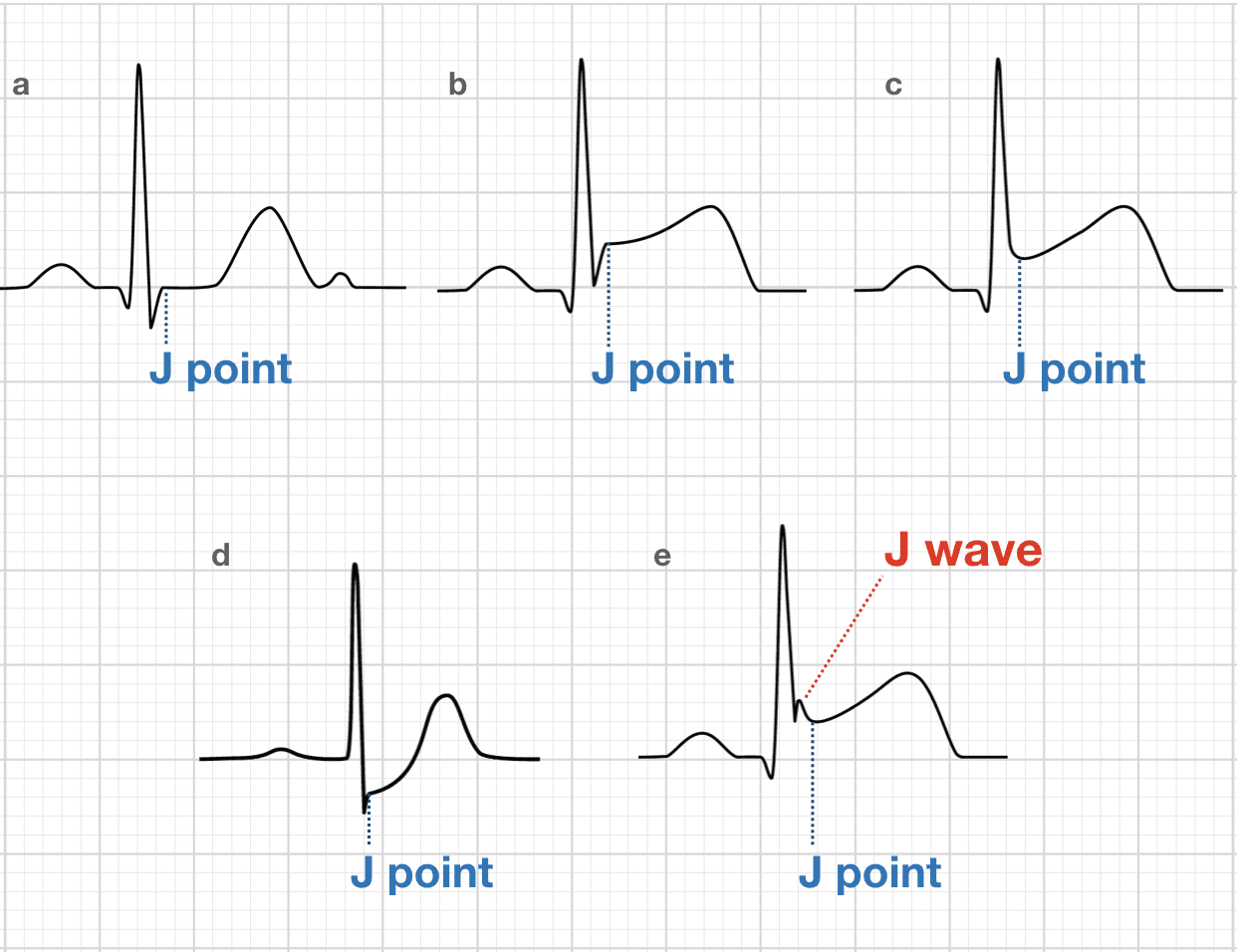
- Displacement: elevation/ depression (J point vs TP interval)
- Contour: horizontal /upsloping / downsloping
T wave
- Amplitude: normal <2/3 R/ peaked/ inversion/ alternans
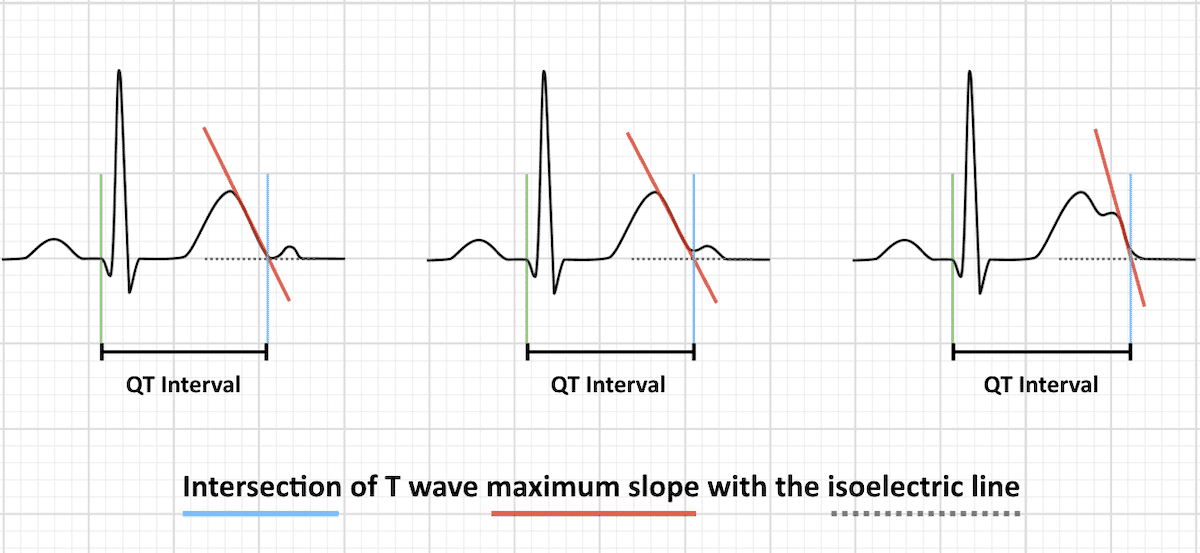
- Duration: normal 390-450 or 460msec / long/ short/ QT dispersion
- Method, 3+ QRS in 3+ leads, QTc formulae, caveats
U wave
- Normal 10% T or <1.5mm/ prominent/ inversion/ alternans
Additional waves
- DOE: Delta wave, Osborn wave, Epsilon Wave
Chamber hypertrophy
Lethal – do not miss!
- Ischaemia – STE criteria and DDX/ Sgarbossa/ reciprocal change/ Wellens/ aVR
- Quick BRAD Walk Home! Lethal causes of syncope:
- Pulmonary Embolus
- Electrolytes: hyperK, hypoK, hypoCa, hyperCa, hypoMg
- Toxicology: TCAs, digoxin
Other tricks and traps
- Dextrocardia, Lead reversals
- Artifacts – tremor artifact
- Pacing spikes – pacemaker malfunction: failure to sense/ capture/ output?
Synthesis
- Leave space to put this at the start of the answer
- Unifying diagnosis, DDx, life threats
Advanced Reading
Online
- Wiesbauer F, Kühn P. ECG Mastery: Yellow Belt online course. Understand ECG basics. Medmastery
- Wiesbauer F, Kühn P. ECG Mastery: Blue Belt online course: Become an ECG expert. Medmastery
- Kühn P, Houghton A. ECG Mastery: Black Belt Workshop. Advanced ECG interpretation. Medmastery
- Rawshani A. Clinical ECG Interpretation ECG Waves
- Smith SW. Dr Smith’s ECG blog.
- Wiesbauer F. Little Black Book of ECG Secrets. Medmastery PDF
Textbooks
- Zimmerman FH. ECG Core Curriculum. 2023
- Mattu A, Berberian J, Brady WJ. Emergency ECGs: Case-Based Review and Interpretations, 2022
- Straus DG, Schocken DD. Marriott’s Practical Electrocardiography 13e, 2021
- Brady WJ, Lipinski MJ et al. Electrocardiogram in Clinical Medicine. 1e, 2020
- Mattu A, Tabas JA, Brady WJ. Electrocardiography in Emergency, Acute, and Critical Care. 2e, 2019
- Hampton J, Adlam D. The ECG Made Practical 7e, 2019
- Kühn P, Lang C, Wiesbauer F. ECG Mastery: The Simplest Way to Learn the ECG. 2015
- Grauer K. ECG Pocket Brain (Expanded) 6e, 2014
- Surawicz B, Knilans T. Chou’s Electrocardiography in Clinical Practice: Adult and Pediatric 6e, 2008
- Chan TC. ECG in Emergency Medicine and Acute Care 1e, 2004
LITFL Further Reading
- ECG Library Basics – Waves, Intervals, Segments and Clinical Interpretation
- ECG A to Z by diagnosis – ECG interpretation in clinical context
- ECG Exigency and Cardiovascular Curveball – ECG Clinical Cases
- 100 ECG Quiz – Self-assessment tool for examination practice
- ECG Reference SITES and BOOKS – the best of the rest
ECG LIBRARY
Chris is an Intensivist and ECMO specialist at The Alfred ICU, where he is Deputy Director (Education). He is a Clinical Adjunct Associate Professor at Monash University, the Lead for the Clinician Educator Incubator programme, and a CICM First Part Examiner.
He is an internationally recognised Clinician Educator with a passion for helping clinicians learn and for improving the clinical performance of individuals and collectives. He was one of the founders of the FOAM movement (Free Open-Access Medical education) has been recognised for his contributions to education with awards from ANZICS, ANZAHPE, and ACEM.
His one great achievement is being the father of three amazing children.
On Bluesky, he is @precordialthump.bsky.social and on the site that Elon has screwed up, he is @precordialthump.
| INTENSIVE | RAGE | Resuscitology | SMACC